What Is an ERCP (Endoscopic Retrograde Cholangiopancreatography)?
Endoscopic retrograde cholangiopancreatography, or ERCP, is a medical procedure that combines endoscopy and X-ray imaging to diagnose and treat problems in the:
- Liver
- Gallbladder
- Bile ducts
- Pancreas
A flexible tube with a camera (endoscope) is passed through the mouth and into the small intestine. Contrast dye is then injected into the bile and pancreatic ducts, and X-rays are taken to look for blockages, stones, or other abnormalities.
How Does ERCP Work?
ERCP serves both as a diagnostic test and a treatment procedure:
- Diagnosis: It helps identify the cause of symptoms such as jaundice, unexplained abdominal pain, pancreatitis, or abnormal blood test results.
- Treatment: During the procedure, doctors can remove gallstones, place stents to open blocked ducts, or take tissue samples (biopsies).
ERCP is typically performed by a gastroenterologist, a doctor specializing in digestive system disorders.
30-60 minutes
Surgery Duration
Outpatient (same-day)
Hospital Stay
1-2 Days
Full Recovery Timeline
What conditions does ERCP treat?
ERCP can both diagnose and treat a wide range of conditions, including:
- Jaundice: Identifying and managing bile duct obstructions causing yellowing of the skin and eyes
- Gallstones or bile duct stones: Locating and removing stones that cause pain, infection, or pancreatitis
- Abdominal pain: Investigating unexplained pain when other tests are inconclusive
- Bile duct narrowing (strictures): Treating blockages from tumors, scarring, or inflammation
- Chronic pancreatitis: Assisting in diagnosis and relieving duct blockages related to long-term inflammation
- Pancreatic disorders: Managing duct blockages, leaks, or strictures within the pancreas
- Tumors: Detecting and assessing growths in the pancreas or bile ducts
- Sphincter of Oddi dysfunction: Evaluating and treating problems with bile flow caused by abnormal sphincter muscle function
- Fluid drainage: Draining pseudocysts or fluid collections around the pancreas
- Post-surgery complications: Treating bile or pancreatic duct issues that develop after operations
- Duct anatomy evaluation: Providing detailed imaging for complex duct structures before surgery or further treatment.
Why is an ERCP done?
ERCP is performed to find and treat issues that affect how bile and pancreatic juices flow through your body. Unlike imaging tests that only show pictures, ERCP allows your provider to take action during the procedure, such as removing stones, placing stents, or opening narrowed ducts.
It is often used when symptoms suggest a problem in the biliary or pancreatic system, and less invasive tests are not enough to guide treatment.
Who needs an ERCP Procedure?
You may need an ERCP if you have symptoms or test results pointing to a blockage or dysfunction in the bile or pancreatic ducts.
This includes people who have:
- Jaundice (yellowing of the skin or eyes)
- Abdominal pain that may be linked to the gallbladder or pancreas
- A history of gallstones, especially if they may have moved into the bile duct
- Pancreatitis (inflammation of the pancreas), especially if it keeps coming back
- Known or suspected tumors in the bile ducts or pancreas
- Fluid collections like pseudocysts near the pancreas
- Complications after gallbladder or liver surgery
- Unexplained weight loss or digestive issues linked to bile flow
Your provider will review your symptoms, lab results, and imaging studies before recommending ERCP.
When would a doctor recommend it?
Your provider may recommend ERCP when:
- You have jaundice and imaging shows a blocked bile duct
- You've had pancreatitis and a stone or stricture is suspected
- Other tests cannot explain your abdominal pain or liver enzyme changes
- A tumor is blocking the bile or pancreatic duct and needs stenting
- You need bile duct stones removed
- You have a fluid collection that can be drained through the digestive tract
ERCP is not used for routine screening. It is recommended when there is a clear need for diagnosis or treatment that can be done during the same procedure.
How Should I Prepare for an ERCP Procedure?
Preparation starts days before your ERCP. The goal is to make the process as smooth and safe as possible.
Talk openly with your provider about your full medical history. Mention any allergies, past surgeries, or conditions like liver disease, pancreatitis, or heart and lung problems. This helps your care team choose the safest approach, especially when it comes to sedation.
You'll need someone to drive you home. Sedation affects your coordination and judgment, so you cannot drive for at least 24 hours. Plan, don't schedule the procedure without a ride lined up.
On the day of the procedure:
- Wear comfortable, loose-fitting clothes
- Leave jewelry, watches, and valuables at home
- Bring a list of all your medications, including dosages
- Pack your insurance card and photo ID
Most people go home the same day. After the procedure, plan to rest. Avoid work, exercise, and complex tasks for the rest of the day.
Your healthcare provider may provide you with special instructions tailored to your health. If anything is unclear, call your care team. They're there to help.
What tests are done before ERCP?
Not everyone needs preoperative testing, but your provider may order a few simple tests to guide your care.
These may include:
- Blood tests to check liver function, kidney health, and blood clotting ability
- Imaging studies like ultrasound, CT, or MRI to view the bile and pancreatic ducts
- Pregnancy test if you're a woman of childbearing age. X-rays are used during ERCP
- EKG (electrocardiogram) if you have heart disease or are older than 50
These tests aren't meant to delay your care; they help your gastroenterologist plan the safest, most effective procedure.
Should I stop eating, drinking, or taking medicines?
Yes. Your instructions will depend on the type of anaesthesia planned:
Fasting:
- Stop eating solid foods at least 6-8 hours before the procedure
- Stop drinking clear liquids 2-4 hours before the procedure
Medications:
- Continue most regular medicines unless told otherwise
- Blood thinners (warfarin, aspirin, clopidogrel, etc.) may need to be paused to reduce bleeding risk
- Diabetes medicines may need adjustment because of fasting
- Never stop any medication without your provider's approval.
Steps Involved During an ERCP Procedure
You'll start by lying on your left side on an exam table. A team of skilled nurses and a gastroenterologist, a doctor who specialises in digestive health, will be with you throughout.
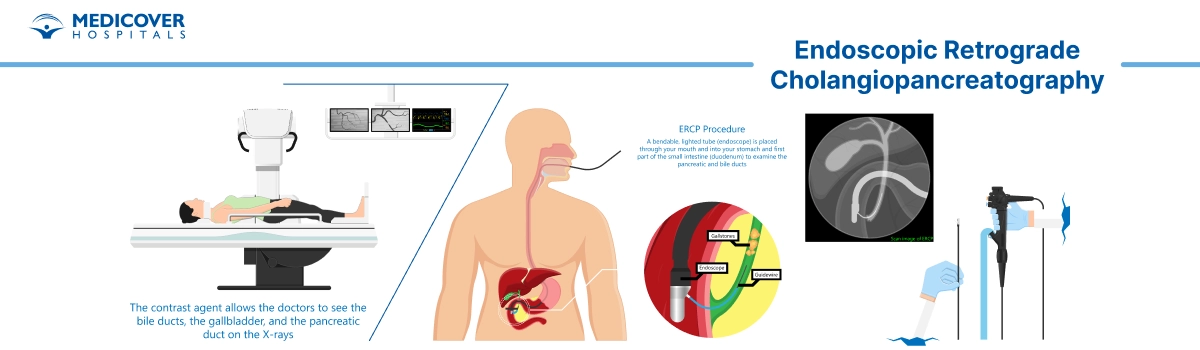
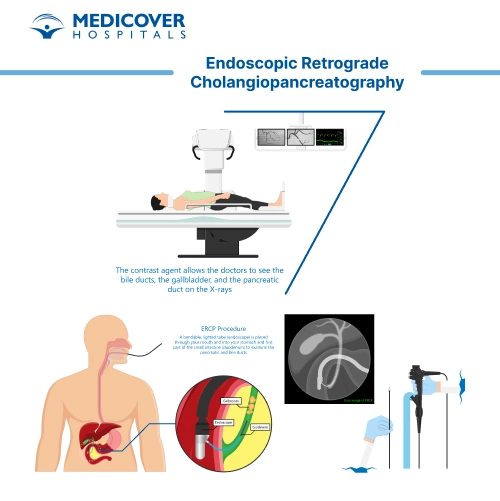
Before the procedure begins, you'll receive sedation to keep you relaxed and comfortable. Once the medication takes effect, the doctor will gently guide a thin, flexible tube called an endoscope through your mouth, down your esophagus, through your stomach, and into the first part of your small intestine (the duodenum).
This may sound uncomfortable, but most people don't feel it due to the sedation. You might be asked to swallow at the beginning to help the scope move smoothly.
Once the endoscope reaches the opening of the bile and pancreatic ducts, a small catheter is passed through the scope into the ducts. A special dye is injected so the ducts can be seen clearly on X-ray images.
These real-time images help your provider spot blockages, stones, narrowing, or tumors. If a problem is identified, treatment can often be initiated promptly.
Common interventions include:
- Removing bile duct stones using tiny baskets or balloons
- Placing a stent to keep a narrowed duct open
- Taking tissue samples (biopsies) for lab testing
- Draining fluid from pseudocysts near the pancreas
- Performing a sphincterotomy (a small cut) to improve bile or pancreatic juice flow
After all the needed steps are complete, the endoscope is slowly and carefully removed.
What type of anesthesia is used?
You'll receive intravenous (IV) sedation, which makes you deeply relaxed and may make you sleep through most of the procedure. This is also called "conscious sedation" You're not fully asleep, but you're calm and won't feel pain.
Some patients receive deeper sedation or general anesthesia, especially if the procedure is expected to be complex or if they have certain medical conditions.
You won't need to breathe through a tube in most cases, and you'll continue to breathe on your own. The sedation team continuously monitors your heart rate, blood pressure, and oxygen levels throughout the procedure.
Because of the sedation, you'll need someone to drive you home and stay with you for the rest of the day.
How long does ERCP take?
The ERCP procedure typically lasts between 30 and 90 minutes, depending on the findings and whether treatment is required.
Afterwards, you'll spend 30 minutes to a few hours in a recovery area while the sedation wears off. Nurses will check your vital signs and make sure you're stable before you go home.
Most people go home the same day. If you have had a stent placed or fluid drained, your provider may recommend a short observation period; however, overnight stays are rare.
Who performs the ERCP procedure?
ERCP is performed by gastroenterologists who have advanced training in endoscopy and biliary-pancreatic disorders. These specialists are often referred to as therapeutic endoscopists because they not only diagnose but also treat during the same procedure.
Your care team will include nurses and technicians trained in GI procedures. Everyone works together to ensure your comfort and safety.
You'll know who's performing your ERCP ahead of time, and you can ask questions before it begins.
What to Expect During Recovery After an ERCP Procedure?
Recovery after an ERCP is typically quick, and most people return to normal within a day or two. While everyone heals at their own pace you can expect to go home the same day and begin feeling better soon after the procedure.
Your care team will guide you through each step and inform you about the signs to watch for.
How long does recovery take after an ERCP?
Most people recover within 24 to 48 hours, although full healing may take a few days to a week, depending on the procedure performed. If stones are removed, a stent is placed, or a stricture is treated, you may experience mild discomfort for a short time.
If no major intervention was needed, you might feel fine by the next day. Some people develop mild pancreatitis after an ERCP, which is a known but uncommon risk, and it can extend recovery by a few days.
In rare cases, complications may require a longer recovery or a brief hospital stay. For most, the process is smooth and uncomplicated.
What should I expect immediately after an ERCP?
After the procedure, you will be taken to a recovery area where nurses will monitor your breathing, heart rate and alertness. You may feel:
- Drowsy or groggy from the sedation, which is normal and will fade as the medication wears off
- Bloating or gas in your abdomen due to air used during the procedure, passing gas, or burping will help relieve it
- A mild sore throat from the endoscope passing through your throat, which usually goes away in 1 or 2 days
- Mild cramping or discomfort in your bell, which should improve quickly
Once you are awake, you will be offered sips of water. If all goes well, you can gradually resume clear liquids and then a light meal before going home. Your provider or nurse will discuss the results with you before you leave or the next day, outlining what was found and what comes next.
When can I return to normal activities after an ERCP?
You should rest for the rest of the day after your ERCP. Most people can return to light activities within 24 hours. Here is a general guide:
- Driving and operating machinery: Avoid for at least 24 hours due to sedation
- Work: If your job is desk-based, you may return the next day. For physical jobs, wait 1-2 days or follow your provider's advice.
- Eating: Start with clear liquids and progress to a light diet. A low-fat diet may be recommended if you have pancreatic or gallbladder concerns.
- Exercise and heavy lifting: Avoid for at least 24 to 48 hours. Ask your provider when it's safe to resume.
Listen to your body. If you feel weak, dizzy or unwell, keep resting.
Are lifestyle changes required after recovery from an ERCP?
Depending on the findings of the ERCP, your provider may recommend long-term changes to support your digestive health. These are not needed for everyone, but may include:
- Diet changes: A low-fat diet may help if you have gallstones, chronic pancreatitis or bile duct issues. Avoid greasy fried or heavy meals that can trigger pain
- Alcohol: Limit or avoid alcohol if you have liver disease, pancreatitis or bile duct problems
- Smoking: Quitting improves healing and lowers the risk of complications. Your provider can help connect you with support programs.
- Hydration: Drink plenty of water unless told otherwise, especially if recovering from infection or dehydration
- Medications: Take all prescribed medicines as directed, including antibiotics, pain relievers or drugs to manage bile flow
- Weight management: Maintaining a healthy weight can reduce the risk of gallstones and improve digestion
- Follow-up care: Attend all scheduled appointments as scheduled. You may need repeat imaging, blood tests or stent checks.
- Symptom monitoring: Report any new or worsening symptoms such as fever, severe abdominal pain, nausea, vomiting or yellowing of the skin or eyes
- Stress management: Deep breathing, meditation, gentle walking or yoga can support healing and overall well-being
These changes are only recommended if they apply to your condition.
What Are the Risks and Benefits of an ERCP Procedure?
ERCP (endoscopic retrograde cholangiopancreatography) is a valuable procedure that can diagnose and treat conditions affecting the bile ducts, gallbladder, and pancreas. For many people, it provides both answers and treatment in one step, often avoiding surgery. But like any medical procedure, it has both benefits and possible risks.
What are the benefits of the ERCP procedure?
An ERCP can provide answers and treatment in a single step, often avoiding the need for surgery. It allows your provider to see inside your bile and pancreatic ducts, identify blockages, and treat them right away.
Common benefits include:
- Removing stones from the bile duct that are causing pain, infection, or pancreatitis
- Placing stents to keep narrowed ducts open and restore proper flow of bile or pancreatic juice
- Draining fluid collections such as pseudocysts near the pancreas
- Taking tissue samples to check for cancer or inflammation
- Relieving jaundice by clearing a blocked bile duct
- Diagnosing the cause of unexplained abdominal pain or abnormal liver tests
Because ERCP is both diagnostic and therapeutic, many people get immediate relief and avoid more invasive procedures.
What are the risks and complications of ERCP surgery?
While ERCP surgery is generally safe, rare complications can occur. Your provider will only recommend it when the benefits clearly outweigh the risks.
The most common complication is pancreatitis, or inflammation of the pancreas, which can happen when the pancreatic duct is irritated during the procedure. Most cases are mild and improve with fluids and monitoring, but some may require a hospital stay.
Other possible complications of ERCP surgery include:
- Pancreatitis (inflammation of the pancreas) is the most common complication after ERCP.
- Infection in the bile ducts or pancreas can occur, especially if a blockage is present.
- Bleeding may happen if a cut is made in the bile duct or if a biopsy is taken.
- Perforation (a small tear) in the esophagus, stomach, or intestines can occur, though it's rare.
- Allergic reactions to the dye or sedatives used during the procedure.
- Heart or breathing problems related to sedation or anesthesia.
- Bile leakage occurs if a duct is accidentally injured.
Most complications are uncommon and treatable when caught early.
What are the side effects after an ERCP procedure?
Side effects after an ERCP procedure are usually mild and go away within a day or two.
You may experience:
- A sore throat from the endoscope
- Bloating or gas from air used during the procedure
- Mild cramping or discomfort in your abdomen
- Drowsiness from sedation that lasts a few hours
These are normal and expected. They do not mean something went wrong.
More serious symptoms, such as severe abdominal pain, fever, vomiting, or jaundice, are not side effects. They could be signs of a complication and should be reported right away.
How much does an ERCP (Endoscopic Retrograde Cholangiopancreatography) procedure cost in India?
The price typically ranges from about Rs. 15,000 to Rs. 80,000, but in some cases it may be as low as Rs. 11,000 or as high as Rs. 88,000. The final cost depends on several factors, including the hospital's reputation and location, the surgeon's experience, whether additional procedures like stenting or stone removal are needed, and the length of the hospital stay.













































