| Do’s | Don’ts |
|---|---|
|
Take rest |
Ignore osteomyelitis symptoms |
|
Keep diabetes under control |
Gain weight |
|
Eat healthy food |
Smoke and consume alcohol |
|
Prevent falls |
Do strenuous physical activities |
|
Regular health check-up |
Eat processed and junk foods |
Osteomyelitis: Causes, Symptoms and Treatment Options
Osteomyelitis (OM) is a bone infection. It is an inflammation or swelling of bone tissue. The infection can spread to a bone by spreading through the blood circulation or from nearby infected tissues. Bone infection can also occur if an injury exposes the bone to germs.
Osteomyelitis can either be acute (of recent onset) or chronic (longstanding). There can be numerous causes of osteomyelitis, which can affect both children and adults.
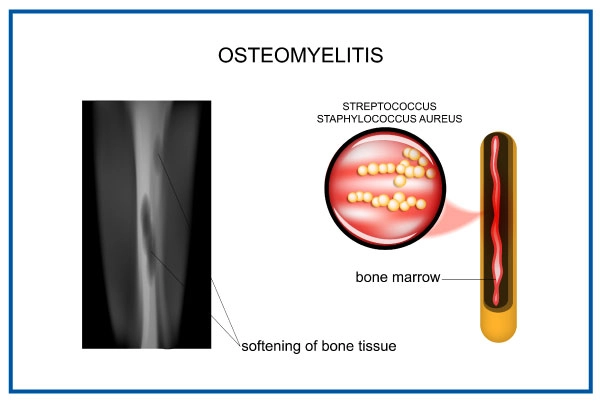
Types of osteomyelitis
Acute Osteomyelitis
- Haematogenous osteomyelitis: Acute hematogenous osteomyelitis is a common bone infection. It usually affects boys and is generally seen in children. Acute osteomyelitis occurs in areas of high metabolic activity and often infects the distal femoral and proximal tibial metaphysis.
- Direct inoculation osteomyelitis: It is an infection of the bone caused due to inoculation of organisms from trauma, infection or from sepsis initiated by a surgical procedure.
Chronic Osteomyelitis
This type of infection fails to respond to treatment and reappears to stay for a long time. Often, chronic osteomyelitis is polymicrobial, indicating the involvement of more than one infectious agent. It causes bone pain and Brodie's abscess (chronic pyogenic osteomyelitis).
Vertebral Osteomyelitis
Vertebral osteomyelitis is a serious infection of the spine, usually caused by bacteria like Staphylococcus aureus or, less commonly, fungi. It often occurs when an infection spreads through the bloodstream from another site, after spinal surgery, or following a traumatic injury.
Get a second opinion from trusted experts and makeconfident, informed decisions.
Osteomyelitis Symptoms
The osteomyelitis symptoms include:
- Localised bone pain
- Excessive sweating
- Decreased movement of the affected body part
- The overlying skin patch may be inflamed and red
- Accumulation of pus
- Muscle cramps
- Sudden weight loss
- General malaise
- Fever
- Fatigue
- Chills
When to See a Doctor?
Consult your doctor if there is worsening bone pain accompanied by fever. If you notice signs and symptoms of an infection because of a medical condition or a recent operative procedure or injury, book an appointment with a doctor.
- Recent Surgery or Trauma: Consult a doctor if you experience unusual symptoms like pain or swelling after a surgical procedure or spinal trauma.
- General Symptoms: If you feel fatigue, chills, or unexplained weight loss along with bone discomfort.
- Existing Medical Conditions: If you have diabetes, weakened immunity, or are prone to infections, consult a doctor at the first sign of symptoms.
Consult our orthopaedic doctors or general physicians for more information and adequate treatment for osteomyelitis.
Osteomyelitis Causes
- Bacterial Infections: Most commonly caused by Staphylococcus aureus, which can enter the bloodstream or directly infect the bone.
- Fungal Infections: Less common but may occur in immunocompromised individuals.
- Infection Spread Through Bloodstream: Infections from other parts of the body, such as the skin, urinary tract, or lungs, can travel to the bone via blood.
- Direct Contamination: Open fractures, wounds, or surgical procedures (like joint replacements) can introduce bacteria directly to the bone.
- Injuries or Trauma: Deep puncture wounds or severe injuries can expose the bone to infection.
- Weakened Immune System: Conditions like diabetes, HIV, or chemotherapy weaken immunity, increasing the risk of infection.
- Vascular Insufficiency: Poor blood flow, as seen in diabetes, can make bones more vulnerable to infection.
- Intravenous Drug Use: Using non-sterile needles can introduce bacteria into the bloodstream, potentially causing bone infections.
Conditions That Increase the Risk of Osteomyelitis
The conditions and lifestyle factors that increase the risk of osteomyelitisthat may escalate a person’s susceptibility to osteomyelitis are:
- Cancer
- Uncontrolled diabetes
- Long-term skin infections
- Poor blood circulation (arteriosclerosis)
- Immune deficiency disorders
- The implantation of prosthetic joints
- Intravenous drug use
- Sickle cell anaemia
- Excessive alcoholism
- Smoking
- HIV or AIDS
- Rheumatoid arthritis
Osteomyelitis Complications
To prevent complications, starting an early treatment, including antibiotic therapy, is necessary. Few complications can arise with untreated or inadequately treated osteomyelitis; they are as follows:
- Brodie's abscess
- Osteonecrosis (bone death)
- Soft tissue inflammation (cellulitis)
- Septicaemia (Sepsis)
- Chronic infection with no response to treatment
- Pathological fractures
- Bone deformity
- Systemic infection
- Squamous cell carcinoma (Skin cancer)
- Sinus tract formation
- Amyloidosis (rare)
Osteomyelitis Diagnosis
The orthopaedic doctor will enquire about the patient's medical history and perform a physical examination to diagnose osteomyelitis symptoms.
The doctor may examine the area around the affected bone for any inflammation or tenderness and may recommend a combination of diagnostic tests to determine the condition:
- Complete Blood Count (CBC): Identifies infection, anaemia, and leukaemia by evaluating white blood cells (WBCs).
- Erythrocyte Sedimentation Rate (ESR): Measures inflammation by checking the rate at which red blood cells settle.
- C-Reactive Protein (CRP): Detects bacterial infections and inflammation, helping diagnose osteomyelitis.
- Blood Culture Test: Identifies bacteria or fungi in the blood.
- Needle Aspiration/Bone Biopsy: Extracts bone samples to identify pathogens and abnormal cells.
- X-ray: Examines bone damage, revealing signs of infection.
- Bone Scan (Scintigraphy): Detects chemical and physical changes in bones, helpful for osteomyelitis.
- CT Scan: Provides detailed images of bones and organs to diagnose infections like osteomyelitis.
- MRI Scan: It uses magnetic fields to create images of bones, which is helpful in diagnosing osteomyelitis.
- Ultrasound (USG): It uses sound waves to produce images and is useful for detecting acute osteomyelitis.
Osteomyelitis Treatment
Osteomyelitis treatment options vary from person to person and the severity of the condition. The treatment of osteomyelitis aims to cure bone infection and reduce any long-term complications. Treatment may include:
- Medicines: A hospital stay may be required, and the patient will be given intravenous (IV) antibiotics. After that, oral antibiotic medications may be prescribed for several weeks. Chronic osteomyelitis may require long-term medications.
- Surgery: Osteomyelitis surgery is done when antibiotics cannot cure the bone infection. The surgery may be needed to drain the infected fluid, remove necrosed bone tissue, restore blood flow to the bone, take out any foreign objects or amputate the limb.
- Pain management: Nonsteroidal anti-inflammatory drugs (NSAIDs) are prescribed to treat pain and inflammation.
- Bed rest: The patient may need to take bed rest to limit movements of the affected area and to avoid pain.
Your health is everything - prioritize your well-being today.
Dos and Don’ts
Follow the below-mentioned Do’s and Don’ts to prevent osteomyelitis and its complications. It is a bone infection, and the source of the blood infection is usually Staphylococcus aureus. It is mainly found in smokers, diabetes or kidney failure patients.
Osteomyelitis symptoms include fever, fatigue, inflammation and redness in the affected bone area. Its treatment involves osteomyelitis medications, pain relievers, bed rest and surgery.
Osteomyelitis Care at Medicover Hospitals
At Medicover hospitals, we have the most experienced and trusted medical team consisting of general physicians and orthopaedic doctors who provide the best management for osteomyelitis. We are dedicated to providing excellent healthcare services to our patients holistically. Our team adopts a multidimensional approach to managing bone infection and related complications with utmost care and the active participation of medical experts from different specialities. We ensure world-class healthcare facilities in all our departments at affordable prices to ensure high-quality treatment outcomes.
Frequently Asked Questions
How can osteomyelitis be prevented?
Osteomyelitis can be prevented by maintaining good hygiene, treating infections promptly, avoiding injuries, managing chronic conditions like diabetes, and taking care of surgical wounds to reduce the risk of bacterial entry.
Can osteomyelitis cause death?
If left untreated, osteomyelitis can lead to severe complications such as sepsis, organ failure, or amputation, which in rare cases, may result in death. Early diagnosis and treatment are crucial to prevent such outcomes.
What is a normal CRP level for osteomyelitis?
The normal C-reactive protein (CRP) level for osteomyelitis typically ranges from 0 to 10 mg/L. Elevated CRP levels above 10 mg/L may indicate infection or inflammation, commonly seen in osteomyelitis patients.
What is the recovery rate for osteomyelitis?
The recovery rate for osteomyelitis varies depending on factors like severity, treatment, and overall health. With early intervention, most patients recover fully, while severe cases may require longer treatment or surgical procedures.
Can osteomyelitis be cured without surgery?
In some cases, osteomyelitis can be treated with antibiotics alone, especially if caught early. However, severe or chronic cases may require surgery to remove infected tissue or drainage, making surgery often necessary for full recovery.
Is osteomyelitis painful?
Yes, osteomyelitis is usually painful. Symptoms include localized pain, swelling, and warmth over the infected bone. Pain may worsen over time if the infection spreads, requiring medical intervention for relief.