What Is a Laparoscopic Supracervical Hysterectomy?
Laparoscopic Supracervical Hysterectomy (LSH) is a minimally invasive surgical procedure designed to remove the uterus while leaving the cervix intact. This approach is often chosen to treat a variety of uterine conditions, such as heavy menstrual bleeding, fibroids, or abnormal uterine growths.
Because it is performed laparoscopically, LSH typically results in:
- Smaller incisions and less scarring
- Reduced postoperative pain
- Shorter hospital stays and quicker recovery
- Lower risk of complications compared to traditional open surgery
Preserving the cervix may also help maintain pelvic support and sexual function, offering patients a modern, patient-centered approach to gynecological surgery.
How Does Laparoscopic Supracervical Hysterectomy Work?
During LSH, small incisions are made in the abdomen to insert a laparoscope (a thin, lighted camera) and specialized surgical instruments.
The uterus is carefully detached from surrounding structures, leaving the cervix in place, and then removed through the small incisions. This minimally invasive approach allows for quicker healing and smaller scars compared with traditional hysterectomy.
1 to 3 Hours
Surgery Duration
General Anesthesia
Anesthesia Used
4-6 Weeks
Full Recovery Timeline
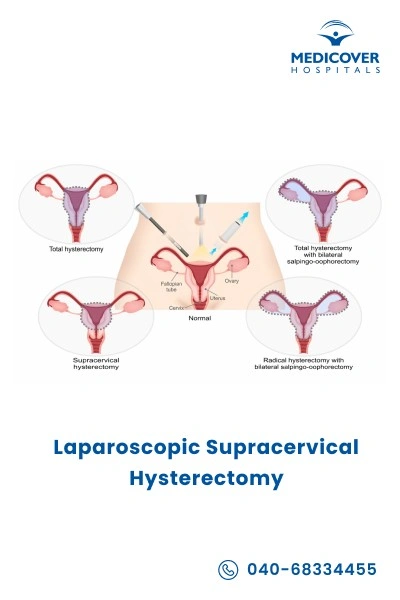
Indications of Laparoscopic Supracervical Hysterectomy (LSH)
Laparoscopic Supracervical Hysterectomy (LSH) is a surgical procedure that is considered under specific indications, aiming to address various gynecological conditions while preserving the cervix.
Common indications for LSH include:
- Uterine Fibroids: LSH may be recommended for individuals with uterine fibroids that cause symptoms such as heavy menstrual bleeding, pelvic pain, or pressure.
- Abnormal Uterine Bleeding: LSH can be considered for those experiencing irregular or excessive menstrual bleeding that hasn't responded to other treatments.
- Adenomyosis: LSH may be an acceptable alternative when adenomyosis, a disorder in which the uterine lining develops into the muscle wall of the uterus, causes considerable pain or discomfort.
- Endometriosis: Endometriosis, a disorder in which tissue comparable to the uterine lining grows outside the uterus, producing pain and other symptoms, can be treated with LSH.
- Pelvic Organ Prolapse: In cases of pelvic organ prolapse, where the uterus falls into the vaginal canal, LSH may be considered as part of the treatment.
- Chronic Pelvic Pain: LSH can be explored when chronic pelvic pain is attributed to gynecological conditions that warrant hysterectomy.
- Desire to Preserve Cervix: Some women opt for LSH to retain the cervix, potentially preserving pelvic functions and maintaining a more natural anatomy.
- Patient Preference: In cases where patients express a preference for a less invasive approach or want to maintain the cervix for personal or cultural reasons, LSH may be considered.
It's important to note that the decision to undergo Laparoscopic Supracervical Hysterectomy should be made in consultation with a qualified gynecologist.
The gynecologist will evaluate the individual's medical history, symptoms, and overall health to determine whether LSH is the most suitable treatment option based on their specific circumstances.
When would a doctor recommend Laparoscopic Supracervical Hysterectomy?
Doctors may suggest LSH when:
- Less invasive treatments, like medications or hormone therapy, have failed
- The patient prefers to preserve the cervix for pelvic support or sexual function
- There is a need for a minimally invasive approach to reduce recovery time and surgical complications
- Patient-specific factors, including personal or cultural preferences, make LSH the most suitable option
How should I prepare before Laparoscopic Supracervical Hysterectomy (LSH)?
Preparing for Laparoscopic Supracervical Hysterectomy (LSH) is essential to ensure a safe procedure and smooth recovery. Here's what you should do:
- Consult your gynecologist to review your medical history, discuss symptoms, and confirm the need for LSH.
- Medical evaluations may include blood tests, imaging such as ultrasound or MRI, and a physical exam to assess overall health.
- Medication review is important. Inform your healthcare provider about all medications, supplements, and herbs you are taking. You may need to adjust or temporarily stop certain medications.
- Nutrition should be optimized according to your doctor's recommendations to support healing.
- Smoking cessation is advised, as smoking can impair recovery and increase complication risk.
- Hygiene and skin care should follow your surgeon's instructions to minimize infection risk.
- Mental preparation helps manage anxiety and understand the procedure, recovery process, and expected outcomes.
What tests are done before Laparoscopic Supracervical Hysterectomy (LSH)?
Before the procedure, your healthcare provider may perform several assessments to ensure you are fit for surgery:
- Blood tests to check overall health, hemoglobin, and clotting factors.
- Imaging studies such as ultrasound or MRI to evaluate the uterus and surrounding structures.
- Physical examination to assess your general health and readiness for surgery.
- Medication and allergy review to ensure safe use of anesthesia and other perioperative medications.
These tests help the surgical team minimize risks and plan the procedure effectively.
Should I stop eating, drinking, or taking medicines before Laparoscopic Supracervical Hysterectomy (LSH)?
Yes, following your surgeon's instructions is important:
- Fasting guidelines will specify when to stop eating and drinking before surgery to reduce anesthesia risks.
- Medication adjustments may be required. Blood-thinning medications or other drugs may need to be temporarily stopped or modified.
- Follow your doctor's instructions closely to ensure a safe procedure and reduce the risk of complications.
Steps Involved in Laparoscopic Supracervical Hysterectomy (LSH)
Laparoscopic Supracervical Hysterectomy (LSH) is a meticulous surgical procedure that involves the removal of the uterus while preserving the cervix. This minimally invasive technique offers several benefits, including reduced pain, shorter recovery times, and potential retention of certain pelvic functions.
The following steps outline the process of performing LSH:
- Anesthesia: The patient is placed under general anesthesia to ensure they are comfortable and unconscious throughout the procedure.
- Incision Placement: Several small incisions are created, generally around the belly button and lower abdomen, to allow laparoscopic tools to be inserted.
- Creation of Pneumoperitoneum: Carbon dioxide gas is supplied to generate space in the abdominal cavity, providing greater vision of the surgical area.
- Insertion of Laparoscope: A laparoscope (a thin tube with a camera) is inserted through one of the incisions. The camera's images are projected onto a monitor, providing the surgeon with a clear view of the surgical site.
- Dissection of Uterine Attachments: The surgeon uses specialized instruments inserted through the other incisions to carefully detach the uterus from its surrounding structures, such as ligaments and blood vessels.
- Ligation and Removal: Once the uterus is freed from its attachments, the blood vessels supplying it are ligated (tied off) to prevent bleeding. The uterus is then removed through one of the incisions.
- Cervical Management: The cervix is left intact. If desired, the cervix can be anchored to the top of the vaginal canal to prevent potential descent or prolapse in the future.
- Closure: After ensuring all bleeding is under control, the surgeon removes the instruments and releases the carbon dioxide gas.
- Dressings and Recovery: Sterile dressings are applied to the incisions. The patient is carefully monitored in the recovery area as they wake up from anesthesia.
- Post-Operative Care: Following the procedure, patients are given pain medication and post-operative instructions for wound care, activity levels, and recovery.
- Follow-Up: Scheduled follow-up appointments allow the surgeon to assess healing, address any concerns, and provide guidance for the recovery process.
Each patient's experience may vary, and the specifics of the procedure can be influenced by the surgeon's approach and the patient's unique anatomy.
Who will perform the Laparoscopic Supracervical Hysterectomy (LSH)?
Experienced gynecologists or gynecological surgeons perform Laparoscopic Supracervical Hysterectomy (LSH) with expertise in minimally invasive techniques.
Key professionals involved include:
- Gynecologist: Assesses symptoms and determines if LSH is appropriate.
- Gynecological Surgeon: Performs the surgery using laparoscopic tools.
- Minimally Invasive Surgeon: Specialises in small-incision procedures.
- Surgical Team: Includes anesthesiologists and nurses who assist during surgery.
- Medical Centre: Procedure is done in a well-equipped hospital or surgical center.
What should I expect immediately after Laparoscopic Supracervical Hysterectomy (LSH)?
After LSH, most patients are monitored in the recovery area until the effects of anesthesia wear off. You may experience:
- Mild discomfort or pain, which can be managed with prescribed medications.
- Drowsiness or fatigue from anesthesia.
- Small amounts of vaginal bleeding or spotting.
- Slight abdominal bloating or cramping, which is normal after laparoscopic surgery.
Your healthcare team will provide guidance on wound care, pain management, and activity limitations before you go home.
When can I return to normal activities after Laparoscopic Supracervical Hysterectomy (LSH)?
Recovery is gradual, and your return to normal activities depends on your overall health and healing:
- Rest and gradual movement: Start with light activity and short walks to improve circulation.
- Driving: Avoid driving until your doctor clears you, usually within 1-2 weeks.
- Work: Light work can often resume in a few weeks; avoid strenuous activity and heavy lifting for at least 4-6 weeks.
- Follow-up visits: Attend all scheduled appointments to monitor healing and address any concerns.
By gradually resuming activities and following your surgeon's instructions, you can support a safe and effective recovery.
Are lifestyle changes required after recovery from Laparoscopic Supracervical Hysterectomy (LSH)?
Yes, adopting healthy lifestyle habits can enhance healing and overall well-being:
- Balanced diet: Include fruits, vegetables, lean proteins, and whole grains to support tissue repair.
- Hydration: Drink plenty of water daily to aid recovery.
- Gentle exercise: Walking or light activity as advised helps maintain strength and circulation.
- Rest and sleep: Prioritize adequate rest and avoid heavy lifting during recovery.
- Quit smoking: Smoking can delay healing and increase complication risks.
- Stress management: Practices like meditation, yoga, or deep breathing can improve emotional well-being.
- Medication adherence: Take prescribed medications as directed and follow up with appointments.
- Intimacy and emotional health: Resume sexual activity only when cleared by your doctor and seek emotional support if needed.
Following these lifestyle adjustments helps optimize your recovery and supports long-term health after LSH.
What are the benefits of having a Laparoscopic Supracervical Hysterectomy (LSH)?
Laparoscopic Supracervical Hysterectomy (LSH) offers several advantages for individuals with uterine conditions:
- Minimally invasive approach: Smaller incisions lead to less pain, quicker healing, and a shorter hospital stay.
- Preservation of the cervix: Maintaining the cervix may help retain pelvic support and sexual function.
- Reduced recovery time: Patients often resume normal activities sooner compared to traditional hysterectomy.
- Lower risk of complications: Minimally invasive techniques reduce blood loss, scarring, and risk of infection.
- Improved quality of life: Relief from symptoms such as heavy menstrual bleeding, pelvic pain, or pressure improves daily functioning.
What are the risks and complications of Laparoscopic Supracervical Hysterectomy (LSH)?
Although LSH is generally safe, potential risks and complications can include:
- Infection: At the incision sites or internally in the pelvic area.
- Bleeding: Severe bleeding may require additional procedures or blood transfusions.
- Injury to surrounding organs: Possible damage to the bladder, intestines, or ureters.
- Blood clots: Risk of deep vein thrombosis (DVT) or pulmonary embolism (PE), particularly due to immobility.
- Adverse reaction to anesthesia: Including nausea, vomiting, or allergic reactions.
- Scarring and adhesions: Internal scarring can cause pelvic pain or bowel obstruction.
- Urinary retention: Temporary difficulty urinating, sometimes requiring catheterization.
- Pelvic organ prolapse: Rarely, the preserved cervix may contribute to prolapse.
- Ovarian damage: Accidental damage or removal of ovaries can affect hormonal balance.
What are the side effects after Laparoscopic Supracervical Hysterectomy (LSH)?
Common side effects after LSH are usually mild and temporary:
- Abdominal discomfort or cramping near the incision sites.
- Mild vaginal bleeding or spotting for a short period.
- Fatigue or drowsiness as your body recovers from surgery and anesthesia.
- Bloating or gas due to air introduced during laparoscopy.
- Emotional changes such as mood swings, anxiety, or stress related to surgery and recovery.
By understanding these potential risks, complications, and side effects, patients can take proactive steps to ensure a safe recovery and optimize the benefits of LSH.
What is the typical cost of Laparoscopic Supracervical Hysterectomy (LSH) surgery in India?
The cost of Laparoscopic Supracervical Hysterectomy (LSH) in India typically ranges from Rs. 75,000 to Rs. 2,50,000. Prices can vary depending on the hospital, surgeon, patient condition, and other factors.
Factors Influencing LSH Cost:
- Hospital Charges: Pricing differs based on the hospital's facilities and reputation.
- Surgeon's Experience: Highly experienced surgeons may charge more.
- Patient's Condition: Complexity of the underlying gynecological issue affects cost.
- Inclusions: Some quotes include pre-surgery tests, lab work, and post-operative care; others do not.
- Geographic Location: Costs vary between cities and regions.






















































































