Heart Attack: Symptoms, Causes, Prevention, Diagnosis
Written by Medicover Team and Medically Reviewed by Dr Ravindra Amujuru , Cardiologist
Heart attack, also known as myocardial infarction. A heart attack happens when the blood flow to a part of your heart suddenly gets blocked. Your heart muscle needs oxygen-rich blood to work properly. When that flow stops, even for a few minutes, it can damage or kill part of the heart muscle.
This usually happens because of a buildup of fat and cholesterol in the arteries, which forms a plaque. If the plaque breaks, it can form a blood clot that blocks the flow.
Important things to remember:
- A heart attack is a medical emergency, call for help immediately.
- Acting fast can save your life and limit damage to the heart.
- Even if symptoms are mild, they should never be ignored.
Not everyone has the same symptoms. Some people may not even feel chest pain, especially women and older adults.
Cardiac Arrest vs Heart Attack: What's the Difference?
People often confuse a heart attack and cardiac arrest, but they're not the same. They both affect the heart, but in very different ways.
What is a Heart Attack?
- Caused by a blockage in the arteries
- Blood flow to the heart muscle is reduced or stopped
- The heart keeps beating, but not properly
- Person is usually awake and breathing
What is Cardiac Arrest?
- Caused by a sudden electrical issue in the heart
- The heart suddenly stops beating
- A person collapses and becomes unconscious
- Breathing stops almost immediately
Key differences to know:
- A heart attack is a circulation problem. The heart doesn't get enough blood.
- A cardiac arrest is an electrical problem. The heart suddenly stops pumping.
- A heart attack can lead to cardiac arrest if not treated quickly.
- Cardiac arrest happens suddenly and without warning, CPR and immediate care are critical.
What Are the Heart Attack Symptoms?
A heart attack happens when blood flow to the heart is blocked. This is a medical emergency, and knowing the symptoms can save lives. While some symptoms develop suddenly and intensely, others emerge gradually and can be easily overlooked.
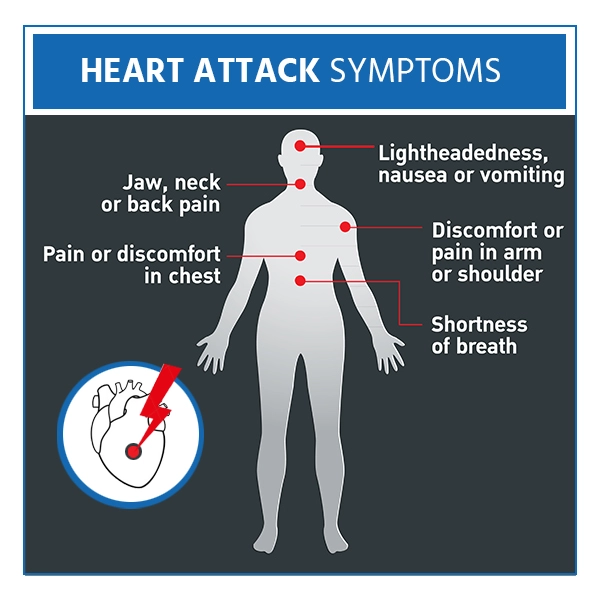
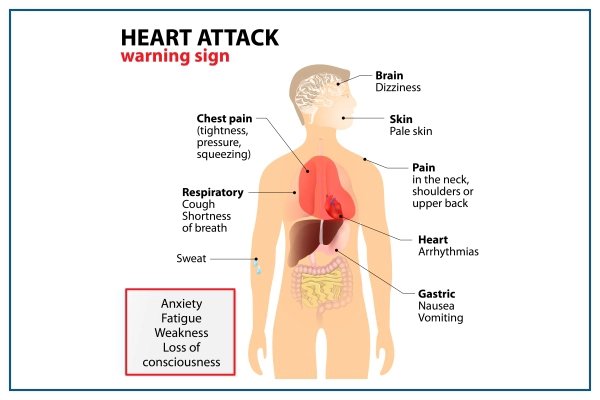
Most people describe the feeling as pressure, tightness, or pain in the chest, but symptoms can affect other parts of the body too.
- Chest pain that may feel like tightness, pressure, pain, aching or squeezing.
- Pain or discomfort that spreads to the arm, shoulder, neck, back jaw, and teeth
- Shortness of breath
- Heartburn or indigestion
- Lightheadedness
- Sudden dizziness
- Nausea
- Fatigue
- Cold sweat
Not everyone feels all these symptoms. Some people may only have mild pain, while others might not have chest pain at all. That's why it's important to listen to your body.
If you think you or someone else may be having a heart attack, call emergency services right away. Acting fast makes a big difference.
Heart Attack Symptoms in Women and Men
Heart attack symptoms can look different in women and men. While chest pain is a common warning sign for both, women often have additional or unusual symptoms that can be mistaken for other conditions.
Common Symptoms of Heart Attack in Men
- Chest pain or pressure (classic “elephant on the chest†feeling)
- Pain in the left arm or shoulder
- Sweating, shortness of breath
- Feeling dizzy or faint
- Nausea
Common Symptoms of Heart Attack in Women
- Chest pain or discomfort (can feel more like squeezing or fullness)
- Unusual tiredness that lasts for days
- Pain in the neck, jaw, or back
- Shortness of breath
- Nausea or vomiting
- Light-headedness
Women are more likely to overlook these signs because they're not as obvious as chest pain. Many women think it's just stress or indigestion.
What are the Causes of Heart Attack?
Most of the heart attacks are caused by coronary artery disease. One or more of the heart's (coronary) arteries are blocked in coronary artery disease, and this is typically caused by cholesterol-containing deposits known as plaques.
Plaques can cause artery narrowing, limiting blood flow to the heart.
When a plaque breaks down, it might create a blood clot in the heart.
However, a heart attack can be caused by a total or partial blockage of a coronary artery in the heart. One way to identify heart attacks is when an electrocardiogram (ECG or EKG) reveals certain changes (ST elevation) that necessitate immediate invasive treatment. Your doctor may use ECG data to describe various sorts of heart attacks.
- Acute total blockage of a medium or large heart artery usually indicates an ST-elevation myocardial infarction (STEMI).
- A partial blockage frequently indicates a non-ST elevation myocardial infarction (NSTEMI). Some persons with NSTEMI, however, have a complete blockage.
Not all heart attacks are caused by blocked arteries. Here are the other reasons for heart attack:
- Coronary artery spasm: The artery typically exhibits cholesterol plaques or early stiffening owing to smoking or other risk factors. Coronary artery spasms are sometimes known as Prinzmetal's angina, vasospastic angina, or variant angina.
- Certain infections, such as COVID-19 and other viral infections, can harm the cardiac muscle.
- Spontaneous coronary artery dissection (SCAD): A tear within a cardiac artery causes this possibly life-threatening condition.
Sometimes, a heart attack can happen even if your arteries aren't fully blocked. It may result from intense physical activity, emotional stress, or drug use.
Get a second opinion from trusted experts and makeconfident, informed decisions.
Get Second OpinionWho Is at Risk of a Heart Attack?
Anyone can have a heart attack, but some people are more likely to face one because of their lifestyle, age, or health conditions. Knowing these risk factors can help you act early and protect your heart.
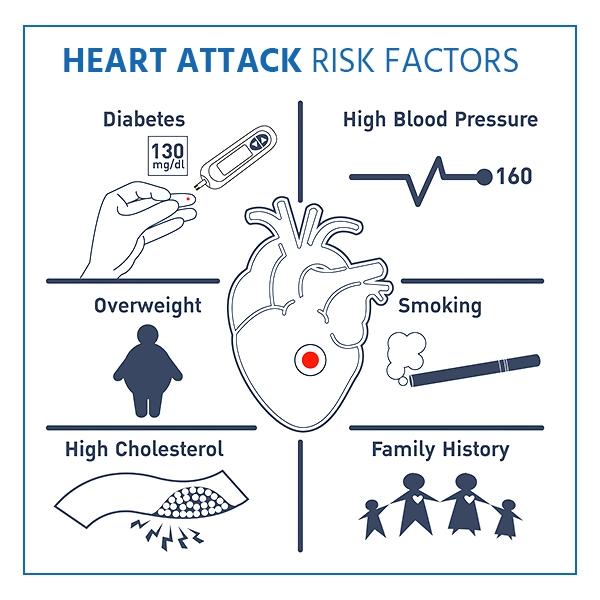
Here are the main risk groups:
- Age: Men over 45 and women over 55 of age are more likely than younger men and women to have a heart attack.
- Tobacco use: This includes smoking and long-term secondhand smoke exposure.
- High blood pressure: This can damage the arteries that lead to the heart over time. High blood pressure and other illnesses, such as obesity, high cholesterol, or diabetes, raise the risk even further.
- Obesity: Obesity is associated with high blood pressure, diabetes, high triglyceride and bad cholesterol levels, and low good cholesterol levels
- Diabetes: Blood sugar levels rise when the body does not produce or uses the hormone insulin properly. High blood sugar levels raise the chance of having a heart attack.
- Unhealthy diet: A diet heavy in sugar, animal fats, processed foods, trans fats, and salt raises the risk of heart disease.
- Stress: Extreme emotional stress, such as anger, may raise the chance of a heart attack.

How Doctors Diagnose Heart Attack?
When someone has symptoms like chest pain, shortness of breath, or a heavy feeling in the chest, doctors will act quickly to check if it's a heart attack. Early diagnosis is crucial in preventing heart damage and saving lives.
Doctors usually begin by asking about your symptoms, medical history, and risk factors like high blood pressure, smoking, or diabetes. They'll also listen to your heart and lungs and check your vital signs.
A quick diagnosis helps start treatment fast, sometimes even while tests are still running. The goal is to open blocked arteries and restore blood flow to the heart as soon as possible.
A heart attack is diagnosed by monitoring blood pressure, pulse, and temperature. Tests are performed to determine how the heart is beating and to assess overall heart health.
What Tests Will Be Done to Diagnose a Heart Attack?
To confirm if you're having a heart attack, doctors rely on a few key tests. These tests help them see how your heart is working and whether there's been any damage.
Here are the main tests used:
- Electrocardiogram (ECG or EKG): This is a test to diagnose a heart attack and monitors electrical impulses as they flow through the heart. Sticky patches (electrodes) are placed to the chest and, in certain cases, the arms and legs.
- Blood tests: After a cardiac attack, certain heart proteins progressively leak into the bloodstream. These proteins can be detected using blood testing (cardiac markers).
- Chest X-ray: A chest X-ray displays the condition and size of the heart and lungs.
- Echocardiogram: Ultrasound waves provide images of the beating heart. This test can reveal how blood flows through the heart and its valves.
- Coronary catheterization (angiogram): A long, thin tube (catheter) is guided to the heart after being inserted into an artery, generally in the leg.
- Cardiac CT or MRI: Cardiac exams, including X-rays and MRI, generate heart and chest images. X-rays use radiation, while cardiac MRI employs a magnetic field and radio waves. Patients lie on a table that slides into a tubelike machine for both tests. These diagnostics assess and quantify heart damage.
What Are the Treatment Options for a Heart Attack?
When someone has a heart attack, fast treatment can save their life and protect the heart from more damage. The main goal is to restore blood flow to the heart and prevent future attacks.
Doctors use a mix of medications, procedures, and lifestyle advice based on the severity of the attack. The type of heart attack treatment depends on whether blood flow is partially or completely blocked.
Surgical and other procedures for a heart attack
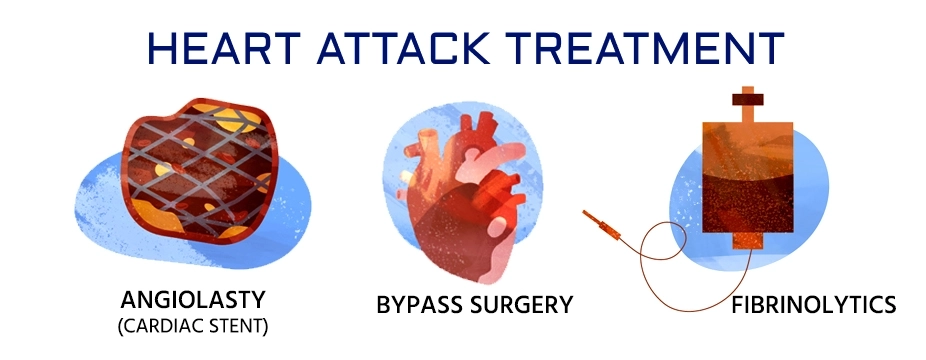
Surgery or a technique to unblock a blocked artery may be required if someone has had a heart attack. The following surgeries and procedures are used to treat a heart attack:
- Coronary angioplasty and stenting: This procedure clears blocked cardiac arteries. Percutaneous coronary intervention is another name for it (PCI). If you've had a heart attack, this treatment is generally performed as part of a procedure to detect blockages (cardiac catheterization). Angioplasty is performed by an expert cardiologist who directs a thin, flexible tube (catheter) to the constricted section of the heart artery. To help expand the blocked artery and improve blood flow.
- Coronary artery bypass graft (CABG): This is open-heart surgery. A surgeon uses a healthy blood artery from another part of the body to create a new path for blood in the heart. The blood then circulates the restricted or obstructed coronary artery. CABG can be performed as an emergency procedure in the event of a heart attack. It is sometimes done a few days later after the heart has recovered.
Medications for Heart Attack
Doctors often begin treatment with medicines to improve blood flow, reduce heart strain, and prevent future heart attacks. These may include:
- Anti-clotting medications: Help stop blood clots from getting worse
- Nitroglycerin: Relieves chest pain by widening blood vessels
- Thrombolytic (clot-busting) medications: Used in emergency to dissolve clots quickly
- Antiarrhythmia medications: Help correct abnormal heartbeats
- Pain medications: Reduce discomfort during and after a heart attack
- Beta-blockers: Lower heart rate and blood pressure to reduce heart's workload
- Antihypertensives: Control high blood pressure
- Statins: Lower cholesterol to keep arteries clear
Complications Caused by Heart Attack Treatment
While heart attack treatments save lives, some patients may face mild to moderate side effects or complications during recovery. Don't worry, most of these are manageable, and our medical team is here to guide you through every step. You're not alone in this.
Here are a few possible complications:
- Bleeding or bruising from blood-thinning medicines or procedures
- Irregular heartbeat (arrhythmia) after surgery
- Reaction to medications like dizziness or low blood pressure
- Infection at the catheter or incision site (though rare)
- Fatigue or emotional stress during recovery
Stay strong. With today's advanced treatments and individual care, these issues can be treated quickly.
When to See a Doctor For a Heart Attack?
If you think you're having a heart attack, don't wait, get medical help right away. Many people delay treatment, thinking the pain will go away. But with heart problems, every minute counts.
Here are signs that mean you should call a doctor or emergency services immediately:
- Chest pain or pressure that lasts more than a few minutes
- Pain spreading to your arm, back, neck, or jaw
- Shortness of breath, even at rest
- Cold sweats, dizziness, or nausea
- Unusual tiredness, especially in women
Sometimes, symptoms can feel mild, like heartburn or anxiety. But if something doesn't feel right, it's safer to get checked.
You should also see a doctor if you:
- Have frequent chest discomfort, even if it goes away
- Feel breathless during regular activities
- Have a family history of heart problems
- Have conditions like diabetes, high blood pressure, or high cholesterol
Your health is everything - prioritize your well-being today.
What Is the Recovery Process After Heart Attack Treatment?
Recovering from a heart attack doesn't happen overnight, but with the right steps, you can feel better and get back to your routine.
Here's what the recovery journey usually looks like:
First Few Days:
- Stay in the hospital for monitoring
- Doctors will check your heart and adjust medications
First Few Weeks:
- Start with light activities like walking
- Avoid heavy lifting or stressful tasks
- Take your medicines as prescribed
Long-Term Recovery:
- Join a cardiac rehabilitation program
- Eat heart-healthy foods (low salt, more fruits/vegetables)
- Exercise regularly, your doctor will guide you
- Manage stress and get enough sleep
- Avoid smoking and limit alcohol
Regular check-ups are very important. Your doctor may adjust your treatment based on how you're feeling.
Recovery is a journey, and every small step matters. At Medicover, our team will guide you with care, helping you build a healthier heart and a better life, one day at a time.
What Precautions Can Help Prevent a Heart Attack?
Preventing a heart attack starts with taking care of your heart every day. The good news is, even small changes in your daily habits can make a big difference over time. Here are some helpful ways to protect your heart:
Healthy Lifestyle Tips:
- Eat a heart-friendly diet: more fruits, vegetables, whole grains, and less salt, sugar, and fried food
- Stay active: aim for at least 30 minutes of walking or light exercise most days
- Avoid smoking and tobacco: it's one of the biggest risk factors for heart attacks
- Limit alcohol: too much can raise blood pressure and harm your heart
- Manage stress: deep breathing, yoga, or simply relaxing can help
- Maintain a healthy weight: even losing a few kilos can ease pressure on your heart
- Get regular check-ups: monitor blood pressure, cholesterol, and sugar levels
Heart attacks often happen after years of unnoticed buildup. Taking these precautions today can keep your heart stronger tomorrow. If you already have conditions like diabetes or high BP, staying on top of your medications is also key.
Complications of a Heart Attack
A heart attack can affect more than just your chest, it may lead to other health issues if not treated on time. That's why early care and follow-up are so important.
Short-Term Complications:
- Irregular heartbeat (arrhythmia): Your heart may beat too fast or too slow
- Heart failure: the heart can't pump blood properly, causing tiredness and swelling
- Cardiac arrest: sudden loss of heart function, which can be life-threatening
- Shock: very low blood pressure and oxygen levels in the body
Long-Term Complications:
- Weakened heart muscle: making it harder to do everyday tasks without feeling tired
- Repeat heart attacks: if the first one isn't well managed
- Depression or anxiety: Many patients feel emotional changes after a heart attack
- Lung problems: fluid buildup (called pulmonary edema) due to a weak heart
Even if you feel fine after a heart attack, follow-up care, lifestyle changes, and medications are essential to avoid these complications and live a healthier life ahead.
Our Experience Treating Heart Attack
If you or your loved one has experienced a heart attack, we want you to know, you are not alone.
At Medicover, we treat heart attack patients every single day, and we understand how frightening and overwhelming it can feel. But here's the good news: with timely treatment and the right care, most people recover and get back to living their lives.
Our experienced team of cardiologists and emergency care specialists are trained to act fast, because in heart care, every second counts. From the moment you arrive, we use advanced tools like ECGs, angiograms, and cardiac enzyme tests to assess your condition quickly.
We don't just treat the heart, we treat the person. Stay strong, ask questions, and lean on us. You don't have to go through this alone. We're here to help you heal and protect your heart for years to come.