What Is a Bariatric (Weight Loss) Surgery?
Bariatric surgery is also known as weight-loss or metabolic surgery, refers to a group of operations designed to help people with obesity lose weight and improve overall health by altering the digestive system. These surgeries work by making the stomach smaller, limiting the amount of food you can eat, changing how your body absorbs nutrients, and influencing hunger-related hormones to help you feel full sooner.
Why Is It Done?
Doctors typically recommend bariatric surgery when someone:
- If you have a BMI (Body Mass Index) of 40 or higher (severe obesity), or
- If you have a BMI of 35-39.9 and suffer from serious weight-related health issues such as type 2 diabetes, high blood pressure, or sleep apnea.
Shifting your BMI from severe obesity to a healthier range doesn't just reduce weight. It can dramatically lower the risks of heart disease, stroke, fatty liver disease, certain cancers, and other metabolic conditions.
Types of Bariatric Surgery Procedures
Bariatric surgery isn't for quick results. It's a powerful tool for long-term change. Many patients lose up to one-third of their body weight in two years, significantly improve or even reverse type 2 diabetes, sleep apnea, hypertension, and more.
Gastric Bypass (Roux-en-Y Gastric Bypass)
A small pouch is created at the top of the stomach and directly connected to the small intestine, bypassing part of the stomach and upper intestine. This reduces the amount of food you can eat and lowers calorie absorption.
Sleeve Gastrectomy
A large portion of the stomach is removed, leaving a smaller, banana-shaped sleeve. In this procedure, about 75-80% of the stomach is removed, leaving a smaller, banana-shaped pouch. This smaller stomach limits how much you can eat and helps reduce hunger naturally.
Adjustable Gastric Band (Lap-Band)
A silicone band placed around the upper part of the stomach creates a small pouch. This band is adjustable and helps control food intake. The size of the opening between the pouch and the rest of the stomach can be adjusted, allowing for better control of food intake.
Biliopancreatic Diversion with Duodenal Switch (BPD/DS)
This complex surgery removes part of the stomach and reroutes a significant portion of the small intestine. It combines restrictive and malabsorptive techniques to promote weight loss.
Bariatric Revision Surgery
For individuals who have had prior bariatric procedures, revision surgery may be needed to address complications, insufficient weight loss, or other issues.
Mini Gastric Bypass (One Anastomosis Gastric Bypass)
This variation of gastric bypass connects a small stomach pouch to the intestine in one step, making it a quicker procedure with fewer connections than RYGB.
Single-Anastomosis Duodeno-Ileal Bypass with Sleeve Gastrectomy (SADI-S)
This is a newer procedure combining a sleeve gastrectomy with a single connection to the small intestine.
2-4 hours
Surgery Duration
General anesthesia
Anesthesia Used
6 to 8 weeks
Full Recovery Timeline
When is Bariatric Surgery Recommended?
Bariatric surgery does not only for weight loss. It can significantly improve or even resolve serious health problems related to obesity:
Conditions That Bariatric Surgery Can Treat
- Severe Obesity: Bariatric surgery is typically recommended for those with a BMI of 40 or higher. It can also be considered for individuals with a BMI of 35 or higher if they have obesity-related severe health issues.
- Type 2 Diabetes & High Blood Sugar: Many patients experience dramatic improvements in blood sugar control after surgery. In fact, remission occurs in over 90% of those who undergo surgery early, especially within one year of diabetes diagnosis.
- High Blood Pressure & Heart Disease: Surgery lowers blood pressure and reduces risks like heart attack, stroke, and heart failure. One study showed nearly a 39% drop in cardiovascular events after surgery.
- High Cholesterol & Metabolic Syndrome: Losing weight after surgery helps reduce harmful cholesterol levels and improves conditions tied to metabolic imbalance, such as elevated triglycerides.
- Obstructive Sleep Apnea: Surgery can relieve the pressure of excess throat fat, often significantly improving or curing sleep apnea.
- Fatty Liver Disease (NAFLD / NASH): Up to 90% of patients see improvements in liver fat, with many achieving full remission after surgery.
- Joint Pain and Osteoarthritis: Excess weight puts enormous strain on joints. Post-surgery, many patients experience reduced joint pain and improved mobility.
- Gastroesophageal Reflux Disease (GERD): Weight-related pressure on the stomach often leads to acid reflux. Weight loss via surgery frequently leads to lasting relief.
- Infertility & PCOS: Obesity-related hormonal imbalances can affect fertility and worsen conditions like PCOS. Surgery can help restore hormone balance and improve fertility outcomes.
- Cancer Risk Reduction: Long-term studies show bariatric surgery is associated with a 50% lower risk of developing certain cancers, including breast, colon, liver, and endometrial cancers.
How to Prepare for Bariatric Surgery?
- Consultation and Evaluation: Meet with a bariatric surgeon to discuss surgery options. Undergo physical exams, imaging, and blood tests to assess health.
- Education and Counselling: Attend informational sessions about surgery and recovery. Meet with a dietitian and mental health professional for guidance.
- Pre-Operative Requirements: Follow dietary guidelines and complete necessary tests like blood work, EKG, and pulmonary tests.
- Lifestyle Changes: Adopt a healthy diet, exercise regularly, and quit smoking to reduce Bariatric surgery risks.
- Medical Management: Manage chronic conditions like diabetes and hypertension with your healthcare provider.
- Support System: Build a support system of family and friends to assist during recovery.
- Pre-Operative Diet: Follow a specific low-calorie or liquid diet as instructed by your healthcare team.
- Psychological Preparation: Address emotional factors through counselling or support groups.
- Medications: Consult your doctor about medication adjustments before surgery.
- Logistics: Plan your hospital stay, arrange transportation, and prepare for home recovery.
- Post-Operative Preparation: Stock up on protein supplements, vitamins, and medications. Clear your schedule for recovery time.
- Final Consultation: Have a final meeting with your surgeon to address any last-minute questions before surgery.
Steps Involved in Bariatric Surgery
During a bariatric surgery, several steps are taken to achieve the desired weight loss and metabolic changes. The exact details may vary depending on the type of surgery being performed, but a general overview of what happens during bariatric surgery is as follows:
Initial Consultation & Assessment
You'll meet with a bariatric surgeon to review your medical history, weight loss journey, and health goals. The doctor will also run tests like blood work, heart and lung checks, and imaging to ensure you're a suitable candidate.
Anesthesia
You will receive general anesthesia to ensure you're comfortable and pain-free throughout the procedure.
Incisions
Small incisions are made in the abdomen to give the surgeon access to the surgical area. In many cases, minimally invasive techniques (laparoscopic surgery) are used, involving tiny instruments and a camera.
Access to the Stomach
The surgeon uses the incisions to reach the stomach and digestive tract.
Surgical Technique
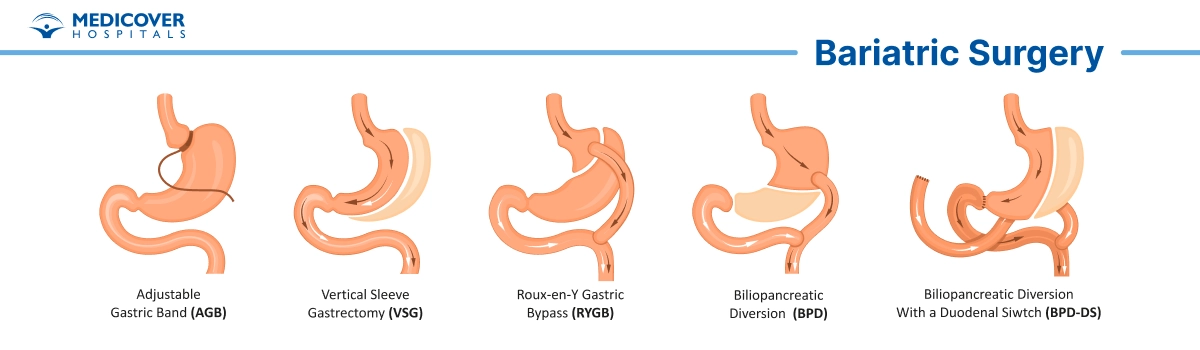
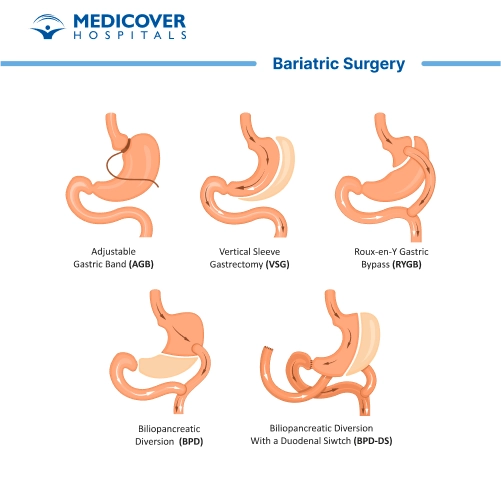
Different types of bariatric surgery use different techniques:
- Gastric Bypass (Roux-en-Y): A small pouch is created at the top of the stomach and connected to a lower part of the small intestine, bypassing a section of both the stomach and small intestine.
- Sleeve Gastrectomy: A large portion of the stomach is removed, leaving a smaller, banana-shaped "sleeve."
- Gastric Banding (Lap-Band): A band is placed around the top of the stomach to create a small pouch.
- Biliopancreatic Diversion with Duodenal Switch (BPD/DS): A portion of the stomach is removed, and a larger part of the small intestine is bypassed.
Closure and Healing
The incisions are carefully closed with sutures or staples, and the healing process begins.
Recovery and Monitoring
After the surgery, you'll be moved to a recovery area where medical staff will monitor your vital signs and ensure you wake up safely from the anesthesia.
Hospital Stay
Depending on the type of surgery and your health, you may stay in the hospital for a few days to recover and receive post-operative care.
Diet Progression
You will start with clear liquids, gradually move to soft foods, and eventually return to regular foods based on the guidance from your healthcare team.
Follow-up Care
Regular follow-up appointments will be scheduled to monitor your progress, adjust medications, and provide advice on diet and lifestyle changes.
Who Performs the Bariatric Surgery Procedure?
Bariatric or metabolic surgery is performed by General surgeons who specialise in treating obesity and related conditions. These surgeons have advanced training to ensure the procedure is both safe and effective.
Bariatric surgeons typically have a background in general surgery, along with additional expertise in handling complex obesity cases. They work closely with a multidisciplinary team, including dietitians, psychologists, nurses, and other specialists, to provide comprehensive care before, during, and after surgery.
Recovery After Bariatric Surgery
The recovery process after bariatric surgery is a crucial phase that involves adjusting to your new digestive system, adopting a modified diet, and gradually resuming physical activity. Recovery times can change depending on the type of surgery, individual health, and adherence to post-operative guidelines.
Here's an overview of what to expect during the recovery period
Immediate Post-Op (Hospital Stay):
- Stay in the hospital for monitoring and recovery.
- Start moving around soon to prevent blood clots.
- Pain management medications will be provided.
Week 1-2:
- Transition from clear liquids to pureed/soft foods as per your surgeon's guidelines.
- Sip fluids slowly, avoid carbonated drinks.
- Attend follow-up appointments and take prescribed medications.
Week 3-4:
- Introduce soft, protein-rich solid foods.
- Focus on small, frequent meals and chew thoroughly.
- Start with light physical activity, such as short walks.
Months 2-3:
- Progress to a variety of foods and increase physical activity intensity.
- Monitor weight loss and health improvements, and discuss with your healthcare team.
Long-Term Recovery:
- Keep regular follow-up appointments.
- Maintain a balanced diet with portion control and hydration.
- Stay active and address emotional challenges with counseling or support groups.
Lifestyle Changes After Bariatric Surgery
Undergoing bariatric surgery necessitates significant lifestyle changes to ensure successful weight loss, improved health, and long-term well-being. These changes are designed to support your body's new digestive system and promote healthy eating habits.
Eating Habits
- Portion Control: Eat small, controlled portions.
- Slow Eating: Chew thoroughly and eat slowly.
- Nutrient-rich Foods: Focus on protein, vegetables, fruits, and whole grains.
- Hydration: Drink fluids between meals, not during.
Nutritional Guidelines
- Balanced Diet: Include essential nutrients and vitamins.
- Supplements: Take prescribed vitamins to avoid deficiencies.
- Avoid Empty Calories: Limit sugary and processed foods.
Meal Planning
- Regular Meals: Stick to three meals and plan snacks.
- High-Quality Protein: Eat lean proteins for muscle and metabolism.
Physical Activity
- Regular Exercise: Engage in walking, swimming, or strength training.
- Gradual Progression: Increase exercise intensity slowly.
Follow-Up Care
- Medical Appointments: Attend regular check-ups.
- Blood Work: Have routine tests to monitor health.
Social Support
- Family & Friends: Share your journey with loved ones.
- Support Groups: Connect with others in bariatric surgery groups.
Benefits of Bariatric Surgery
Weight Loss Benefits of Bariatric Surgery
Effective Weight Loss: Bariatric surgery helps with lasting weight loss by reducing stomach size or changing the digestive process. This limits how much food you can eat or absorb, leading to gradual weight loss.
Improvement of Health Conditions
Health Boost: It can significantly improve or resolve obesity-related issues like hypertension, type 2 diabetes, and sleep apnea, lowering your risk of health complications.
Better Quality of Life
Quality of Life: Successful weight loss can improve mobility, reduce joint pain, boost self-esteem, and enhance overall well-being.
Long-Term Weight Management
Long-Term Success: Bariatric surgery helps maintain weight loss better than non-surgical methods. However, you still need to commit to a healthy lifestyle with dietary changes and regular exercise.
Lower Mortality Risk
Studies show that bariatric surgery significantly reduces mortality risk in severely obese individuals when related health conditions are improved.
Bariatric Surgery Side Effects
Undergoing bariatric surgery can be life-changing, but like any major surgery, it carries both short-term and long-term risks. Here's what doctors want you to know:
Surgery-Related Risks
- Bleeding and Infection: As with any operation, there's a chance of bleeding or infection at the surgical site.
- Reactions to Anesthesia & Breathing Issues: Some patients may experience adverse reactions to anesthesia or breathing complications after surgery.
- Blood Clots: Particularly in the legs or lungs (pulmonary embolism); preventive measures like leg compression and early movement are important.
- Leaks & Bowel Obstruction: Rare, serious complications like leaks in the gastrointestinal system or intestinal blockages may require immediate medical attention.
Long-Term Risks
- Dumping Syndrome: Rapid stomach emptying can cause nausea, dizziness, diarrhea, or faintness, especially after meals high in sugar.
- Nutrient Deficiencies & Malnutrition: Many patients may develop deficiencies in vitamins (A, D, E, K, B12), iron, or protein, requiring lifelong supplements and monitoring.
- Gallstones & Kidney Stones: Rapid weight loss increases the risk of forming stones in the gallbladder or kidneys.
- Gastroesophageal Reflux (GERD): Especially common after sleeve gastrectomy, causing heartburn and reflux symptoms.
- Strictures & Leaks: Narrowing of the surgical site ("stricture") or leaks may require further intervention
- Psychological Impact: Feelings of low energy, depression, or anxiety can arise due to changes in eating patterns and emotional relationships with food.
- Need for Additional Surgeries: Between 1% and 8% of patients may require additional surgery within a few years due to complications or revisions.
Understanding Bariatric Surgery Costs
Bariatric surgery, also known as weight-loss surgery, is a treatment option for individuals who haven't achieved long-term success with diet and exercise alone. In India, the bariatric surgery cost typically ranges from Rs 2 lakh to Rs 5 lakh, depending on the type of procedure and other factors.
Cost Influencing Factors
- Type of Procedure
- Hospital Location & Infrastructure
- Surgeon's Expertise
- Pre- and Post-Operative Care
- Procedure Complexity & Patient Health
- Hospital Stay Duration






















































