What is Cervical Cerclage?
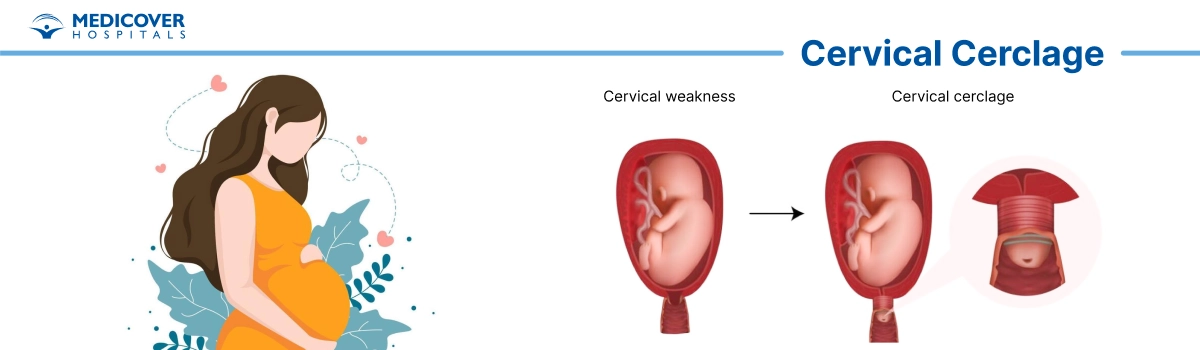
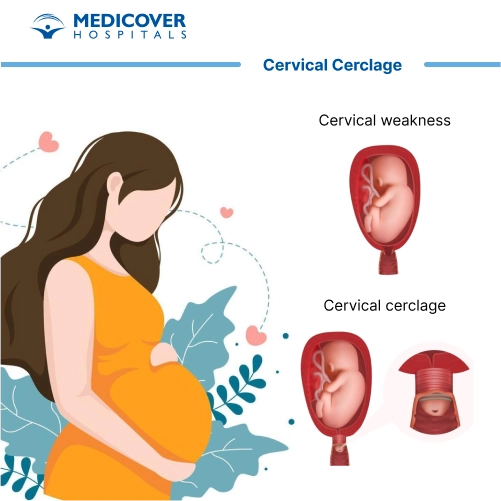
Cervical cerclage is a medical procedure performed during pregnancy to prevent premature birth or miscarriage. It involves placing a strong stitch (suture) around the cervix , the lower part of the uterus , to keep it closed and provide extra support until the baby is ready for delivery.
This procedure is usually recommended for women with cervical insufficiency (a weak cervix that opens too early), a history of preterm births, or those identified as high-risk during pregnancy. By reinforcing the cervix, cervical cerclage helps reduce the chances of pregnancy complications and increases the likelihood of carrying the baby safely to full term.
Types of Cervical Cerclage
According to medical experts, there are a few different types of cervical cerclage, chosen based on the mother's health, pregnancy stage, and cervical condition.
McDonald Cerclage
It is the most prevalent one, carried out by way of the vagina. A stitch is put around the cervix in the form of a purse-string to keep it closed. It is typically administered between 12 and 14 weeks of pregnancy, and it is taken near the delivery.
Shirodkar Cerclage
Like the McDonald technique, only that the stitches are placed deeper and nearer to the uterus to provide more significant support. It may involve lifting the bladder slightly to reach the cervix. Often recommended in cases of substantial cervical weakness.
Transabdominal Cerclage
Used when vaginal cerclage is not possible or has failed in the past. The stitch is placed through the abdomen, usually laparoscopically or via open surgery. In this type, the stitch often remains in place for future pregnancies.
30-60 Minutes
Surgery Duration
Spinal, Epidural, or General Anesthesia
Anesthesia Used

When is Cervical Cerclage Recommended?
Cervical cerclage is usually advised when the cervix is too weak to hold a pregnancy on its own, increasing the risk of preterm birth or miscarriage. Based on clinical guidance, here are the main reasons why doctors recommend it:
- History of Cervical Insufficiency or Preterm Birth: If a woman has previously experienced a miscarriage or premature delivery due to a weak cervix, cerclage may be recommended early in the subsequent pregnancy to provide stronger cervical support.
- Short Cervix Detected in Ultrasound: During routine pregnancy scans, if the cervix appears shorter than usual, it may not be strong enough to stay closed. In such cases, placing a stitch can help reduce the risk of early labour.
- Cervical Changes in Current Pregnancy: Sometimes, during pelvic exams or ultrasounds, doctors may notice that the cervix is already starting to open or thin too soon. An "emergency cerclage" may be placed to protect the pregnancy.
Preparing for Cervical Cerclage Surgery Procedure
Cervical cerclage should be prepared way in advance to make the surgery easier and the birth of a baby healthier.
Medical Evaluation & Pre-Op Tests
Your physician will review your entire medical history, the progress of your pregnancy, and the earlier complications. Ultrasound is commonly done to examine the length and status of the cervix to schedule the operation.
Medications & Lifestyle Adjustments
You may be advised to avoid certain medications, smoking, or alcohol, as these can affect healing and pregnancy health. Doctors might also prescribe antibiotics or progesterone to lower the risk of infection and preterm contractions.
Planning for the Hospital Stay
Cervical cerclage is usually a short procedure, but you may be asked to stay for a few hours or overnight for monitoring. Arrange for a support person to accompany you and help with travel and post-procedure care.
Day of the Procedure
Follow fasting instructions (usually no food or drink for 6-8 hours before surgery if anaesthesia is planned). Wear comfortable clothing and avoid heavy meals or stress before heading to the hospital.
What Happens During Abdominoplasty Surgery?
Cervical cerclage is a relatively simple surgical procedure designed to give your pregnancy extra support by reinforcing a weak cervix.
- Anesthesia & Preparation: The procedure is usually done under regional (spinal/epidural) or general anaesthesia so that you won't feel pain. Your doctor ensures both you and your baby are stable before starting.
- Accessing the Cervix: Using a speculum (like during a pap smear), the cervix is gently visualised. No abdominal cuts are required, as the entire procedure is done vaginally in most cases.
- Placing the Stitches: A powerful surgical thread is sewn around the cervix, the size of a purse, and this tightens and holds it shut. This will be used to avoid premature delivery, which may cause early labour or miscarriage.
- Duration & Recovery: This is generally done in 30-45 minutes. A majority of women can go home in a few hours after observing contractions, bleeding or any form of discomfort.
- Follow-up Care: You'll need regular ultrasounds and checkups to monitor cervical length and stitch placement. The cerclage is usually removed around 36-37 weeks of pregnancy, or earlier if labour begins.
Who Will You Contact for Cervical Cerclage Surgery?
- Consult Your Obstetrician/Gynecologist (OB/GYN): Your first step should be to consult your regular OB/GYN. They will review your medical history, perform exams, and decide if cervical cerclage is right for you.
- High-Risk Pregnancy Specialist (Perinatologist/Maternal-Fetal Medicine Specialist): If you have a history of miscarriages, preterm births, or other pregnancy concerns, your OB/GYN might refer you to a specialist in high-risk pregnancies. These doctors are experts in complicated pregnancies and can provide more advanced care.
- Surgical Center or Hospital: Once the decision is made for cervical cerclage, your doctor will schedule the surgery at a hospital or surgical center. They will explain what to expect before, during, and after the procedure.
- Follow Medical Recommendations: Follow your doctor's instructions about any tests, fasting, or preparations needed before the surgery.
- Recovery and Post-Operative Care: After the surgery, follow the care instructions from your doctor. This may include avoiding heavy activities, taking prescribed medications, and attending follow-up appointments to ensure proper healing.
Recovery After Cervical Cerclage Procedure
Recovery is usually smooth, but following your doctor's advice is key to a safe pregnancy journey.
First Few Days After Surgery
- Mild cramping, light spotting, or a pulling sensation in the abdomen is common.
- Rest is essential, avoid lifting, bending, or prolonged standing.
- Gentle movements are okay to maintain circulation.
Doctor's Tip: "Mild cramping and spotting are normal. Contact your doctor if you notice heavy bleeding or fluid leakage."
Weeks 2 to 4
- Discomfort usually reduces, and light daily activities may be resumed with medical advice.
- Regular follow-up visits and ultrasounds help monitor cervical health.
- Avoid sex and strenuous activity to prevent extra pressure on the cervix.
Doctor's Tip: "Follow-up checkups are crucial to make sure the stitch is doing its job.
Weeks 5 to 6
- Most women return to regular routines, but should still avoid heavy lifting or exercise.
- Your doctor may adjust activity levels based on cervical scans.
- Continue medications like progesterone, if prescribed.
Doctor's Tip: "Even if you feel fine, your cervix is still healing, don't rush into full activity."
Final Weeks of Pregnancy (36-37 Weeks)
- Stitch is usually removed in a simple, outpatient procedure.
- Removal is quick and mostly painless, requiring no anaesthesia.
- If labour begins early, the stitch is removed immediately to prevent complications.
Doctor's Tip: "Cerclage removal is routine and safe, it's one step closer to meeting your baby."
Benefits of Cervical Cerclage Surgery
- Prevents Miscarriage or Preterm Birth: The main benefit is supporting women with a weak or short cervix. By keeping the cervix closed, cerclage helps reduce the risk of pregnancy loss and allows the baby more time to grow.
- Safe and Widely Practised Procedure: It has been used for decades and is considered safe, with a high success rate in prolonging pregnancies for women who are good candidates.
- Extra Support During Critical Weeks: The stitch helps when the cervix is under pressure, especially in the second trimester when risks are higher, giving the pregnancy a stronger chance of continuing.
- Emotional Reassurance for Mothers: Knowing that the cervix is secured provides peace of mind for many women, reducing anxiety about preterm delivery.
Risks of Cervical Cerclage Surgery
- Cramping, Spotting, or Discomfort: Mild pain, spotting, or cramping is common in the first few days after surgery. These symptoms usually settle with rest and prescribed medication.
- Infection Risks: Though uncommon, infections can occur at the stitch site or in the amniotic sac. Regular follow-ups and antibiotics when needed help reduce this risk.
- Preterm Contractions or Irritation: Sometimes, the stitch can irritate the cervix and trigger contractions, though doctors closely monitor and manage this with medication if needed.
- Premature Rupture of Membranes (Water Bag Breaking): In rare cases, the membranes can rupture early, which may lead to preterm labour or require stitch removal.
What is the Cost of Cervical Cerclage?
The cost of a cervical cerclage can vary depending on the hospital, doctor's expertise, type of cerclage performed (transvaginal or transabdominal), and additional medical needs such as anesthesia or hospital stay. On average, the procedure may range between 30,000 to 80,000.






















































































