Cirrhosis Disease: Diagnosis and Treatments
Written by Medicover Team and Medically Reviewed by Dr R Prasanth , Gastroenterologists Medical
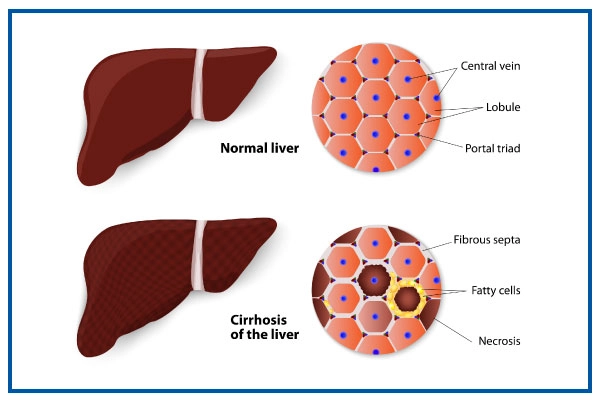
Cirrhosis, also called hepatic cirrhosis or liver cirrhosis, is an end-stage liver disease. This disease replaces healthy tissue with scar tissue known as fibrosis.
It starts growing and stops the liver from functioning normally. Cirrhosis can be fatal if it progresses to the point where the liver malfunctions.
What are the Stages of Liver Cirrhosis?
Cirrhosis doesn't happen overnight; it develops gradually through different stages as the liver gets damaged over time. Recognizing these stages helps patients and caregivers understand what's happening inside the body and when to take action.
Stage 1: Early Liver Stress
In the beginning, the liver shows signs of strain often due to alcohol, infections, or fat buildup. There might be mild inflammation, but many people don't feel any symptoms at this point. With the right changes in diet, habits, or medication, the liver can still bounce back.
Stage 2: Internal Scarring (Fibrosis)
Fibrosis as liver stress continues, scar tissue starts forming in small patches. The organ still functions, but not as efficiently. Most people don't realise their liver is under strain unless they go for routine tests. Catching it here offers a good chance to slow or even halt the damage.
Stage 3: Severe Damage (Cirrhosis)
At this point, the scarring becomes widespread and permanent. The liver begins to lose its ability to do its job filtering toxins, producing proteins, and helping digestion. Symptoms may occur like fatigue, swelling, and digestive issues. Complications like blood pressure buildup in the liver or fluid accumulation in the belly can develop.
Stage 4: Liver Failure
In the final stage, the liver stops working properly. The body starts showing serious signs like confusion, internal bleeding, or yellowing of the skin. This is a medical emergency, and in many cases, the only option left is a liver transplant.
Always act early. The sooner liver stress is diagnosed, the better the chances of controlling it. Don't wait for visible symptoms, regular health check-ups can make a life-saving difference.
What are the Cirrhosis Symptoms and Warning Signs?
Cirrhosis symptoms can vary depending on how much damage the liver has. In many cases, early signs may be mild and go unnoticed. But as the condition progresses, symptoms become more noticeable and may affect daily life.
Common Signs
- Feeling tired all the time or weak without much effort
- Ongoing nausea or poor appetite
- Discomfort or a heavy feeling in the belly
- Losing weight without trying
- Itchy skin, especially in specific areas
Advanced Signs
- Yellow skin or eyes (also called jaundice)
- Swelling in the stomach or ankles due to fluid build-up (ascites)
- Easy bruising or bleeding from minor injuries
- Blood in vomit or stools
- Confusion, forgetfulness, or trouble sleeping
- Enlarged spleen or bulging veins under the skin
- Dark-coloured urine that seems abnormal
If any of these symptoms continue or worsen, especially yellowing of the skin, swelling, bleeding, or confusion, please see a liver specialist without delay.
What are the Different Types of Cirrhosis?
Cirrhosis can develop from different health issues. Knowing the cause helps doctors decide the best treatment plan.
- Alcohol-related cirrhosis: Caused by long-term, heavy drinking
- NASH (Non-alcoholic steatohepatitis): Related to fat buildup in the liver, often linked to obesity
- Biliary cirrhosis: Caused by damage or blockage in the bile ducts
- Viral cirrhosis: Caused by long-term hepatitis B or C infections
Identifying the type of cirrhosis helps guide proper monitoring and treatment decisions.
What are the Common Causes and Risk Factors of Cirrhosis?
Cirrhosis happens when healthy liver tissue is slowly replaced with scar tissue. This process can result from long-term damage caused by certain illnesses or habits.
Common Causes
- Chronic infection with hepatitis B or C
- Drinking alcohol heavily over many years
- Fatty liver diseases such as NAFLD or NASH
- Autoimmune liver conditions
- Inherited disorders like Wilson's disease or hemochromatosis
- Injury or blockage in the bile ducts
Risk Factors
If you have these risk factors and start noticing symptoms like tiredness, appetite loss, or changes in digestion, it's important to speak to a doctor early.
Get a second opinion from trusted experts and makeconfident, informed decisions.
How Cirrhosis is Diagnosed?
Doctors use several steps to diagnose cirrhosis. They'll first ask about your health history, especially if you had liver problems, alcohol use, or hepatitis. Then they'll run tests to check how well your liver is working.
Diagnostic Methods
- Blood tests: These show liver function, blood counts, and clotting ability
- Scans: Ultrasound, CT, MRI, or elastography to measure liver stiffness
- Liver biopsy: A small sample of liver tissue (used only when needed) to confirm scarring
At Medicover, we use modern lab tests and advanced imaging to get accurate results, with support from our liver specialists for proper diagnosis and treatment planning.
What are the Treatment Options for Cirrhosis?
Treatment focuses on slowing liver damage, managing symptoms, and helping the liver work as well as possible. The type of treatment depends on how severe the cirrhosis is.
Medicines:
- Antiviral medicines for hepatitis
- Beta-blockers or vasodilators to reduce pressure in the liver
- Diuretics to control fluid retention
- Antibiotics to prevent or treat infections
Lifestyle changes:
- Stop drinking alcohol completely
- Eat a healthy, low-salt diet
- Lose extra weight and control diabetes or cholesterol
Procedures and Surgery:
- Endoscopic treatment for swollen veins (varices)
- Paracentesis to drain fluid from the belly
- TIPS (shunt procedure) for severe pressure in liver blood vessels
Our liver care teams monitor your progress regularly with tests and scans. For advanced cases, we also guide patients through transplant planning, ensuring timely decisions based on their health stage.
When to See a Doctor?
Early medical attention can help slow or stop liver damage. Get a doctor's help right away if you notice:
- Yellow skin or eyes
- Sudden or painful swelling in your belly
- Black stools or vomiting blood
- Confusion or trouble remembering things
- Feeling tired or dizzy often
High-risk people include:
- Those with long-term liver issues
- People who drink alcohol regularly
- Anyone with obesity, diabetes, or hepatitis
Your health is everything - prioritize your well-being today.
What is the Recovery Process After Cirrhosis Treatment?
How well someone recovers depends on how damaged the liver is and how early treatment begins. With regular care and healthy habits, many people can live better with cirrhosis.
Follow-up plan:
- Liver tests every 3 to 6 months
- Scans or elastography to check liver stiffness
- Watch for problems like bleeding veins or confusion
Everyday tips for recovery:
- Eat low-salt meals and drink clean water
- Avoid alcohol and unnecessary medications
- Stay active with safe, doctor-approved exercises
We also provide nutrition advice, mental health support, and regular reviews with liver doctors to keep your recovery on track.
What Precautions Can Help Prevent Cirrhosis?
Many cirrhosis cases can be avoided with good habits and early care. Following simple steps can protect your liver and lower your risk of long-term damage.
- Avoid or stop drinking alcohol
- Get vaccinated for hepatitis B
- Eat a balanced diet and stay at a healthy weight
- Go for regular liver checkups if you're at risk
- Practice safe hygiene and avoid risky behaviours to prevent infections
If not treated, cirrhosis can lead to:
- Liver failure
- Bleeding due to high liver pressure
- Brain problems like confusion (encephalopathy)
- Higher risk of liver cancer
Our Experience Treating Cirrhosis
At Medicover, we care for people with cirrhosis using the best medical tools and experienced doctors. From early diagnosis to transplant planning, we guide each patient with care and clarity.
We aim to protect your liver, improve your health, and support your recovery every step of the way.