What is Jaundice Disease?
Written by Medicover Team and Medically Reviewed by Dr Harshal Rajekar, Gastroenterology
Jaundice is a condition where the skin, eyes, and mucous membranes and sometimes other parts of the body, turn yellow due to a buildup of a substance called bilirubin in the blood.
Bilirubin is a yellow pigment produced when red blood cells die naturally in the body. Normally, the liver filters bilirubin from blood, mixes it with bile, and removes it from the body through stool. When this process is stopped, the bilirubin levels are overloaded in your blood. This is called hyperbilirubinemia, leading to jaundice.
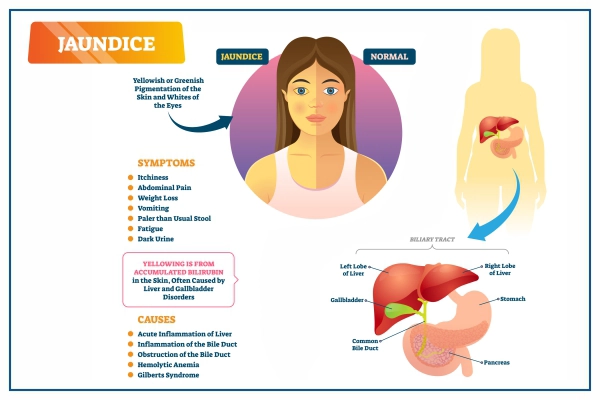
Jaundice is not a disease itself. It is a symptom that indicates something is wrong with liver function. This may be due to medical conditions, like hepatitis, gallstones and tumors.
In a community study from Alwar, Rajasthan, researchers identified 192 jaundice cases over one year within a population of 69,440, resulting in an annual incidence of approximately 2.76 per 1,000 people. Hospital-based data from southern India found that among acute viral hepatitis cases, 45.5% were caused by hepatitis E, 33% by hepatitis A, and 12.5% by hepatitis B, indicating that viral hepatitis is a leading cause of jaundice in India.
What are the Different Types of Jaundice?
The types of Jaundice are classified based on how the processing of bilirubin is disrupted. Knowing the specific causes and implications of each jaundice type is crucial for doctors to identify them correctly and provide adequate care.
Pre-Hepatic Jaundice
Pre-Hepatic Jaundice is usually caused by excessive breakdown of red blood cells. This leads to high bilirubin levels. This type occurs before bilirubin reaches the liver. Conditions such as malaria, sickle cell anemia, or hemolytic anemia are common causes of this type.
Hepatic Jaundice
Hepatic Jaundice happens when your liver is damaged or scarred. Due to the damage, the liver is unable to process bilirubin properly. Diseases like hepatitis, cirrhosis, alcoholic liver disease, or genetic liver disorders can cause this type of jaundice.
Post-Hepatic (Obstructive) Jaundice
Post-Hepatic or Obstructive Jaundice develops when bile ducts are blocked. This blockage prevents bilirubin from being released from the liver. The gallstones, pancreatic or bile duct tumors, and strictures in the bile ducts are common reasons for these blockages. This leads to dark urine, pale stools, and severe itching.
Neonatal Jaundice
Neonatal jaundice, also known as infant jaundice. We commonly see Jaundice in newborn babies. The newborn baby's livers are not fully developed to process bilirubin efficiently. It appears within a few days of birth and resolves on its own or with simple treatments, such as phototherapy.
What are the Jaundice Symptoms?
Symptoms of Jaundice range from mild to severe, depending on the cause. The iconic noticeable sign of jaundice is the yellowing of the skin and eyes (jaundice eyes).
- Starting Symptoms of Jaundice: The yellowing of the whites of the eyes and skin is usually the first sign, often followed by dark-colored urine, pale stools, mild fatigue, and occasional itching.
- Symptoms in Adults: Noticeable yellowing of the skin and eyes, dark urine, pale or clay-colored stools, persistent itchiness, fatigue, abdominal pain, nausea, and sometimes fever depending on the cause of jaundice.
- Symptoms in Newborns: Yellow skin appearing 2–4 days after birth, starting on the face and moving down the body, poor feeding, excessive sleepiness, irritability, and in severe cases, high-pitched crying or difficulty waking up.
Other Noticeable Signs of Jaundice
- Fever
- Stomach pain
- Chills
- Itchy skin
- Weight loss
- Confusion
- Bloody vomit
If you observe symptoms of jaundice, it’s best to consult our Gastroenterologist for early evaluation and proper care.
Get a second opinion from trusted experts and makeconfident, informed decisions.
Get Second OpinionWhat are the Jaundice Causes?
Primarily, jaundice is caused by liver failure in bilirubin processing. Bilirubin is a waste product formed when red blood cells die in the blood.
- There are three main causes of jaundice. Pre-hepatic jaundice happens when there is excessive breakdown of red blood cells, producing more bilirubin than the liver can handle.
- Hepatic (intrahepatic) jaundice happens when liver cells can’t process or conjugate bilirubin properly. Common causes include viral hepatitis (A, B, C), alcoholic liver disease, cirrhosis, non‑alcoholic fatty liver disease, drug‑induced liver injury, autoimmune hepatitis, and genetic disorders like Gilbert’s, Crigler–Najjar, Rotor or Dubin-Johnson syndromes.
- Post‑hepatic (obstructive) jaundice results from a blockage of bile ducts after bilirubin is conjugated. Common causes include gallstones in the common bile duct (choledocholithiasis), biliary strictures, cholangiocarcinoma, pancreatic head tumors, biliary atresia in infants, cholangitis, parasitic infections (liver flukes), and benign or malignant ductal obstruction.
Other Medical Conditions: Jaundice Reasons
- Alcoholic Hepatitis
- Liver Cirrhosis
- Drug-Induced Liver Injury
- Sepsis
- Pancreatic Disorders
- Hemolytic Transfusion Reactions
- Parasitic Infections
- Autoimmune Liver Diseases
Risk Factors of Jaundice
There are several factors that can increase the risk of developing jaundice, by causing liver problems, increasing red blood cell breakdown, or blocking bile flow.
- Excessive Alcohol Consumption
- Viral Hepatitis Infections
- Unprotected Blood Transfusions or Needle Use
- Newborn Factors
- Gallstones or Bile Duct Diseases
- Autoimmune or Genetic Liver Disorders
- Certain Medications or Toxins
- Metabolic Disorders
- Exposure to Parasites or Contaminated Water
How is Jaundice Diagnosed?
The Jaundice diagnosis process begins when doctors ask about symptoms such as yellowing of the skin or eyes, dark urine, pale stools, fatigue, itching, abdominal pain, fever, or recent infections. They also inquire about medication use, alcohol use, travel, and family history of liver disease or hemolytic disorders.
Jaundice diagnosis relies on several steps:
- First, a bilirubin blood test measures total bilirubin and its direct/indirect fractions. Levels above about 2–3 mg/dL (34–51 μmol/L) indicate jaundice, the normal total is below 1.0 mg/dL (17 μmol/L).
- A liver function panel (LFT) includes enzymes such as AST, ALT, ALP, and GGT, plus albumin and total protein, helping distinguish hepatic versus obstructive causes.
- A complete blood count (CBC) helps to detect anaemia or hemolysis. A urine urobilinogen test shows pre‑hepatic or intrahepatic causes when elevated, and the absence of bilirubinuria suggests unconjugated bilirubin.
- If obstruction is suspected, abdominal ultrasound (and sometimes CT or MRCP) is used to detect gallstones, bile duct blockages or tumors.
- A liver biopsy may be performed to assess liver tissue directly for underlying disease in unclear cases. A small piece of liver is taken by inserting a needle for effective tests to detect liver issues.
- These tests together help determine whether jaundice is pre‑hepatic (hemolytic), hepatic (liver-related) or post‑hepatic (obstructive) by analysing patterns in bilirubin and enzyme levels, urine findings, blood counts, and imaging results.
What is the Jaundice Treatment?
Jaundice has no direct cure because it is not a disease. It is a symptom of various medical conditions. The healthcare provider designs the treatment plan for jaundice based on its causes. Medical care focuses on diagnosing and treating the underlying cause, whether it’s viral hepatitis, anemia, gallstone obstruction, or liver damage.
- If you have viral hepatitis, you may be prescribed antiviral medications to reduce inflammation and boost liver recovery. If jaundice comes from a bile duct blockage, such as gallstones or tumors. The procedures, such as ERCP or surgery, are performed to remove the obstruction, can restore bile flow and resolve jaundice.
- For symptom relief, especially itching (pruritus), doctors may prescribe cholestyramine or colestipol, which help clear bile acids from the body.
- Corrective treatments, like blood transfusions, iron supplements, immunosuppressants, or IVIG, are used to manage red blood cell breakdown and reduce bilirubin production in cases of hemolytic anemia.
- In newborns, high bilirubin levels are addressed through phototherapy (blue-light treatment) to convert bilirubin into a form that is easier to excrete, and in severe cases, exchange transfusion may be necessary. But this phototherapy is not effective in treating jaundice in adults.
- Ursodeoxycholic acid (UDCA) is used in rare cases for cholestatic liver conditions like sclerosing cholangitis or biliary cirrhosis to improve bile flow and reduce bilirubin levels.
When to see a Jaundice Doctor?
Always remember that jaundice in adults and newborns requires a doctor’s consultation. You can't manage the symptoms by your own at home, sometimes it will give bad results.
You should see a doctor immediately if you notice a yellow colour of the skin or eyes.
Medical attention is especially important if you notice the following signs.
- dark urine
- pale stools
- severe abdominal pain
- persistent vomiting
- unexplained fatigue
- Fever
- sudden weight loss
Newborns with jaundice are examined by a doctor as soon as symptoms appear because untreated high bilirubin levels can be harmful. Adults who already have liver disease, hepatitis, gallstones, or heavy alcohol use should take proper medical care.
Your health is everything - prioritize your well-being today.
What is the Recovery Process After Jaundice Treatment?
Recovery from jaundice depends on the underlying cause and the individual's overall health. Most infants recover within weeks, adults may require a longer time.
Recovery Steps
- Regular liver function monitoring
- Proper medication usage by the doctor's advice
- Follow-up visits and imaging
- Adequate hydration and nutrition
- Managing related conditions like hepatitis or gallstones
- Lifestyle changes under medical supervision
What Precautions Can Help Prevent Jaundice?
Prevention of jaundice starts with focusing on the cause of the jaundice. High-risk individuals should take extra care through regular monitoring and avoiding triggers to liver health through healthy lifestyle choices and early detection of liver conditions.
- Hepatitis B Vaccination
- Hepatitis B immunoglobulin and antivirals, safe injection practices for pregnant women
- Safe Injection and Blood Practices (Using auto-disable syringes)
- Safe Drinking Water and Food Hygiene
- Public Awareness and Screening
- Stop alcohol
- Maintain a healthy body weight
What are the Jaundice Complications if Left Untreated?
- Jaundice affects 50% of full-term babies and 80% of preterm babies, with severe untreated cases leading to 30% death rate or long-term brain damage such as cerebral palsy, deafness, or seizures.
- Jaundice in pregnancy occurs in 3–5% of cases, with maternal death rates up to 40% and perinatal deaths up to 37–40% in severe conditions.
- In critically ill adults, high bilirubin levels increase the risk of sepsis, organ failure, and death, and in rare cases can cause neurological damage (kernicterus).
- Long-term complications can include liver failure, kidney failure, and permanent neurological disorders if not treated on time.
Jaundice Food Diet
What we eat decides our health. During the jaundice treatment, there are many food restrictions to decide what to eat and what to avoid.
Foods to Eat During Jaundice
- Coconut water
- Herbal teas (chamomile, ginger, peppermint)
- Spinach
- Kale
- Carrots
- Beets
- Papaya
- Oranges
- Lemons
- Sweet potatoes
- Berries (strawberries, blueberries, raspberries)
- Oats
- Brown rice
- Quinoa
- Whole wheat bread
- Egg whites
- Moong dal
- Lentils
- Beans (kidney beans, black beans, chickpeas)
- Tofu
- Skinless chicken
- Fish (steamed or boiled)
- Avocado
- Almonds
- Walnuts
- Flaxseeds
- Sugarcane juice
Foods to Avoid During Jaundice
- Alcohol
- Coffee
- Strong tea
- Fried snacks
- Chips
- Burgers
- Oily curries
- Processed meats (sausages, bacon, hot dogs)
- Ready-to-eat packaged meals
- Instant noodles
- Pastries
- White bread
- Soft drinks
- Sweetened juices
- Beef
- Lamb
- Pork
- Butter
- Whole milk
- Cream
- Cheese
- Pickles
- Canned soups
- Salty snacks
- Spicy gravies
- Undercooked fish or shellfish
Our Experience Treating Jaundice
At Medicover Hospitals, we provide dedicated care for jaundice in both adults and newborns. Our team of doctors and nurses works together to ensure accurate diagnosis and treatment plans tailored to each patient’s needs.
We offer advanced diagnostic services and complete post-treatment support, focusing on patient safety and well-being at every stage. With a caring approach and modern medical facilities, Medicover aims to help patients recover and maintain good liver health.