What Is Cardiac Resynchronization Therapy (CRT)?
Cardiac Resynchronization Therapy (CRT) is a specialised treatment for patients with heart failure and abnormal heart rhythms. It involves implanting a small device that sends electrical signals to the heart's chambers, helping them beat in a more coordinated way. This improves the heart's pumping efficiency, reduces symptoms like fatigue and shortness of breath, and enhances overall quality of life.
CRT is usually considered for patients with weakened heart muscles, irregular electrical activity (such as left bundle branch block), or those who do not respond adequately to medications alone. While CRT significantly improves heart function, it is not a cure for heart failure and works best when combined with ongoing medical management and lifestyle changes.
Types of Cardiac Resynchronization Therapy
- CRT-P (Cardiac Resynchronization Therapy with a Pacemaker): This device uses a pacemaker to help synchronize the heart's contractions. It is mainly suited for patients with heart failure and conduction abnormalities but without a high risk of sudden, life-threatening arrhythmias.
- CRT-D (Cardiac Resynchronization Therapy with a Defibrillator): This device combines CRT with an implantable cardioverter-defibrillator (ICD). Along with coordinating heart contractions, it also monitors for dangerous arrhythmias and can deliver a shock if needed to restore a normal rhythm. CRT-D is typically recommended for patients with heart failure who are at high risk of sudden cardiac arrest.
2-4 Hours
Surgery Duration
Local Anesthesia
Anesthesia Used
4-6 Weeks
Full Recovery Timeline

Who Needs the Cardiac Resynchronization Therapy (CRT) Procedure?
Cardiac Resynchronization Therapy is recommended for patients with heart failure who show signs of electrical conduction delays and remain symptomatic despite medication. The key indications include:
- Symptomatic Heart Failure: Suitable for patients with NYHA Class II, III, or ambulatory Class IV symptoms who continue to experience limitations despite optimal drug therapy.
- Reduced Left Ventricular Ejection Fraction (LVEF): Recommended when LVEF is 35% or lower, indicating weakened pumping ability of the heart.
- Prolonged QRS Duration: QRS interval ?120 ms, especially with a left bundle branch block (LBBB), suggesting delayed ventricular activation that CRT can help correct.
- Sinus Rhythm: Most effective in patients with normal sinus rhythm. In atrial fibrillation cases, additional interventions such as AV nodal ablation may be required.
- Dilated Cardiomyopathy: Beneficial for both ischemic and non-ischemic cardiomyopathy when associated with ventricular dyssynchrony.
- Chronic Right Ventricular Pacing: Patients dependent on RV pacing with low LVEF may benefit from CRT to prevent pacing-induced dyssynchrony.
CRT is not appropriate for all heart failure patients-particularly those with narrow QRS complexes or reversible causes of heart failure. Careful evaluation with ECG and echocardiography is essential before deciding on this therapy.
Preparing for Cardiac Resynchronization Therapy (CRT)
Proper preparation for CRT helps ensure a safe procedure and faster recovery. Here's what you need to know:
Medical Evaluation & Pre-Procedure Check
- Meet your cardiologist to confirm if CRT is right for you.
- Share details of your medical history, including previous heart conditions, surgeries, and implanted devices.
- Routine tests such as ECG, echocardiogram, chest X-ray, and blood work may be required.
Medication & Lifestyle Adjustments
- Review your current medications with your doctor. Blood thinners, diabetes medicines, or certain heart drugs may need adjustment.
- Inform your healthcare team about all allergies, vitamins, or supplements you take.
- Follow a heart-healthy diet and lifestyle as recommended to support recovery.
Day Before & Day of Procedure
- Follow fasting instructions (commonly no food or drink after midnight before the procedure).
- Shower as advised, using mild soap around the chest area. Avoid lotions, powders, or perfumes.
- Wear loose, comfortable clothing and do not wear jewellery or makeup.
Hospital Stay & Recovery Planning
- After CRT, patients usually stay in the hospital for 1-2 days for monitoring and device adjustments.
- Transportation should be arranged at the time of discharge, as driving independently is not advised.
- A family member or friend should be available to assist during the first 24 hours at home post-discharge.
- The home environment can be prepared in advance with essentials such as medications, water, and light meals kept easily accessible.
Ask Questions & Clarify Doubts
- Discuss any concerns or questions with the doctor before the procedure.
- Ensure clear understanding of post-procedure care, follow-up appointments, and activity limitations.
What Happens During Cardiac Resynchronization Therapy (CRT)?
Preparing for Cardiac Resynchronization Therapy (CRT) involves several steps to ensure that you're ready for the procedure and that your health is optimized for a successful outcome. Here's a guide on how to prepare:
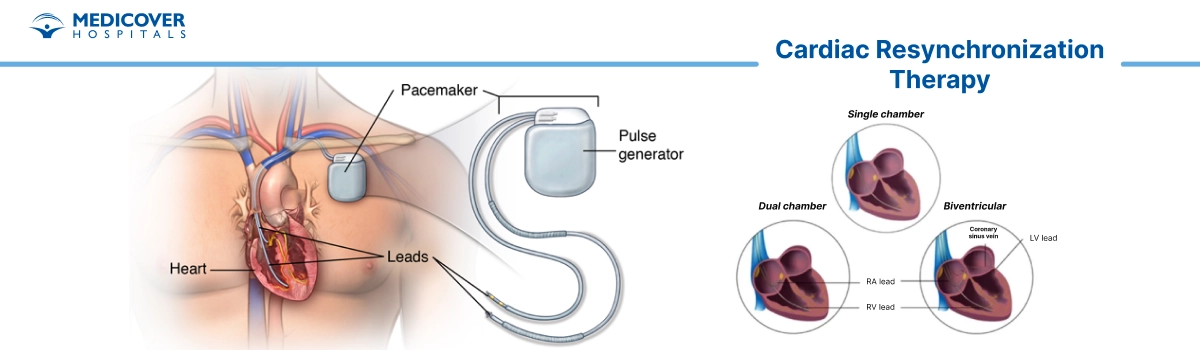
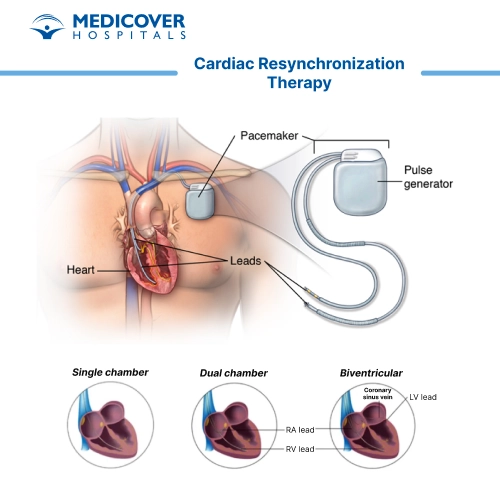
- Preparation & Anesthesia: Before the procedure, the healthcare team reviews medical history, current medications, and heart function tests such as ECG and echocardiography. After informed consent, anesthesia is administered to ensure the patient is relaxed and comfortable.
- Incision & Device Pocket Creation: A small incision is made near the collarbone. Through this incision, the surgeon creates a pocket just beneath the skin where the CRT device will be placed.
- Lead Placement in the Heart: Thin wires, called leads, are gently guided through a vein into the heart chambers. These leads are positioned carefully so they can deliver electrical signals to help the heart chambers beat in sync.
- Connecting the CRT Device: Once the leads are in place, they are attached to the CRT pacemaker or defibrillator. The device is then placed in the pocket under the skin.
- Testing & Optimization: The device is tested to confirm it is sending signals correctly and improving heart rhythm. Adjustments may be made to ensure the chambers are contracting in proper synchrony.
- Closing the Incision: The incision is closed with sutures, adhesive, or surgical tape, and a sterile dressing is applied to protect the area.
- Recovery & Monitoring: After surgery, the patient is moved to a recovery area where heart rhythm and vital signs are monitored closely. Most patients stay in the hospital overnight or up to 1-2 days for monitoring and device adjustments before being discharged.
- Post-Procedure Care: Follow-up appointments are scheduled to check device function and heart performance. The healthcare team also provides guidance on activity levels, wound care, and long-term management.
Recovery After Cardiac Resynchronization Therapy (CRT)
Recovery after a Cardiac Resynchronization Therapy (CRT) procedure is typically well-managed, and many patients experience improvements in their heart function and quality of life. Here's what you can expect during the recovery period:
First 24 Hours
- After the procedure, you'll stay under close monitoring. Your heart rhythm, blood pressure, and oxygen levels will be tracked to ensure the device is working correctly.
- You may be asked to lie still for several hours to reduce the risk of bleeding from the insertion site.
Doctor's Tip: "Mild soreness at the incision is expected. Report any unusual pain, swelling, or bleeding right away."
First Week
- During the first week, you may feel mild discomfort around the chest or shoulder where the device was placed. Keep the area clean and dry, and follow your wound care instructions.
- Limit arm movements on the side of the implant to allow proper healing. Avoid stretching overhead, lifting heavy objects, or sudden jerking movements.
Doctor's Tip: "Protect your incision site. Overusing the arm on that side can delay healing."
Weeks 2 to 4
- Most patients gradually feel more energetic as their heart function improves. You may be allowed to resume light daily activities such as walking and simple household tasks.
- Driving may be restricted for a short period, depending on your doctor's advice.
- Regular follow-up visits will be scheduled to check the incision and test the CRT device.
Doctor's Tip: "Follow-ups are not optional, they ensure your device is tuned to your heart's needs."
1 to 3 Months
- Swelling and discomfort should continue to ease. You can usually return to non-strenuous work and light exercises, but avoid vigorous workouts or lifting weights until cleared.
- Continue wearing loose clothing that doesn't irritate the incision site.
Doctor's Tip: "Even if you feel better, give your body time. Healing inside takes longer than you think."
Long-Term Care (3 Months and Beyond)
- By this stage, most people notice improvements in breathing, stamina, and daily comfort.
- Stick to heart-healthy habits, including a balanced diet, regular walking, stress management, and avoiding smoking or alcohol.
- Always inform healthcare professionals that you have a CRT device before medical procedures. Stay cautious around strong magnetic or electrical fields.
Doctor's Tip: "Your device helps your heart, but your lifestyle keeps it strong. Commit to both."
Benefits of Cardiac Resynchronization Therapy (CRT)
- Improves heart function: CRT restores coordination between the left and right ventricles, helping the heart pump more effectively.
- Relieves symptoms of heart failure: Patients often experience reduced shortness of breath, fatigue, and swelling, making daily activities easier.
- Increases exercise tolerance: By improving circulation, CRT enhances stamina and physical capacity.
- Reduces hospitalizations: Better heart performance lowers the risk of frequent admissions for heart failure complications.
- Enhances quality of life: With improved energy and reduced symptoms, many patients report a more active and fulfilling lifestyle.
- Lowers risk of serious events: CRT can decrease the risk of arrhythmias, strokes, and in some cases, heart failure-related death.
Risks of Cardiac Resynchronization Therapy (CRT)
Like any medical procedure, CRT has potential risks. Being informed helps patients make confident decisions.
- Infection at the incision or device site
- Bleeding or bruising around the implant area
- Lead-related issues may lead to the movement out of position or malfunction
- Pneumothorax is a rare lung injury during lead placement
- Venous thrombosis risk of blood clots in the veins
- Allergic reaction or anesthesia risks uncommon but possible
- Device malfunction requiring adjustment or replacement
- Pain or swelling at the incision or pocket site
Cost of Cardiac Resynchronization Therapy (CRT)
The cost of Cardiac Resynchronization Therapy (CRT) varies depending on several factors such as the type of device used (CRT-P or CRT-D), patient condition, duration of hospital stay, and associated medical requirements.
- CRT-P (Pacemaker only): Rs. 3,00,000 - Rs. 6,50,000
- CRT-D (with Defibrillator): Rs. 6,00,000 - Rs. 12,00,000
Our team at Medicover Hospitals ensures transparent guidance about the treatment plan and cost, helping patients and families make informed decisions.
Note: These figures are indicative and may differ based on individual medical needs and hospital policies. For an accurate estimate, it is best to consult directly with our cardiac specialists.






























