What is Diabetic Retinopathy Treatment?
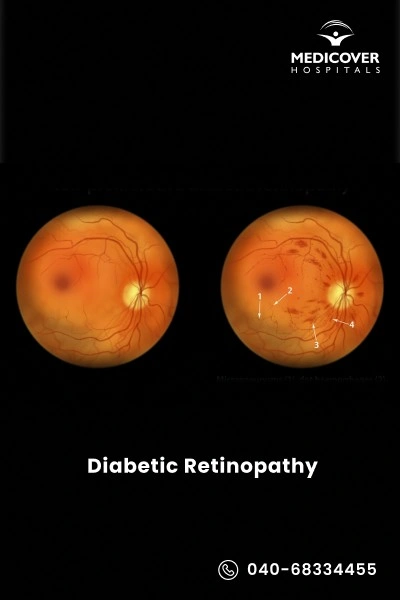
Diabetic retinopathy is a serious eye condition caused by long-term high blood sugar in people with diabetes. It damages the tiny blood vessels in the retina, leading to vision problems and, if untreated, blindness.
Early stages may not show symptoms, which is why regular eye checkups are very important. The goal of treatment is to slow down the disease, prevent further damage, and protect your vision.
Common Treatment Options:
- Laser Therapy (Photocoagulation): Used to seal or shrink abnormal blood vessels and prevent further leakage.
- Anti-VEGF Injections: Medicines injected into the eye to reduce swelling and stop new abnormal blood vessels from forming.
- Vitrectomy surgery is a surgical procedure to remove scar tissue or blood from the eye's vitreous gel.
- Corticosteroid Injections: Sometimes used to reduce retinal swelling.
- Blood Sugar and Blood Pressure Control: Essential to slow the progression of the disease and protect vision.
Types of Diabetic Retinopathy
Diabetic retinopathy is classified into three main types based on the severity of the condition:
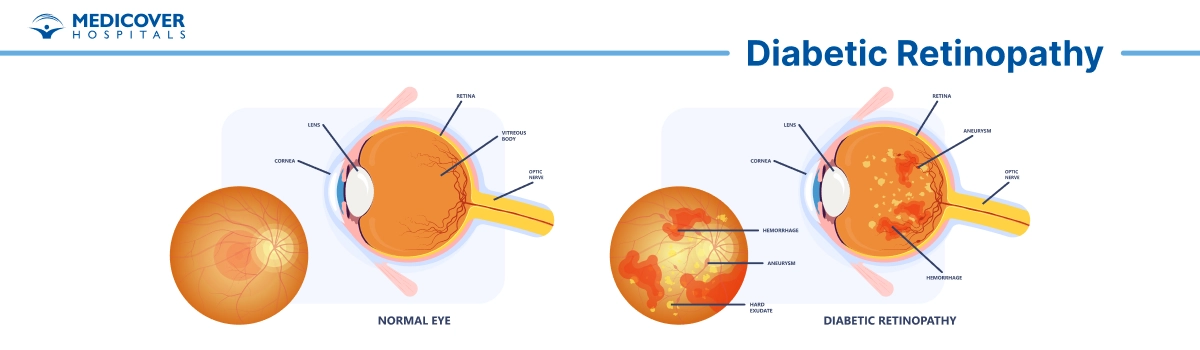
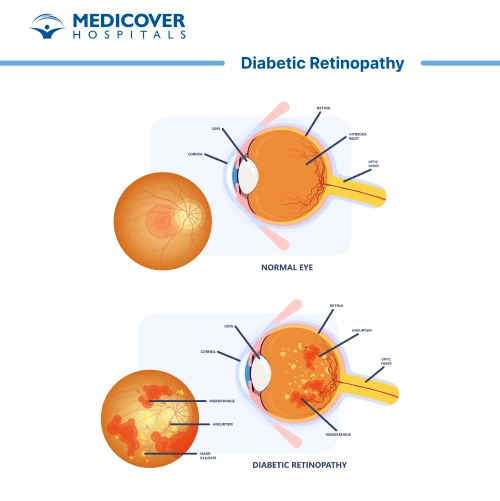
- Non-Proliferative Diabetic Retinopathy (NPDR): The early stage of the disease, where small blood vessels in the retina weaken, causing leakage and swelling.
- Proliferative Diabetic Retinopathy (PDR): A more advanced stage where new blood vessels grow in the retina, which are fragile and prone to bleeding, leading to more severe vision problems.
- Diabetic Macular Edema (DME): Swelling of the macula, which can cause vision distortion, often occurring in conjunction with either NPDR or PDR.
30 to 60 Minutes
Surgery Duration
Numbing Eye Drops or General Anesthesia
Anesthesia Used
1-2 Weeks
Full Recovery Timeline
When is Diabetic Retinopathy Treatment Recommended?
Treatment for diabetic retinopathy is recommended when the damage to the blood vessels in the retina begins to affect vision or shows signs of progressing. Indications of Diabetic Retinopathy include:
- Blurred Vision: Vision may become blurry or fluctuating, particularly if fluid is leaking into the retina, which can distort sight.
- Vision Disturbances: Diabetic retinopathy disease can cause the appearance of dark spots or floaters in the field of vision due to internal bleeding in the retina. These can obstruct clear vision and affect daily activities.
- Sudden Loss of Vision: In some cases, diabetic retinopathy can lead to sudden, severe vision loss, often caused by bleeding into the eye or a retinal detachment. Immediate intervention is necessary to prevent permanent damage.
- Difficulty Seeing at Night: As diabetic retinopathy progresses, difficulty seeing in low-light conditions can develop. This can impact activities like driving at night.
- Gradual Decrease in Vision: Over time, untreated diabetic retinopathy can cause a gradual decline in vision, especially if blood vessels in the retina are leaking or becoming blocked.
Preparing for Diabetic Retinopathy
Preparing for the diabetic retinopathy surgery is essential for ensuring a smooth and safe treatment experience. Below are the key steps to follow:
- Medical Evaluation: A complete eye examination and general health check-up are done before surgery.
- Blood Sugar Control: Keeping blood sugar, blood pressure, and cholesterol under control reduces risks during and after surgery.
- Medication Review: Inform the doctor about all medicines being taken. Some blood thinners may need to be stopped before surgery.
- Fasting Instructions: If general anesthesia is planned, the patient may be asked not to eat or drink for several hours before the procedure.
- Arrange Support: Patients should have someone to accompany them home after surgery since vision may be blurred temporarily.
Steps Involved in Diabetic Retinopathy Procedure
During a diabetic retinopathy procedure, a healthcare provider uses a specialized instrument called a hysteroscope to visually examine the inside of the uterus. The procedure for diabetic retinopathy surgery usually involves the following steps:
- Anesthesia: Local or general anesthesia is given to ensure the patient feels no pain during surgery.
- Vitrectomy: The surgeon makes small incisions in the eye and removes the blood-filled vitreous gel that clouds vision.
- Retinal Repair: Scar tissue pulling on the retina is removed, and in some cases, a gas bubble or silicone oil is placed to hold the retina in position.
- Laser Treatment (Photocoagulation): A laser is used to seal leaking blood vessels and prevent further bleeding.
- Medication Injection: Anti-VEGF injections may be given to reduce abnormal blood vessel growth and swelling.
- Closure & Recovery: The eye is carefully closed, and a protective patch is applied. Patients are monitored for vision improvement and healing progress.
This combination of techniques makes diabetic retinopathy surgery effective in stabilizing or improving vision in people with advanced stages of the condition.
Who Performs the Diabetic Retinopathy Procedure?
Diabetic retinopathy is typically managed and treated by eye care professionals, specifically ophthalmologists specialising in retinal diseases. These specialists have the expertise and training to diagnose, monitor, and treat diabetic retinopathy and its associated complications. Here are the types of healthcare professionals involved in the treatment of diabetic retinopathy:
Recovery After Diabetic Retinopathy
Recovery after treatment depends on the type of procedure received, such as laser therapy, injections, or surgery.
- Immediate Post-Procedure Symptoms: Blurry vision, mild irritation, and light sensitivity; these usually improve within a few hours to a day.
- Pain Management: Mild discomfort can be relieved with over-the-counter pain relievers; any discomfort typically fades quickly.
- Activity Restrictions: Avoid heavy lifting and strenuous activities for a few days; do not drive if vision is blurry or sedation is used; limit screen time to reduce eye strain.
- Vision Improvement: Temporary blurry vision is common; gradual improvement in vision as healing progresses.
- Follow-Up Appointments: Essential to monitor recovery and detect any complications; ensure the procedure's effectiveness.
- Long-Term Care: Control blood sugar levels to prevent further retinal damage; continue regular eye exams and follow your diabetes management plan.
Lifestyle Changes After Diabetic Retinopathy
- Maintain Blood Sugar Levels: Keeping blood sugar levels under control is crucial to prevent further damage to the retina and overall eye health.
- Healthy Diet: Follow a balanced diet rich in fruits, vegetables, whole grains, and lean proteins to support overall health and manage diabetes effectively.
- Regular Exercise: Engage in regular physical activity to help control blood sugar and improve circulation, which benefits eye health.
- Monitor Eye Health: Schedule regular eye exams with your ophthalmologist to track the health of your retina and detect any early signs of complications.
- Quit Smoking: Smoking can worsen diabetic retinopathy, so quitting is essential for preserving eye health and reducing further risk.
- Control Blood Pressure and Cholesterol: Keeping blood pressure and cholesterol levels within healthy ranges can prevent additional stress on the retina and help protect your vision.
- Limit Alcohol Intake: Excessive alcohol consumption can affect blood sugar control and overall health, so it's important to limit intake.
- Wear Sunglasses: Protect your eyes from UV rays by wearing sunglasses to reduce strain on the eyes and protect the retina from further damage.
Benefits of Diabetic Retinopathy
The treatment for diabetic retinopathy is primarily aimed at stopping the progression of the disease and preventing further damage to the retina. The benefits include:
- Helps slow or stop the progression of diabetic retinopathy.
- Preserves vision and prevents severe vision loss.
- Improves quality of life by maintaining independence and daily activities.
- Reduces the risk of blindness when treated at an early stage.
Complications and Risks Associated with Diabetic Retinopathy
Like any medical procedure, treatments for diabetic retinopathy also carry certain risks and side effects, though most are temporary and manageable.
- Temporary blurred vision or eye irritation after procedures.
- Light sensitivity and discomfort for a short period.
- Rare chances of bleeding or infection in the eye.
- In some cases, treatment may not fully restore lost vision but can prevent further damage.
Cost of Diabetic Retinopathy Treatment in India
The cost of Diabetic Retinopathy treatment in India varies depending on the stage of the disease and the type of treatment required.
- Laser treatment (Photocoagulation): Rs. 10,000 - Rs. 30,000 per eye
- Vitrectomy surgery: Rs. 60,000 - Rs. 1,20,000 per eye
- Anti-VEGF injections (like Avastin, Eylea, Lucentis): Rs. 8,000 - Rs. 40,000 per injection
Overall, the cost usually ranges between Rs. 10,000 and Rs. 1,20,000, influenced by hospital facilities, doctor expertise, city, and technology used.




































