What is Diagnostic Hysteroscopy?
Diagnostic hysteroscopy is a minimally invasive procedure that allows doctors to look inside the uterus using a thin, lighted tube called a hysteroscope. This helps in identifying problems such as uterine fibroids, polyps, adhesions, or abnormal bleeding causes. Unlike major surgeries, it is usually performed on an outpatient basis, meaning patients can often go home the same day.
The procedure is highly valuable because it provides clear and direct visualization of the uterine cavity, helping doctors make accurate diagnoses and plan effective treatments.
For many women, diagnostic hysteroscopy is a quick, safe, and reliable way to get answers about fertility issues, menstrual problems, or unexplained pelvic pain.
Types of Diagnostic Hysteroscopy
According to trusted medical resources, there are several types of Diagnostic Hysteroscopy.
- Outpatient (Office) Hysteroscopy: This is done in the doctor's clinic without general anesthesia. A very thin hysteroscope is used, and most women can tolerate the procedure with little to no discomfort. It's quick, convenient, and usually allows you to return to daily activities immediately.
- Operative-Combined Diagnostic Hysteroscopy: Sometimes, if a problem such as a polyp or fibroid is found during the diagnostic hysteroscopy, the doctor may proceed to remove it in the same sitting. This avoids the need for two separate procedures and helps in faster treatment.
- In-Patient Hysteroscopy: This type is performed in a hospital under anesthesia, especially if a woman is anxious, has a complex condition, or if doctors anticipate a need for minor operative correction along with diagnosis.
- Rigid Hysteroscopy: Uses a firm, straight scope that delivers high-quality images.Best for accurate diagnosis, though it may cause more discomfort than flexible scopes.
10-30 Minutes
Surgery Duration
Local, Regional, or General Anesthesia
Anesthesia Used

When is Diagnostic Hysteroscopy Recommended?
Diagnostic hysteroscopy is recommended when non-invasive tests like ultrasound don't give enough clarity. It helps doctors directly visualize the uterine cavity and detect hidden problems.
- Abnormal Uterine Bleeding (AUB): When periods are too heavy, irregular, or prolonged, hysteroscopy helps identify the root cause, such as fibroids, polyps, or hormonal imbalance.
- Infertility Evaluation: Women struggling to conceive may undergo hysteroscopy to check for uterine abnormalities like adhesions, septum or scar tissue that could affect implantation.
- Recurrent Miscarriages: If a woman experiences multiple pregnancy losses, hysteroscopy is done to detect uterine malformations or growths interfering with pregnancy.
- Suspected Fibroids or Polyps: It provides a clear view of growths inside the uterus, helping doctors plan removal if necessary.
- Thickened Endometrium or Endometrial Hyperplasia: When ultrasound shows thick uterine lining, hysteroscopy allows biopsy collection for further diagnosis.
- Postmenopausal Bleeding: Any unexplained bleeding after menopause is a red flag. Hysteroscopy helps rule out conditions like polyps, endometrial atrophy, or even cancer.
- IUD Problems: It helps check for misplaced, embedded, or broken intrauterine devices (IUDs) and assists in their safe removal.
Preparing for Diagnostic Hysteroscopy
Preparing well before your hysteroscopy helps ensure a safe procedure, accurate results, and a smoother experience overall.
Medical Evaluation & Pre-Procedure Visit
- Your doctor will review your medical history, menstrual cycle, and current medications.
- Basic tests such as blood work, urine tests, or imaging may be recommended to rule out infections or other underlying conditions.
- The timing of the procedure is usually scheduled right after your period when the uterine lining is thin, giving the clearest view.
Health Habits & Lifestyle Adjustments
- Stop smoking at least 2-4 weeks before the procedure, as it affects healing and anesthesia response.
- Avoid blood-thinning medications (aspirin, NSAIDs, certain supplements) as advised by your doctor to minimize bleeding risk.
- Eat a healthy diet rich in fruits, vegetables, and proteins to prepare your body for smooth recovery.
Preparing Your Home and Support System
- Arrange for someone to accompany you to the hospital and bring you home afterward, especially if anesthesia or sedation is used.
- Keep sanitary pads at home, as light spotting is common after the procedure.
- Prepare comfortable, loose-fitting clothes for the day of the procedure to avoid pressure on the abdomen.
The Day Before & Day of Procedure
- If general anesthesia is planned, you'll need to fast (no food or drink) for 6-8 hours before the procedure.
- Take prescribed medications such as antibiotics or cervical softening agents as instructed.
- Empty your bladder before the procedure for comfort and better visibility.
- Arrive at the hospital on time and follow any last-minute instructions given by your healthcare team.
What Happens During Diagnostic Hysteroscopy Surgery?
During a diagnostic hysteroscopy, a doctor uses a thin, lighted instrument called a hysteroscope to look inside the uterus. This simple, minimally invasive procedure helps identify and evaluate uterine problems like abnormal bleeding, fibroids, or polyps.
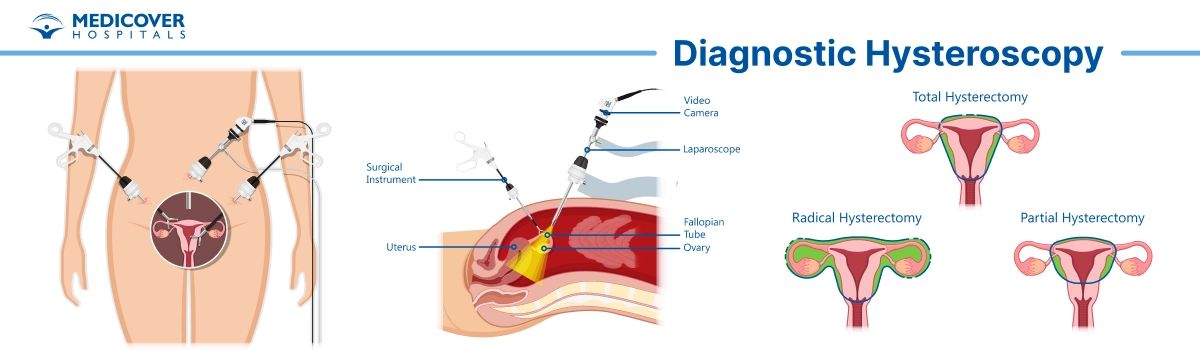
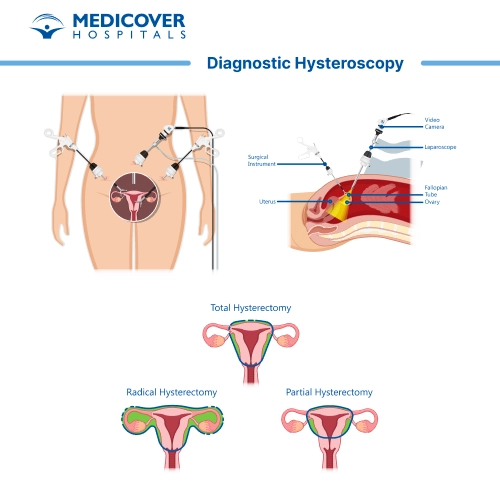
- Preparation & Anesthesia: On the day of the procedure, your doctor will review your medical history and answer last-minute questions. Most diagnostic hysteroscopies are done under local anesthesia or mild sedation, though general anesthesia may be used if combined with other treatments.
- Insertion of the Hysteroscope: The doctor gently inserts a thin, lighted tube called a hysteroscope through the vagina and cervix into the uterus. To make viewing easier, sterile saline solution or gas is introduced, expanding the uterine cavity.
- Examination of the Uterus: The hysteroscope transmits high-quality images onto a monitor, allowing the doctor to thoroughly examine the uterine walls. They look for problems such as fibroids, polyps, scar tissue, or abnormal growths.
- Biopsy or Minor Interventions (if needed): If suspicious tissue is found, a small biopsy may be taken for lab testing. In some cases, minor corrections like removing a small polyp or adhesion can be performed during the same session.
- Completion of the Procedure: Once the evaluation is complete, the hysteroscope is gently removed. The procedure usually takes 15-30 minutes and is minimally invasive, leaving no cuts or external scars.
- Recovery Period: You'll rest for a short while before going home the same day. Light cramping or spotting may occur for a couple of days, but most patients resume normal activities quickly.
Who Performs a Diagnostic Hysteroscopy?
A gynecologist or a gynecologic specialist is the doctor who performs a diagnostic hysteroscopy. These are medical professionals trained to care for the female reproductive system.
Here's what you should know:
- Gynecologist: This is the main type of doctor who treats issues related to the uterus, ovaries, and menstrual health. They are trained to perform hysteroscopies safely.
- Fertility Specialist: If you're undergoing the procedure as part of infertility evaluation, a fertility expert may perform it.
- Hospital: The procedure is usually done in a hospital or outpatient center. In some cases, it can be done in the doctor's office.
Recovery After Diagnostic Hysteroscopy
Recovering from diagnostic hysteroscopy is usually quick and smooth since it's a minimally invasive procedure. Still, knowing what to expect helps you feel more confident and prepared.
First Few Hours After the Procedure
- Mild cramping, spotting, or watery discharge is common right after the procedure.
- You'll rest in the hospital or clinic for a short while before being discharged.
- Avoid driving immediately after if you had anesthesia, arrange for someone to take you home.
Doctor's Tip: "Mild cramps are similar to period pain and usually subside with over-the-counter pain relief."
First Few Days
- Expect light bleeding or pink discharge for 1-2 days. Use sanitary pads instead of tampons to reduce infection risk.
- Cramping may continue but should improve each day.
- Avoid sexual intercourse, swimming, or using vaginal products for at least 48 hours (or as your doctor advises).
Doctor's Tip: "Give your uterus time to settle, don't rush into activities that could irritate it."
1 Week After Procedure
- Most women are back to normal daily activities within 24-48 hours, but if a biopsy was taken, mild discomfort may last a little longer.
- If you had general anesthesia, slight fatigue may linger for a few days.
- Light exercise like walking is fine, but avoid strenuous activity or heavy lifting.
Doctor's Tip: "Listen to your body. Resume normal activity gradually instead of all at once."
2 to 4 Weeks After Procedure
- By this time, all discomfort and spotting should be resolved.
- Your doctor may review biopsy results (if taken) and discuss next steps.
- Any persistent or unusual symptoms (heavy bleeding, fever, foul-smelling discharge) should be reported immediately.
Doctor's Tip: "Don't ignore red flags, early reporting ensures timely treatment if anything is wrong."
Diagnostic hysteroscopy is generally safe and well-tolerated, but like any medical procedure, it comes with both advantages and some risks you should be aware of.
Benefits of Diagnostic Hysteroscopy
- Accurate Diagnosis: Provides a clear, direct view of the uterine cavity, helping detect fibroids, polyps, adhesions, or abnormal bleeding causes more precisely than ultrasound.
- Minimally Invasive: Requires no major cuts, performed through the natural vaginal route, leading to quicker recovery compared to open surgical options.
- Quick Recovery: Most women return to daily activities within a day or two, making it convenient for busy lifestyles.
- Opportunity for Immediate Treatment: In some cases, small polyps or adhesions discovered during the diagnostic procedure can be treated right away, avoiding a second surgery.
- Improves Fertility Planning: Helps identify conditions that might affect pregnancy, such as uterine abnormalities or scar tissue, giving doctors better direction in fertility care.
Risks of Diagnostic Hysteroscopy
Diagnostic hysteroscopy is generally safe, but like any medical procedure, there are some potential risks and complications. These are rare but important to be aware of:
- Cramping and Spotting: Mild discomfort and light bleeding are common but usually resolve quickly with simple care.
- Infection: Low risk, but vaginal infection or pelvic infection can occur, your doctor may give preventive antibiotics in some cases.
- Uterine Perforation (Rare): Very rarely, the hysteroscope may puncture the uterine wall. This usually heals on its own but sometimes needs further care.
- Reaction to Anesthesia: If anesthesia or sedation is used, there's a small risk of nausea, dizziness, or allergic reaction.
- Fluid Overload (Rare): If fluid is used to expand the uterus, in rare cases, too much may be absorbed, affecting electrolytes, your surgical team carefully monitors this.
What is the Cost of Diagnostic Hysteroscopy?
The cost of a diagnostic hysteroscopy in India typically ranges between 25,000 and 60,000, depending on factors such as Hospital facilities & location, Surgeon's expertise, and Type of anesthesia used.























































































