What Is a Diabetic Foot Surgery?
Diabetic foot surgery is a procedure performed to treat severe foot problems caused by diabetes. When high blood sugar damages blood vessels and nerves, it can lead to poor healing, infections, ulcers, and in some cases, tissue death.
These diabetic foot surgery procedure helps remove infected tissue, improve blood flow, and prevent further complications. The main goal is to save the foot, restore function, and reduce the risk of amputation. Depending on the condition, doctors may perform wound cleaning, reconstructive surgery, or bypass procedures to improve circulation.
By treating the underlying problem, diabetic foot surgery gives patients a better chance of healing and helps them return to a more active, pain-free life.
Types of Diabetic Foot Surgery
Diabetic foot surgery is not the same for every person. The type of surgery depends on the severity of the foot problem, blood flow, and infection level. Diabetic foot surgery types:
- Debridement Surgery: Removes dead or infected tissue to promote healing.
- Drainage of Abscess: Opens and cleans infected pockets of pus in the foot.
- Reconstructive Surgery: Corrects deformities, improves foot shape, and prevents future ulcers.
- Vascular Surgery: Restores blood circulation through bypass or angioplasty, helping wounds heal faster.
- Amputation (when necessary): Performed only in severe cases to stop the spread of infection and save the patient's life.
These surgeries aim to protect the foot, improve recovery, and reduce the risk of serious complications.
1 to 3 hours
Surgery Duration
Local, Regional, or General Anesthesia, based on the procedure
Anesthesia Used
2 to 5 days
Hospital Stay
6 to 12 weeks
Full Recovery Timeline
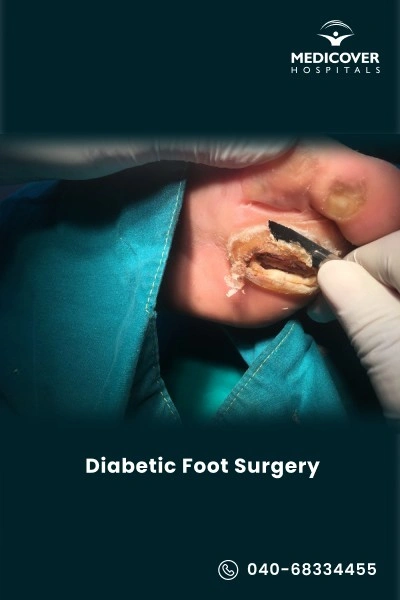
When is Diabetic Foot Surgery Recommended?
Diabetic foot surgery is usually recommended when non-surgical treatments like medicines, dressings, or lifestyle changes do not heal the problem. It becomes necessary if there is severe infection, poor blood flow, or tissue damage that puts the foot at risk.
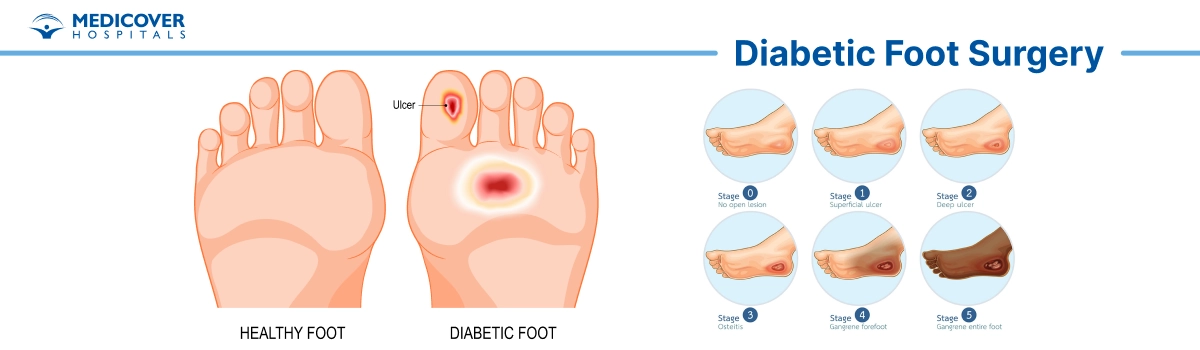
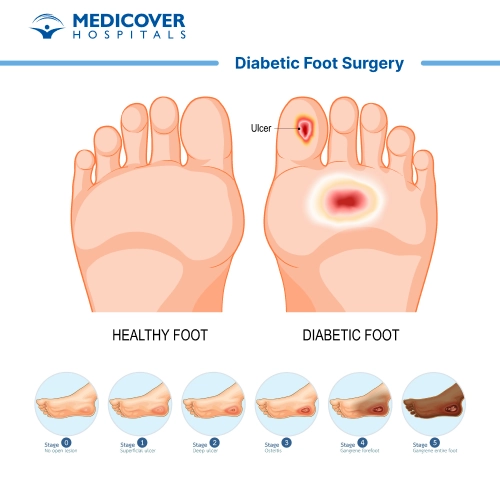
Doctors may suggest surgery in cases such as:
- Non-healing Ulcers: Diabetic foot ulcers that do not respond to conservative wound care measures, such as dressing changes, offloading, and antibiotic therapy, may require surgical intervention to remove necrotic tissue, improve blood flow, and promote wound healing.
- Infections: Severe infections, such as osteomyelitis (bone infection) or cellulitis (soft tissue infection), may necessitate surgical drainage or debridement to remove infected tissue and prevent the spread of infection.
- Charcot Neuroarthropathy: This condition occurs due to nerve damage, leading to fractures, instability, and deformities. Surgical realignment and stabilisation may be necessary to prevent further damage.
- Gangrene: Gangrene, which is the death of tissue due to poor blood circulation, may require surgical removal of the affected tissue to prevent the spread of infection.
- Deformities: Foot deformities, such as hammertoes, bunions, or claw toes, can cause pressure points that lead to ulcers. Surgical correction of these deformities can help alleviate pressure and reduce the risk of ulcers.
- Peripheral Arterial Disease (PAD): Severe PAD can lead to reduced blood flow to the feet, increasing the risk of ulcers and infections. Angioplasty and bypass surgery are examples of revascularization procedures that may be performed to restore blood flow.
- Peripheral Neuropathy: Nerve damage in the feet can lead to loss of sensation and decreased muscle function, increasing the risk of ulcers and deformities. Surgical interventions may include tendon transfers or releases to correct imbalances and improve foot function.
- Necrotizing Fasciitis: This is a rapidly progressing soft tissue infection that requires aggressive surgical debridement to remove infected tissue and prevent its spread.
- Foot Amputation: In severe cases where other interventions have failed and there is a risk of life-threatening infection, partial or complete foot amputation may be necessary to save the patient's life.
The main aim of surgery is to save the foot, reduce pain, and prevent major complications like amputation.
Preparing for the Diabetic Foot Surgery Procedure
Getting ready for diabetic foot surgery is an important step in ensuring a safe procedure and smooth recovery. Our diabetic foot surgery doctor will guide you through the process, but a little preparation can make a big difference.
Before surgery, you may be asked to:
- Review your medications: Some medicines, like blood thinners, may need to be adjusted before the procedure.
- Manage blood sugar levels: Keeping your blood sugar under control helps the healing process.
- Complete routine tests: Blood work, imaging, or other tests may be done to check your overall health.
- Follow fasting instructions: If general anesthesia will be used, your doctor will tell you when to stop eating and drinking before surgery.
- Arrange support at home: Having a family member or friend to help after surgery can make recovery easier.
Taking these steps helps lower risks and prepares your body for healing. Always follow your healthcare team's advice closely for the best outcome.
What Happens During Diabetic Foot Surgery?
Diabetic foot surgery procedures are performed with the primary goal of treating complications related to diabetic foot ulcers, infections, deformities, and other issues that may arise due to diabetes. The specific procedure performed depends on the individual's condition and the severity of the problem.
- Preparation & Anesthesia: Before surgery, the doctor explains the procedure and answers your questions. In the operation room, anesthesia is given so you feel no pain. It may be local, regional, or general depending on your condition.
- Incisions & Cleaning: The surgeon makes a small cut on the affected area of the foot. Infected or dead tissue is removed, and the wound is cleaned to stop infection from spreading.
- Improving Blood Flow: If poor circulation is slowing healing, a vascular procedure like bypass or angioplasty may be done. This helps blood flow better and speeds recovery.
- Reconstructive Surgery: If foot shape or ulcers cause repeated wounds, reconstructive steps are taken. This reduces pressure points and helps prevent new ulcers.
- Closing the Wound: Once cleaned, the wound is closed with stitches or covered with a special dressing. In some cases, skin grafts may be needed.
- Drainage & Dressing: A small drain may be placed to remove extra fluid. The foot is then covered with clean dressings and supported for healing.
- Post-Surgery Care: After surgery, you are moved to recovery. Doctors monitor your healing, blood sugar, and wound condition. Gentle movement is encouraged to improve circulation and support recovery.
Recovery After Diabetic Foot Surgery?
Recovering from diabetic foot surgery takes time & careful follow-up, but each step helps you move closer to healing and regaining mobility.
First Few Days After Surgery
In the first few days, it's normal to experience swelling, soreness, and some discomfort in the foot. Your doctor will keep the wound dressed and may use drains to avoid fluid buildup.
Gentle movement, like short walks, is encouraged to improve blood flow and speed healing.
Doctor's Tip: "Keep your foot clean and dry, and follow dressing change instructions carefully to lower the risk of infection."
Weeks 2 to 4
By weeks 2 to 4, pain and swelling begin to settle. You may be able to walk short distances with support or a walking aid, depending on the surgery. Wound checks and dressing changes remain important during this period.
Doctor's Tip: "Always wear protective footwear or support as advised-it reduces pressure on the foot and helps prevent new ulcers."
Weeks 5 to 6
At this stage, you may notice gradual improvement in mobility. Many patients return to light daily tasks, but heavy work or long walks should still be avoided. Your doctor may suggest physical therapy to restore strength and balance.
Doctor's Tip: "Even if you feel better, avoid putting full weight on the foot until your surgeon confirms it's safe."
3 to 6 Months After Surgery
By this time, most of the healing is complete. Swelling reduces further, wounds close, and walking becomes more comfortable. With proper care and diabetes control, long-term results improve, and the risk of recurrence decreases.
Doctor's Tip: "Good blood sugar control is as important as surgery itself-it helps your foot heal and stay healthy."
Benefits of Diabetic Foot Surgery
- Helps Wounds Heal Faster: The surgery removes dead or infected tissue, giving the foot a better chance to recover.
- Improves Blood Circulation: When blood flow is restored, pain reduces and healing becomes quicker.
- Prevents Serious Complications: Surgery lowers the chance of gangrene and reduces the risk of major amputation.
- Better Quality of Life: Healing of the foot brings comfort, independence, and confidence back to daily living.
Risks of Diabetic Foot Surgery
Even though surgery can be life-saving, there are some risks to keep in mind:
- Infection
- Slow wound healing
- Bleeding
- Scarring
- Numbness or reduced sensation
- Blood clots
- Poor circulation slowing recovery
- Possibility of partial or complete amputation in severe cases
How much does diabetic foot treatment cost?
The diabetic foot surgery cost usually depends on the type of procedure, the severity of the condition, and the hospital facilities. At Medicover Hospital, the price typically ranges between Rs. 40,000 to Rs. 4,45,000.