What is Vaginal Prolapse?
Vaginal prolapse occurs when the muscles, ligaments, and connective tissues that support the vagina weaken or stretch. As a result, the vaginal walls or nearby pelvic organs (such as the bladder, rectum, or uterus) shift downward into or outside the vaginal canal.
This condition is more common in women who have:
- Experienced childbirth (especially multiple or difficult deliveries).
- Reached menopause, where estrogen decline weakens tissue support.
- Undergone pelvic surgery such as hysterectomy.
- Experienced chronic pelvic strain, such as from constipation, obesity, or heavy lifting.
What is Vaginal Vault Prolapse?
The vaginal vault refers to the upper portion of the vaginal canal.
- Vaginal vault prolapse happens when this top part loses support and collapses downward, sometimes protruding outside the vaginal opening.
- It often occurs after a hysterectomy, when the uterus is removed and the vaginal apex is left unsupported.
- Symptoms include pelvic pressure, difficulty with urination or bowel movements, discomfort during intercourse, and a visible bulge at the vaginal opening.
Surgical options, such as vaginal vault prolapse repair, are often recommended to restore normal pelvic anatomy and function.
Types of Vaginal Prolapse
Vaginal prolapse can affect different parts of the pelvic floor depending on which organ loses its support. The main types include:
Cystocele (Anterior Vaginal Prolapse):
- Occurs when the bladder drops from its normal position and bulges into the front wall of the vagina.
- Common symptoms: frequent urination, incomplete bladder emptying, or urinary leakage.
Rectocele (Posterior Vaginal Prolapse):
- Happens when the rectum pushes into the back wall of the vagina.
- Symptoms may include constipation, difficulty with bowel movements, or the need to press on the vaginal wall to pass stool.
Enterocele:
- Involves the small intestine protruding into the upper vaginal wall.
- May cause a sense of heaviness, pelvic pressure, or a bulge sensation.
Uterine Prolapse:
- The uterus descends into the vaginal canal, sometimes extending outside the vaginal opening.
- Often associated with childbirth, menopause, or weakened pelvic ligaments.
Vaginal Vault Prolapse:
- Occurs when the top of the vaginal canal (vault) loses its support and sags downward.
- Most common in women who have undergone a hysterectomy.
1 to 2 Hours
Surgery Duration
General/Local Anesthesia
Anesthesia Used
4-6 Weeks
Full Recovery Timeline
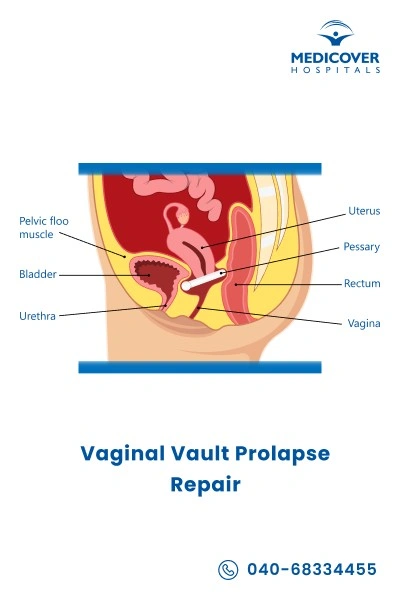
What are the indications for Vaginal Vault Prolapse surgery?
Indications for Vaginal Vault Prolapse repair surgery arise when weakened pelvic support tissues cause the upper portion of the vagina to descend, leading to significant symptoms. A doctor may recommend surgery if you experience:
- Pelvic Heaviness or Pressure: A sensation of fullness or pressure in the pelvic area. This can feel like a constant weight or discomfort in the lower abdomen and pelvic region.
- Vaginal Bulging or Protrusion: Tissue may bulge or protrude through the vaginal opening. This visible bulge can be more noticeable during physical activities or prolonged standing.
- Urinary Problems: Difficulty emptying the bladder or urinary incontinence. You may experience a frequent urge to urinate or leaking, especially when coughing or sneezing.
- Bowel Issues: Difficulty with bowel movements or constipation. Some women may feel the need to strain excessively or feel incomplete bowel emptying.
- Vaginal Discomfort or Pain: Pain during sexual intercourse or general vaginal discomfort. This discomfort can result in a reduced quality of life and may be triggered by physical activity.
- Pelvic Organ Prolapse: Symptoms of a dropped uterus, bladder, or other pelvic organs. This occurs when organs like the bladder or uterus descend lower than their normal position, causing further pressure.
- Back or Pelvic Pain: Discomfort or pain in the back or pelvic region. This may worsen after standing for long periods or after physical exertion.
- Vaginal Lump or Bulge: A noticeable bulge or lump in the vagina. This can be felt inside the vagina and might be visible when looking in a mirror, especially when standing.
These symptoms can disrupt daily activities and vary in severity, often worsening with specific movements or activities.
When would a doctor recommend Vaginal Vault Prolapse repair?
A doctor typically recommends Vaginal Vault Prolapse surgery in situations such as:
- When symptoms significantly interfere with normal daily activities.
- If conservative treatments like pessary use or pelvic floor exercises have failed.
- In cases of severe or worsening prolapse, where the vaginal walls or organs visibly protrude.
- When prolapse causes urinary retention, recurrent UTIs, or incontinence.
- If bowel emptying is difficult or painful due to rectal involvement.
- When a woman wishes to restore both functional and aesthetic vaginal support for better quality of life.
Why is Vaginal Vault Prolapse surgery done?
The primary reasons for performing this surgery include:
- To restore normal vaginal anatomy and support of the pelvic organs.
- To relieve symptoms of bulging, pressure, or pelvic heaviness.
- To improve urinary and bowel function, preventing retention, leakage, and constipation.
- To reduce or eliminate pain and sexual dysfunction.
- To prevent the progression of prolapse into more severe stages.
- To improve quality of life by allowing patients to return to daily activities comfortably.
Who is Vaginal Vault Prolapse surgery for?
This surgery is most suitable for:
- Women who have had a hysterectomy and developed vaginal vault prolapse afterward.
- Women with moderate to severe prolapse symptoms that limit mobility, comfort, or daily functioning.
- Patients who have not benefited from non-surgical options like pessaries or pelvic therapy.
- Women who experience sexual dysfunction, urinary incontinence, or bowel issues due to prolapse.
- Those who wish to restore pelvic health and improve both physical and emotional well-being.
How should I prepare before the Vaginal Vault Prolapse procedure?
Preparing properly before Vaginal Vault Prolapse repair surgery ensures safety and smooth recovery. Steps include:
- Consultation and Evaluation: Meet with a gynecologist or urogynecologist who specializes in pelvic floor disorders. They will review your symptoms, medical history, and perform a physical and pelvic exam.
- Medical History & Medications: Share all health details including current medications, supplements, and allergies. Some blood thinners, diabetes medicines, or hormonal therapies may need adjustment.
- Lifestyle Adjustments: Maintain a healthy weight, eat a balanced diet, stay hydrated, and quit smoking to improve healing.
- Pelvic Floor Exercises: Your doctor may advise Kegel exercises before and after surgery to strengthen pelvic muscles and improve long-term outcomes.
- Support at Home: Arrange for help at home during the first days after surgery and prepare a recovery-friendly space.
- Mental Preparation: Understand the benefits and risks, and address any questions with your surgeon for peace of mind before the procedure.
What tests are done before Vaginal Vault Prolapse surgery?
Before vaginal vault prolapse repair, diagnostic tests help ensure you are fit for surgery and guide the surgical approach. These may include:
- Pelvic Examination: To assess the severity of prolapse and evaluate the vaginal walls, bladder, rectum, and uterus (if present).
- Imaging Tests: Pelvic ultrasound, MRI, or dynamic pelvic floor imaging to visualize prolapse extent and organ involvement.
- Urodynamic Testing: For women with urinary symptoms, to check bladder function and incontinence.
- Blood Tests: To evaluate overall health, detect anemia, clotting issues, or infections.
- ECG or Chest X-ray: Recommended for older patients or those with heart or lung problems, to ensure safe anesthesia.
Should I stop eating, drinking, or taking medicines before Vaginal Vault Prolapse surgery?
Yes, following pre-surgery instructions is crucial for safety:
- Fasting: Typically, you must stop eating and drinking 6-8 hours before surgery (especially if general anesthesia is used). Small sips of water may be allowed for essential medications, but only if approved by your doctor.
- Medications:
- Stop blood thinners (like aspirin, warfarin, or clopidogrel) as directed to reduce bleeding risks.
- Diabetes medications or insulin may be adjusted the night before or morning of surgery.
- Hormone replacement therapy or vaginal estrogen creams may need temporary discontinuation.
- Always follow your surgeon's specific advice, never stop medicines on your own.
- Smoking & Alcohol: Stop smoking at least a few weeks before surgery and avoid alcohol for 24-48 hours beforehand to lower anesthesia risks.
What happens before Vaginal Vault Prolapse surgery?
On the day of the procedure, you can expect:
- Hospital Admission: Arrive a few hours before surgery for final checks.
- Preoperative Assessment: Nurses will record vitals, check lab results, and review your health status.
- Anesthesia Consultation: The anesthesiologist will explain the anesthesia plan (usually general or regional) and discuss safety measures.
- Marking and Consent: Your surgeon will review the procedure, answer final questions, and ask you to sign consent forms.
- Preparation: You may need to change into a surgical gown, remove jewelry, contact lenses, or dentures, and empty your bladder.
- IV Line Placement: For fluids, antibiotics, and anesthesia medications.
After these steps, you'll be taken to the operating room to begin the Vaginal Vault Prolapse repair procedure.
What Happens During Vaginal Vault Prolapse Repair?
Vaginal vault prolapse repair is a surgical procedure aimed at repositioning the vaginal vault and restoring pelvic organ support.
- Anesthesia: The patient is given general or regional anesthesia to ensure they are pain-free during the procedure.
- Positioning: The patient is positioned on their back with legs elevated to access the vaginal area.
- Incision: Small incisions are made in the vaginal wall or abdomen, depending on the approach.
- Repair: The surgeon repositions the vaginal vault and repairs weakened tissues or ligaments, sometimes using mesh for added support.
- Closure: The incisions are closed with sutures, and any mesh used is secured.
- Recovery: After surgery, the patient is monitored in recovery and given instructions for post-op care, including pelvic rest and follow-up visits.
The goal is to restore pelvic organ support, improve comfort, and prevent recurrence of prolapse.
Who Performs Vaginal Vault Prolapse?
Gynecologists or urogynecologists, who specialize in female pelvic medicine and reconstructive surgery, are the healthcare professionals who perform vaginal vault prolapse repair.
If you're experiencing symptoms of vaginal vault prolapse, such as discomfort or pressure in the pelvic area, urinary issues, or changes in bowel habits, or if you have concerns about uterus falling out, it's advisable to consult with a healthcare provider.
Your primary care physician or gynecologist can provide an initial evaluation and recommend a referral to a specialist if needed
Recovery After Vaginal Vault Prolapse
The recovery phase following vaginal vault prolapse repair is crucial for optimal healing and a successful outcome:
- Hospital Stay: Depending on the surgical approach and the patient's overall health, the hospital stay can range from a few hours to a couple of days.
- Pain Management: You might experience discomfort and pain after the surgery. Your healthcare team will prescribe pain medication to manage these symptoms.
- Restricted Activities: You'll be advised to avoid heavy lifting, strenuous exercise, and sexual activity for a specific period following the surgery to allow the repaired tissues to heal properly.
- Vaginal Rest: Your healthcare provider may recommend refraining from inserting anything into the vagina for a certain period to prevent strain on the healing tissues.
- Follow-Up Appointments: Attend all follow-up appointments as scheduled by your healthcare provider. These appointments are crucial for monitoring your healing progress and addressing any concerns.
Lifestyle Changes After Vaginal Vault Prolapse
After being diagnosed with vaginal vault prolapse, certain lifestyle changes can help manage symptoms, improve pelvic health, and prevent further complications.
- Pelvic Floor Exercises (Kegels): Strengthening the pelvic floor muscles can help support the pelvic organs and reduce prolapse symptoms. Regular Kegel exercises are often recommended.
- Maintain a Healthy Weight: Excess weight can increase pressure on the pelvic region, worsening prolapse symptoms. Maintaining a healthy weight through balanced diet and regular exercise can alleviate strain on the pelvic floor.
- Avoid Heavy Lifting: Lifting heavy objects can put additional strain on the pelvic region. If lifting is necessary, ensure proper technique and consider using support garments.
- Manage Constipation: Straining during bowel movements can worsen prolapse. A fiber-rich diet, adequate water intake, and regular physical activity can help prevent constipation.
- Stay Active, But Avoid Strenuous Exercise: While regular physical activity is important, avoid exercises that put excessive strain on the pelvic area, such as heavy weight lifting or high-impact aerobics.
- Use Support Garments: A pelvic support belt or pessary can help relieve pressure on the pelvic organs and provide added support, particularly during physical activities.
- Elevate Legs and Rest: If symptoms worsen after prolonged standing or walking, elevate the legs and take frequent rest breaks to reduce pressure on the pelvic area.
- Posture and Body Mechanics: Maintain good posture while sitting or standing to avoid added pressure on the pelvic floor. Proper posture can help improve comfort and reduce strain.
- Avoid Smoking: Smoking can weaken connective tissues and slow down healing, potentially exacerbating prolapse symptoms. Quitting smoking is beneficial for overall pelvic health.
These lifestyle changes can help manage the condition and may improve quality of life. Always consult with a healthcare provider for personalized recommendations and treatment options.
Benefits of Vaginal Vault Prolapse Repair Procedure
Vaginal vault prolapse repair offers several important advantages for women experiencing pelvic floor dysfunction:
- Restores Pelvic Support: Strengthens and repositions the vaginal walls and surrounding organs, preventing further descent.
- Improves Quality of Life: Reduces symptoms such as pelvic heaviness, vaginal bulging, and discomfort.
- Enhances Bladder Function: Improves or corrects urinary problems, including leakage or difficulty emptying the bladder.
- Better Bowel Function: Alleviates constipation and bowel straining caused by organ pressure.
- Improves Sexual Function: Restores vaginal anatomy, reducing pain or discomfort during intercourse.
- Prevents Further Complications: Helps avoid worsening prolapse or damage to other pelvic organs.
- Boosts Confidence and Comfort: Allows patients to resume daily activities without embarrassment or restriction.
Risks and Complications of Vaginal Vault Prolapse Surgery
Like any surgery, vaginal vault prolapse repair has potential risks and complications:
- Infection: At the incision site or in deeper pelvic tissues.
- Bleeding: Mild bleeding is common; severe bleeding is rare.
- Urinary Issues: Temporary or persistent urinary incontinence, urgency, or difficulty urinating.
- Bowel Dysfunction: Constipation, straining, or discomfort with bowel movements.
- Nerve Injury: Rare but may cause altered sensation or pelvic pain.
- Scarring or Adhesions: Can affect pelvic mobility or cause discomfort.
- Recurrence of Prolapse: In some cases, the prolapse may return if underlying causes persist.
- Blood Clots (DVT/PE): Rare but possible, involving clots in the legs or lungs.
- Pain or Discomfort: Persistent pelvic or vaginal pain in a small number of cases.
Side Effects of Vaginal Vault Prolapse Repair
Temporary side effects may occur during the recovery phase:
- Swelling and Bruising: Around the surgical site or pelvic area.
- Mild Pain or Soreness: Especially in the first few weeks after surgery.
- Vaginal Discharge or Spotting: Light bleeding or discharge is common initially.
- Temporary Urinary or Bowel Changes: Difficulty emptying bladder or constipation for a short period.
- Tiredness and Fatigue: Common after anesthesia and during the body's healing process.
Most side effects improve within a few weeks as healing progresses.
What is the cost of vaginal vault prolapse repair surgery in India?
The vaginal vault prolapse repair surgery cost in India usually ranges from Rs. 90,000 to Rs. 1,60,000, depending on the procedure type, hospital, and city. On average, the cost is around Rs. 1,25,000.
In some cities like Kolkata, a laparoscopic vault prolapse repair (sacrocolpopexy) costs between Rs. 1,00,000 and Rs. 1,50,000, while in Bangalore, procedures such as colpopexy may range from Rs. 90,000 to Rs. 1,30,000, and sacrospinous fixation from Rs. 1,30,000 to Rs. 1,60,000.
The overall price depends on the surgical technique used, the hospital facilities, the surgeon's expertise, and whether additional services like tests, anesthesia, and post-surgery care are included.





















































































