What is Peptic Ulcer Disease?: All You Need To Know
Written by Medicover Team and Medically Reviewed by Dr Manoj Chandrakant Kolhe , Gastroenterologists Medical
Peptic ulcer disease is a condition in which the lining of the stomach or the first part of the small intestine develops painful sores or ulcers (the duodenum).
The stomach lining is normally protected from the effects of its digestive fluids by a thick layer of mucus. However, a variety of factors can weaken this barrier, allowing stomach acid to harm the tissue.
Gastric ulcers and duodenal ulcers are the two most prevalent forms of peptic ulcers. These designations indicate the location of the ulcer.
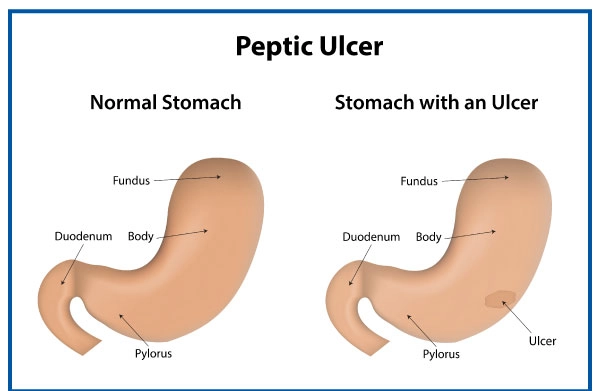
Ulcers in the stomach are known as gastric ulcers. Duodenal ulcers are found in the duodenum, which is the first part of the small intestine (also known as the small bowel). Both stomach and duodenal ulcers can occur at the same time.
What Are the Different Types of Peptic Ulcers?
Peptic ulcers are sores that develop on the inside lining of your stomach or small intestine. They can cause pain, discomfort, and other digestive issues. Knowing the different types of ulcers can help you better understand your symptoms and treatment options.
Gastric Ulcer
- Location: Inside the stomach
- Common Symptoms: Burning stomach pain, nausea, loss of appetite
- Often Worsens: After eating
Duodenal Ulcer
- Location: First part of the small intestine (duodenum)
- Common Symptoms: Burning or gnawing pain in the upper abdomen
- Often Improves: After eating, but may return 2-3 hours later or at night
Esophageal Ulcer
- Location: Lower part of the esophagus
- Common Symptoms: Chest pain, difficulty swallowing, acid reflux symptoms
- Causes: Often related to severe acid reflux (GERD)
Stress Ulcer
- Location: Stomach or duodenum
- Causes: Physical stress from serious illness, surgery, or injury
- Often Found In: Critically ill or hospitalized patients
Refractory Ulcer
- Definition: A peptic ulcer that doesn't heal after 8-12 weeks of treatment
- Causes: Ongoing H. pylori infection, continued NSAID use, or other underlying conditions
The bacteria Helicobacter pylori (H. pylori) infection and long-term usage of NSAIDs like ibuprofen causesulcer.There is no link between stress and peptic ulcers, but they might exacerbate the ulcer symptoms.
What are the Peptic Ulcer Symptoms and Warning Signs?
Many people who have ulcers don't show any signs or symptoms at all. Some people with ulcers experience stomach pain, frequently felt in the upper abdomen.
Food might make the pain go away, but it can also make it worse. Nausea, vomiting, and a sense of being bloated or full are some other symptoms.
It's vital to understand that there are a variety of causes for stomach pain, and not all abdominal discomfort is an 'ulcer'.
Some people might face mild to moderate symptoms. These symptoms include:
- Gnawing or burning pain
- Bloating
- Heartburn
- Nausea or vomiting
- Dark or black stool
- Weight loss
- Severe pain in the upper abdomen
- Trouble while breathing
- Changes in appetite
- Chest pain
- Indigestion
Peptic Ulcer Causes
When the inner surface of the stomach or small intestine is attacked by digestive acids it leads to a peptic ulcer. The acid causes a painful open sore and it may bleed. A mucous layer covers the digestive tract, which often shields the tract from the acid. An ulcer may develop if the amount of acid is increased or the intensity of mucus is decreased. Other causes are:
H. Pylori Bacteria
The H. pylori bacteria attach to the mucus layer in the digestive tract and create inflammation (irritation), which can lead to the breakdown of this protective coating. Because your stomach includes powerful acids to digest food, this breakdown is a concern. Acids can eat through stomach tissue without the mucus layer protecting it.
Pain Killers
You're more prone to develop a peptic ulcer if you take aspirin frequently and for a long time. Other nonsteroidal anti-inflammatory medications are in the same boat (NSAIDs). Ibuprofen and naproxen are two of them.
NSAIDs prevent your body from producing a substance that protects your stomach and small intestine from stomach acid. Other pain relievers, such as acetaminophen, will not cause ulcers.
Different medicines
Combining certain additional drugs with NSAIDs can significantly increase the risk of getting ulcers. These include steroids, anticoagulants, aspirin, selective serotonin reuptake inhibitors (SSRIs), alendronate, and risedronate-containing tablets.
Get a second opinion from trusted experts and makeconfident, informed decisions.
What are the Risk Factors for Peptic Ulcer Disease?
You may be at a higher risk of developing peptic ulcers in addition to the hazards associated with taking NSAIDs in the following situations:
- Smoking increases the risk of peptic ulcers in people having H. pylori infection.
- Alcohol elevates stomach acid production that can irritate and erode the mucus lining of the stomach.
- Take a lot of stress.
- Eat hot and very spicy food.
These elements together do not create ulcers, but they can exacerbate the existing ulcers and make them difficult to treat.
Diagnosis for Peptic Ulcer
A barium upper gastrointestinal X-ray (upper GI series) or an upper gastrointestinal endoscopy are used to diagnose an ulcer (EGD or esophagogastroduodenoscopy).
The barium upper gastrointestinal (GI) X-ray is simple to produce and has little risk or discomfort (apart from radiation exposure). Barium is a white, chalky material that is taken orally.
It shows up on X-rays and allows doctors to view the contour of the stomach; however, barium X-rays are less reliable and can miss ulcers up to 20% of the time.
An upper gastrointestinal endoscopy is more precise than X-rays. Still, it requires the patient to be sedated and the insertion of a flexible tube via the mouth to examine the esophagus, stomach, and duodenum.
Upper endoscopy provides the extra benefit of being able to take small tissue samples (biopsies) to test for H. pylori infection.
H. pylori tests are now commonly available, and your doctor will design a treatment plan to alleviate your symptoms while also killing the bacteria.
The quickest way to find out if you have H. pylori is to do a breath test. A blood or stool test, or a sample taken during an upper endoscopy, can also be used to check for it.
What are the Peptic Ulcer Treatment Options?
The treatment for your ulcer will be determined by the underlying cause. Your doctor will prescribe a combination of medications if tests reveal that you have an H. pylori infection. The drugs must be taken for up to two weeks.
Antibiotics are used to fight infections, and proton pump inhibitors (PPIs) are used to lower stomach acid.
Antibiotic regimens may cause mild side effects such as diarrhea or stomach distress. Consult your doctor if these side effects cause substantial discomfort or do not improve over time.
Suppose your doctor finds that you do not have an H. pylori infection. In that case, he or she may prescribe or recommend an over-the-counter PPI (such as Prilosec or Prevacid) for up to 8 weeks to reduce digestive enzymes and aid in the healing of your ulcer.
Acid blockers, such as famotidine (Pepcid), can help with stomach acid and ulcer pain. These drugs are available with a prescription and over the counter in some areas.
When to See a Doctor for Peptic Ulcer?
A peptic ulcer is a sore that forms in the lining of the stomach or the upper part of the small intestine. It can cause pain and discomfort, and if left untreated, may lead to serious complications like bleeding or infection.
You should see a doctor if you experience:
- Burning stomach pain, especially between meals or at night
- Pain that improves when eating, drinking milk, or taking antacids
- Nausea, bloating, or a feeling of fullness
- Unexplained weight loss
- Frequent indigestion or heartburn
- Vomiting blood or material that looks like coffee grounds
- Black, tarry stools
- Sudden, sharp stomach pain
- Fainting or dizziness
High-risk groups needing prompt care
- People who take pain relievers (NSAIDs) regularly
- Those with a history of ulcers or digestive issues
- Individuals with H. pylori infections
- People who smoke, drink heavily, or are under high stress
Early diagnosis and treatment can help heal the ulcer and prevent complications.
Your health is everything - prioritize your well-being today.
What Is the Recovery Process After Peptic Ulcer Treatment?
With proper treatment, most peptic ulcers heal completely within 4 to 8 weeks. Medications like acid reducers and antibiotics (if H. pylori is involved) are highly effective, and many people only need a short course of therapy.
If the ulcer was caused by H. pylori, follow-up tests may be needed to confirm the bacteria are fully cleared. In some cases, the infection may return, or a new ulcer can form, especially if risk factors like NSAID use, smoking, or untreated stress continue.
Most people recover well, but a small number may have recurrent or non-healing ulcers. These cases can lead to complications like bleeding, scarring, or stomach outlet blockage, and may require further treatment or surgery such as:
- Pyloroplasty: To widen the stomach's outlet and improve food flow
- Vagotomy: To reduce acid production by cutting specific stomach nerves
Ongoing care and lifestyle changes, like avoiding certain medications and managing stress, play a key role in preventing ulcers from coming back.
What are the Complications of Peptic Ulcer?
People with ulcer disease can live regular lives without food restrictions or lifestyle adjustments because of contemporary treatment. It has been discovered that smokers have a higher risk of ulcers and treatment failure.
The bacteria H. pylori is eradicated, which not only heals ulcers but also prevents them from recurring. Patients with ulcers usually have a good quality of life. Some ulcers are likely to heal without the need for drugs (though they probably recur as well).
As a result, the most serious issues that arise as a result of ulcers are ulcer complications. Some complications include:
- Bleeding
- Perforation
- Obstruction of emptying the passage of blood
- Weakness
- Orthostatic hypotension
- Blood vomiting
Blood transfusions may be required for patients who have persistent or severe bleeding. With the help of specialist endoscopic devices, an endoscopy is conducted to determine the source of bleeding and to stop active ulcer bleeding.
Home Remedies for Peptic Ulcer
While medical treatment is essential for healing peptic ulcers, some home remedies may help relieve symptoms and support recovery. These remedies should be used alongside, not instead of, doctor-prescribed medication.
Helpful Lifestyle and Natural Remedies:
- Eat Small, Frequent Meals: Large meals can increase acid production. Eating smaller portions more often reduces pressure on your stomach and may ease discomfort.
- Try Probiotics: Foods like yogurt, kefir, sauerkraut, and kombucha contain probiotics, which help restore healthy gut bacteria and may assist in fighting H. pylori, the bacteria linked to many ulcers.
- Include Fiber-Rich Foods: Oats, apples, carrots, and legumes are gentle on the stomach and may help reduce acid levels while promoting healing.
- Drink Cabbage Juice (in moderation): Some studies suggest that cabbage juice may support ulcer healing due to its glutamine content, which helps repair stomach lining.
- Honey: Raw honey has natural antibacterial properties. A spoonful on an empty stomach may help soothe ulcer symptoms and promote healing.
- Deglycyrrhizinated Licorice (DGL): This herbal supplement (not regular licorice) may support the stomach lining and reduce inflammation. Always consult your doctor before use.
- Avoid Trigger Foods: Spicy, fried, acidic, or heavily caffeinated foods may irritate the ulcer. Identify your triggers and adjust your diet accordingly.
Our Experience Treating Peptic Ulcers
At Medicover, we provide comprehensive care for patients with peptic ulcers, focusing on fast relief, healing, and long-term digestive health. Our experienced team of gastroenterologists and dietitians works together to diagnose and manage ulcers with care and precision.
We offer:
- Advanced endoscopy and lab testing to identify ulcers and their causes
- Treatment plans that may include acid-reducing medications and antibiotics (for H. pylori)
- Dietary guidance to reduce symptoms and prevent flare-ups
- Ongoing care and monitoring to promote full recovery
Whether you're dealing with recurring stomach pain or a newly diagnosed ulcer, We are here to support you every step of the way, with expert care, a listening ear, and a path toward healing.