Diabetes: Symptoms, Causes, and Treatments
Written by Medicover Team and Medically Reviewed by Dr M N Lakshmikanth Reddy , General Medicine
Diabetes is a long-term health disease that impacts the body and converts food into energy, resulting in high blood sugar levels. It primarily affects the endocrine system but can also impact the heart, kidneys, nerves, and eyes.
With the right medical care and healthy daily habits, people living with diabetes can control the condition well, reduce complications, and lead a better life. Early detection is critically crucial for controlling symptoms and preventing long-term damage.
What are the Diabetes Symptoms and Warning Signs?
Identifying diabetes symptoms early is crucial for timely treatment and improved health outcomes. Symptoms of diabetes vary by type and can be mild or severe. Many, especially with type 2, may have no clear signs. Regular checkups and awareness help prevent complications and promote better health.
Common Diabetes Symptoms
- Blurred vision
- Increased thirst
- Numbness in hands or feet
- Fatigue
- Unplanned weight loss
- Dry mouth
- Frequent urination
- Recurrent infections
- Slow-healing wounds
Severe Symptoms
- Nausea or vomiting (especially in type 1 diabetes)
- Abdominal pain
- Mental confusion or unconsciousness
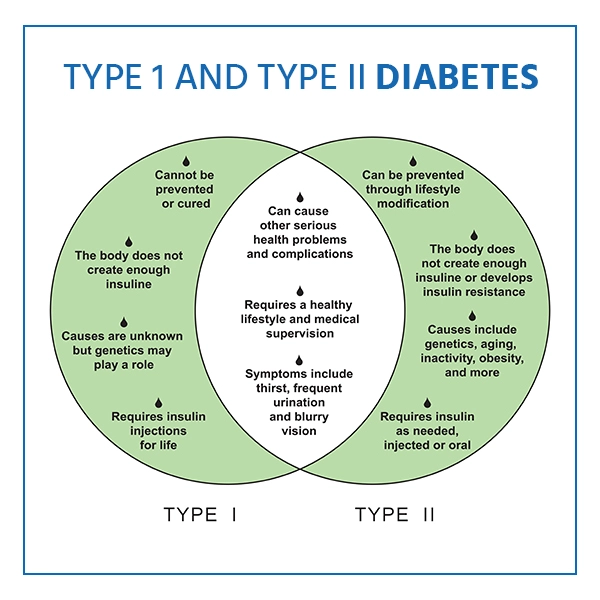
What Are the Different Types of Diabetes?
Understanding the various forms of diabetes helps provide accurate diagnoses and effective care. Each type has its own unique causes, symptoms, and management approaches, so understanding the differences can help ensure that proper care is provided. Different factors cause each type and affect insulin function in unique ways. This helps determine the best approach for ongoing diabetes care.
Type 1 Diabetes
Type 1 diabetes happens when the body's immune system mistakenly attacks the cells that make insulin. It often starts in childhood or during the teenage years and needs lifelong insulin treatment to keep blood sugar under control.
Type 2 Diabetes
The most common type is often linked to lifestyle and genetic factors. The body becomes insulin-resistant or doesn't produce enough insulin. It can usually be managed with diet, exercise, and oral medications.
Gestational Diabetes
Gestational diabetes develops during pregnancy in women who've never had diabetes before. It usually disappears after delivery, but raises the risk of future type 2 diabetes for both mother and child.
Prediabetes
A condition where blood sugar levels are elevated but not high enough to be diagnosed as type 2 diabetes. It can be reversed through healthy lifestyle changes.
What are the Common Causes and Risk Factors of Diabetes?
Diabetes can result from a variety of causes depending on its type. Identifying the underlying causes and associated risk factors allows for early intervention and preventive action.
Causes
- Type 1 Diabetes: Autoimmune destruction of insulin-producing cells
- Type 2 Diabetes: Insulin resistance and pancreatic insufficiency
- Gestational Diabetes: Hormonal changes during pregnancy increase insulin resistance
Risk Factors
- Family history of diabetes
- Overweight or obesity
- Age over 45
- Low physical activity
- Previous gestational diabetes
- Polycystic ovary syndrome (PCOS)
- Non-alcoholic fatty liver disease
Get a second opinion from trusted experts and makeconfident, informed decisions.
How is Diabetes Diagnosed?
Diagnosis of diabetes relies on specific blood tests that measure glucose levels. Early and accurate testing helps initiate treatment before complications occur. At Medicover, we utilize advanced diagnostic tools to ensure that patients receive the proper care from the outset.
Common Diagnostic Tests
- Fasting Plasma Glucose (FPG)
- Oral Glucose Tolerance Test (OGTT)
- Hemoglobin A1c Test
- Random Glucose Test
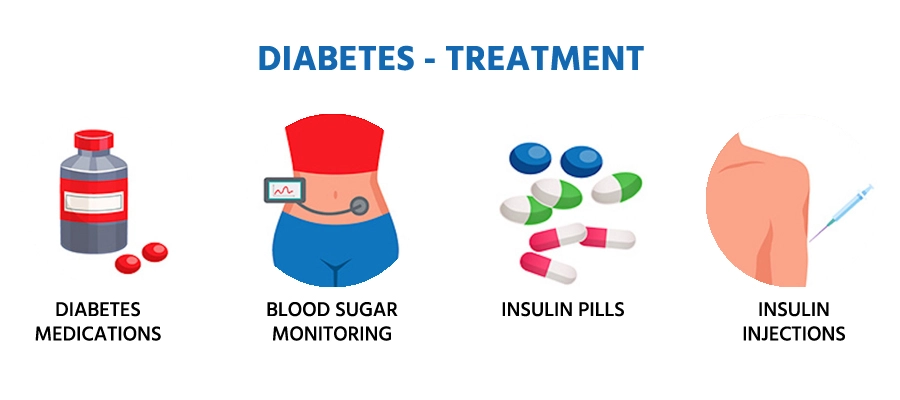
What Are the Treatment Options for Diabetes?
Managing diabetes involves taking medication, adopting healthy habits, and potentially using insulin therapy, depending on the type and severity of the condition. The primary goal is to manage blood sugar levels and prevent complications.
Available Treatments
- Type 1 Diabetes: Insulin therapy, blood sugar monitoring, and diet control
- Type 2 Diabetes: Oral medications, lifestyle changes, and possibly insulin
- Gestational Diabetes: Diet management, physical activity, and insulin, if required
When to See a Doctor?
Knowing when to consult a doctor helps avoid complications and manage symptoms efficiently. Symptoms that persist or worsen may indicate uncontrolled blood sugar levels.
Seek medical attention if
- Symptoms last for more than a few days
- You experience frequent infections or delayed healing.
- You belong to a high-risk group (family history, overweight, over age 45)
Your health is everything - prioritize your well-being today.
What Is the Recovery Process After Diabetes Treatment?
Recovery focuses on managing long-term conditions rather than finding a cure for them. With appropriate support, most individuals can live whole, healthy lives. The recovery journey includes routine checkups, education, and mental health support.
Post-Treatment Recovery Includes
- Regular follow-ups
- Monitoring of blood sugar levels
- Dietary adjustments and physical activity
- Emotional and mental health care
What Precautions Can Help Prevent Diabetes?
Preventing diabetes, especially type 2 and gestational diabetes, largely depends on maintaining a healthy lifestyle. Simple habits, such as eating a balanced diet, maintaining an active lifestyle, and controlling weight, can have a significant impact. Regular health check-ups and understanding risk factors play an important role in early prevention.
Prevention Tips
- Maintain a healthy weight.
- Follow a low-sugar, high-fiber diet.
- Stay physically active
- Monitor blood sugar if at risk.
- Avoid tobacco and excessive alcohol.
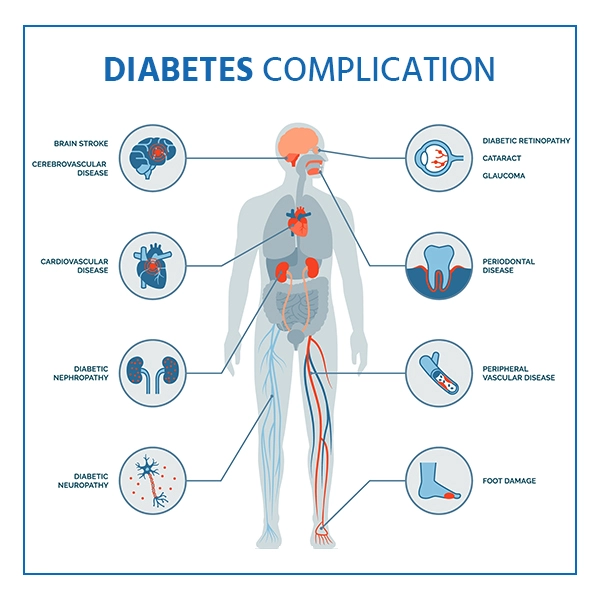
Possible Complications if Unmanaged
- Cardiovascular disease
- Kidney and nerve damage
- Vision loss and foot ulcers
Early action can help avoid these complications and support long-term wellness.
Our Experience Treating Diabetes
Medicover offers expert diabetes care with personalised treatment plans, nutrition guidance, and emotional support. We are dedicated to helping patients manage their health through ongoing care and regular monitoring.