What is Tympanoplasty Surgery?
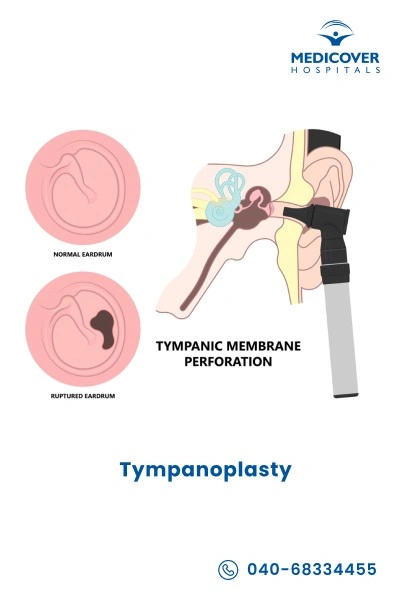
Tympanoplasty is a surgery to repair a hole or tear in the eardrum, which often happens after repeated infections or injury. A damaged eardrum can cause hearing loss, buzzing, or frequent ear discharge.
During the procedure, an ENT surgeon gently patches the hole using the patient's own tissue, allowing the eardrum to heal and sound to travel normally again. In some cases, tiny middle ear bones are also repaired to improve hearing further.
It's a safe and effective surgery that not only restores hearing but also prevents future infections, helping patients enjoy a healthier, more confident life.
Types of Tympanoplasty
Tympanoplasty can be classified into different types based on how much of the middle ear needs repair.
Type I Tympanoplasty (Myringoplasty):
This is the simplest form of tympanoplasty. It is performed when only the eardrum is damaged, and the middle ear bones are still healthy. The surgeon places a graft over the hole in the eardrum, allowing it to heal and restore the normal passage of sound waves. This type is commonly done for patients with a small to moderate perforation and good hearing bone function.
Type II Tympanoplasty:
In this type, both the eardrum and the first hearing bone, called the malleus, are affected. The surgeon repairs the eardrum and positions the graft onto the incus (the next bone in the chain). This helps re-establish the connection needed for sound to move from the eardrum to the inner ear, improving hearing.
Type III Tympanoplasty:
When both the malleus and the incus are damaged or absent, the surgeon directly places the graft onto the stapes bone (the third bone). By doing so, the eardrum can vibrate against the stapes and continue transmitting sound into the inner ear. This type is usually done in more advanced or long-standing ear problems.
Type IV Tympanoplasty:
This type is used when most of the middle ear bones are missing or severely damaged. The surgeon reduces the middle ear cavity and positions the graft in a way that covers the stapes footplate while keeping it open to receive sound vibrations. This protects the inner ear while still allowing hearing to be maintained.
Type V Tympanoplasty:
This method is rarely performed today. It is done when the stapes footplate, which normally moves to transmit sound, becomes fixed or immobile. The surgeon creates a small surgical opening, called a fenestration, to bypass the fixed stapes and allow sound transmission. Though less common now, this technique was important in the past for treating complex ear conditions.
1-2 Hours
Surgery Duration
General or Local Anesthesia with Sedation
Anesthesia Used
When is Tympanoplasty Recommended?
Tympanoplasty can be life-changing for people struggling with ear problems that affect hearing, comfort, or daily life. Based on ENT clinical guidance, here are the main indications of Tympanoplasty include:
- Persistent Eardrum Perforation: If a hole in the eardrum does not heal naturally after infections or injury, it can cause continuous hearing problems and increase the risk of recurrent ear discharge. Tympanoplasty closes the perforation and restores ear health.
- Chronic Ear Infections (Chronic Otitis Media): Repeated ear infections can damage the eardrum and middle ear structures. Tympanoplasty helps stop frequent infections, reduces discharge, and protects the inner ear from further damage.
- Hearing Loss Due to Eardrum or Bone Damage: When hearing ability is reduced because of a damaged eardrum or affected middle ear bones, tympanoplasty repairs these structures and improves hearing clarity, making everyday communication easier.
- Ear Trauma or Injury: Sudden injuries, loud blasts, accidents, or inserting objects into the ear can cause eardrum tears. Surgery is recommended to repair the damage and prevent long-term complications.
- Children with Ongoing Ear Problems: In children, repeated infections and a long-standing perforated eardrum can affect hearing and speech development. Tympanoplasty restores normal hearing and prevents delays in growth and learning.
Preparation for Tympanoplasty Surgery Procedure
Preparing well for your tympanoplasty helps ensure a safe procedure and a smooth recovery. Here's what you can expect:
Before Surgery:
- Complete medical history review and pre-op visit with your ENT specialist.
- Hearing tests and possibly a CT scan to check the middle ear.
- Routine blood work and ECG to ensure you're fit for surgery.
Lifestyle Adjustments:
- Stop smoking 2-3 weeks before surgery.
- Avoid alcohol and blood-thinning medicines (aspirin, NSAIDs, vitamin E, herbal supplements) as advised.
- Eat a nutritious diet rich in protein, vitamins, and minerals.
Home & Support:
- Arrange someone to drive you to and from the hospital.
- Prepare a recovery space with soft pillows, medications, water, and easy access to entertainment.
- Keep your home calm, clean, and noise-free for ear comfort.
Day Before & Day of Surgery:
- Follow fasting instructions (usually no food/drink after midnight).
- Shower and avoid lotions, perfumes, or hair products.
- Wear loose, front-opening clothes and remove all jewellery.
- Carry all medical reports and documents.
What Happens During Tympanoplasty Surgery?
Tympanoplasty is a delicate ear surgery designed to repair a damaged eardrum and, in some cases, the tiny bones of the middle ear. The procedure is carefully performed in several steps to ensure proper healing and restore hearing.
- Anesthesia: On the day of surgery, you'll meet your ENT surgical team one last time to review everything. Once in the operating room, general anesthesia is administered, so you'll be asleep and completely comfortable throughout the procedure.
- Accessing the Eardrum: The surgeon makes a small incision, usually behind the ear or inside the ear canal, to gently reach the damaged eardrum. This approach allows precise access without affecting other parts of the ear.
- Graft Harvesting: A small piece of tissue, often from behind your ear or from fascia, is prepared to patch the hole in the eardrum. This tissue will serve as the graft to help your eardrum heal naturally.
- Repairing the Eardrum: Using a microscope or endoscope, the surgeon carefully places the graft over the perforation. If any of the tiny middle ear bones are damaged, they may also be repaired or repositioned to restore proper sound transmission.
- Closing and Dressing: Once the repair is complete, the incision is closed, and a light ear packing or dressing is applied to support healing. This packing usually stays in place for a few days to protect the graft.
- Post-Surgery Monitoring: You'll be observed in the recovery area until the anesthesia wears off. Most patients can go home the next day, with instructions on keeping the ear dry, avoiding pressure or loud noises, and managing mild discomfort.
Who Will Perform Tympanoplasty Surgery?
Tympanoplasty is a specialized ear surgery performed by experienced ENT (Ear, Nose, and Throat) surgeons to repair the eardrum and restore hearing.
ENT (Otolaryngology) Surgeons
- These are doctors trained in treating ear, nose, and throat conditions.
- They have the expertise to repair perforated eardrums, middle ear bones, and other ear structures.
Otologic or Neurotologic Surgeons
- ENT surgeons who specialize further in ear and temporal bone surgeries.
- Often handle complex or high-risk cases involving chronic ear disease or hearing loss.
Hospital Surgical Team
- Tympanoplasty is performed in a hospital or surgical center with full anesthesia support.
- Anesthesia specialists, nurses, and audiologists assist the ENT surgeon for a safe and effective procedure.
Hearing Assessment Support
- Audiologists may conduct pre- and post-surgery hearing tests to guide the surgeon and track recovery.
Recovery After Tympanoplasty Surgery Procedure
Recovering from tympanoplasty is a gradual process, and following your surgeon's instructions carefully can make a big difference in healing and hearing improvement.
Immediately After Surgery
- Patients are usually monitored in the hospital for a few hours to a day.
- Mild discomfort, dizziness, or ear fullness is common and typically managed with medications.
- A small ear packing or dressing may be placed to protect the eardrum repair.
First Week at Home
- Keep the ear dry; avoid swimming, bathing with water entering the ear, or using cotton swabs.
- Take prescribed antibiotics and pain medications as directed.
- Limit strenuous activities, heavy lifting, and bending to prevent pressure changes in the ear.
Follow-Up Visits
- The surgeon will remove ear packing (if any) and inspect the eardrum repair.
- Regular audiology tests may be scheduled to monitor hearing improvement.
Activity and Lifestyle Restrictions
- Avoid blowing your nose forcefully for at least 2-4 weeks.
- Avoid exposure to dusty or smoky environments that may irritate the ear.
- Resume normal daily activities gradually as advised by the surgeon.
Full Recovery Timeline
- Most patients notice improvement in hearing within a few weeks to months.
- Complete healing of the eardrum and middle ear structures may take 6-8 weeks.
Signs to Watch For
- Persistent pain, swelling, or discharge from the ear
- Fever or worsening dizziness
- Sudden hearing loss or ringing in the ear
Benefits of Tympanoplasty Surgery
Tympanoplasty surgery not only repairs the eardrum but also provides several long-term advantages that improve ear health, hearing, and overall quality of life.
- Restores hearing and ear function: Tympanoplasty repairs the eardrum and, if needed, middle ear bones, helping sound travel normally. Most patients notice clearer hearing and reduced buzzing or muffled sounds.
- Reduces ear infections and discharge: By closing the perforation, the surgery prevents water or bacteria from entering the middle ear, lowering the risk of recurrent infections and discomfort.
- Protects the inner ear: A repaired eardrum shields the delicate middle and inner ear structures, preventing long-term damage and complications.
- Improves quality of life: With better hearing and fewer infections, patients can enjoy everyday activities - conversations, work, and music - with confidence and comfort.
- Long-lasting results: Once the eardrum heals and the graft integrates, improvements in hearing and ear health are typically permanent, provided ear care is maintained.
Risks of Tympanoplasty Surgery
Like any surgical procedure, tympanoplasty carries certain risks. Most complications are rare and manageable, but it is important for patients to be aware of them before surgery.
- Mild pain or discomfort: Some tenderness or fullness in the ear is normal after surgery and usually resolves in a few days.
- Infection or bleeding: Although rare, there's a small risk of infection or bleeding at the surgical site. Following care instructions minimizes this risk.
- Graft failure: Occasionally, the graft may not take properly, leading to incomplete healing and the need for a repeat procedure.
- Hearing may not fully return: While most patients experience significant improvement, hearing restoration depends on the condition of the middle ear bones and extent of prior damage.
- Other rare complications: These include dizziness, ringing in the ear (tinnitus), or changes in taste due to temporary nerve irritation.
Cost of Tympanoplasty Surgery in India
The cost of Tympanoplasty Surgery typically varies depending on the complexity of the perforation, the technique used (with or without ossicular repair), the surgeon’s expertise, and the hospital facilities. On average, tympanoplasty in India can range from Rs. 45,000 to Rs. 1,50,000.

















































