What is breast reconstruction surgery, and why is it important?
Breast Reconstruction is a surgical procedure used to rebuild the shape and appearance of a breast after it has been removed due to breast cancer, trauma, or congenital conditions. The goal of breast reconstruction is to restore a breast's natural look, feel, and symmetry, helping individuals regain their body image and confidence.
This type of surgery holds immense importance for individuals who have undergone mastectomy as part of breast cancer treatment or have experienced traumatic breast injuries, as it contributes to their physical and emotional recovery and helps restore their sense of self and femininity.
Types of Breast Reconstruction Surgeries
It's essential to understand the different breast reconstruction surgery options available. This procedure can be performed using implants, your own tissue (flaps), or a combination of both. The best choice depends on:
- Your body type and anatomy
- Medical history and overall health
- Type of cancer treatment received (especially radiation)
- Personal expectations for recovery, look, and feel
Here are the main types of breast reconstruction surgery:
Implant-Based Reconstruction
This technique uses a breast implant to recreate the breast shape. The implant may be placed either under the chest muscle or above it, depending on what will provide the best support and appearance.
Placement options:
- Subpectoral: Implant placed beneath the chest muscle.
- Subcutaneous (pre-pectoral): Implant placed above the muscle and under the breast tissue.
Types of implants:
- Saline-filled: Contains sterile saltwater solution.
- Silicone-filled: Filled with silicone gel, which feels more like natural breast tissue.
Why choose this option?
- Shorter surgery and quicker recovery compared to flap methods.
- Suitable for women with enough breast tissue and skin to support the implant.
Autologous Tissue (Flap) Reconstruction
This method uses your own tissue, usually from the abdomen, back, thighs, or buttocks, to rebuild the breast. It's often chosen for a more natural look and feel, especially when implants are not suitable.
Common flap techniques include:
- TRAM Flap (Transverse Rectus Abdominis Myocutaneous): Uses tissue and muscle from the abdomen.
- DIEP Flap (Deep Inferior Epigastric Perforator): Uses abdominal skin and fat while sparing the muscles.
- Latissimus Dorsi Flap: Uses tissue from the back, sometimes combined with an implant.
- SGAP Flap (Superior Gluteal Artery Perforator): Uses tissue from the upper buttocks.
- IGAP Flap (Inferior Gluteal Artery Perforator): Uses tissue from the lower buttocks.
- TUG Flap (Transverse Upper Gracilis): Uses tissue from the inner thigh.
Why choose this option?
- Provides a softer, more natural breast appearance.
- Ideal for women who don't want implants or had radiation therapy that damaged chest tissue.
- Longer surgery and recovery time compared to implants.
Some women may also choose a hybrid reconstruction, combining implants with flap tissue to achieve the best shape and balance.
2 to 6 hours
Surgery Duration
General Anesthesia
Anesthesia Used
Same Day Discharge
Hospital Stay
4 weeks to Several months
Full Recovery Timeline

Who needs breast reconstruction surgery?
Breast reconstruction is most often considered after a mastectomy (removal of one or both breasts due to cancer), but it may also be performed for other medical or personal reasons.
The decision is highly individual, based on health needs and emotional well-being.
- Breast Cancer Treatment: Breast reconstruction helps restore the physical appearance after mastectomy, improving well-being and aiding emotional healing during cancer recovery.
- Traumatic Injury or Accidents: Reconstruction can help restore the appearance of the breast after injury or trauma and improve both self-esteem and emotional health.
- Congenital Deformities: Breast reconstruction can correct congenital issues, like asymmetry or underdevelopment, for a more balanced appearance.
- Prophylactic Mastectomy: High-risk women can choose preventive mastectomy (risk reduction), followed by reconstruction, to reduce cancer risk while maintaining breast contour.
- Improved Body Symmetry: Breast reconstruction helps achieve body symmetry, significantly when only one breast is affected by surgery or trauma.
- Enhanced Emotional Well-Being: Restoration of a natural-looking breast improves self-esteem and overall emotional health.
- Aesthetic Preferences: Some women opt for breast reconstruction for aesthetic reasons, seeking a more symmetrical and pleasing appearance.
How should you prepare for breast reconstruction surgery?
Preparation is an important step in ensuring the best results and smooth recovery. Your doctor will guide you through the process, but here are some key things to keep in mind:
- Consult Your Surgeon: Have an open and honest conversation with your breast reconstruction specialist about your goals, expectations, and any concerns you may have. Inquire about the various types of reconstruction and determine which option best suits you.
- Health Evaluation: Your medical team may recommend blood tests, imaging, or other assessments to confirm that you're fit for surgery. Managing chronic conditions like diabetes, heart disease, or high blood pressure is essential before undergoing the procedure.
- Quit Smoking and Limit Alcohol: Smoking and excessive alcohol use can slow down healing and increase risks during surgery. Your surgeon will likely ask you to quit smoking and reduce alcohol intake weeks before the procedure.
- Review Medications: Share a full list of your current medications, vitamins, and supplements. Some may need to be adjusted or stopped before surgery (for example, blood thinners).
- Healthy Lifestyle: Focus on balanced nutrition, regular physical activity, and staying hydrated. A healthy body heals faster and lowers the chance of complications.
- Arrange Support at Home: After surgery, you'll need help with daily tasks, meals, and transportation. Plan ahead and have a family member, friend, or caregiver available during your recovery period.
- Mental Preparation: Many women feel nervous or anxious before surgery. It may help to join support groups, speak with a counselor, or connect with other breast cancer survivors who have undergone reconstruction.
What Happens During Breast Reconstruction Surgery?
Breast reconstruction is a planned, step-by-step procedure that may differ based on whether you choose implant-based reconstruction or autologous (flap) reconstruction. Below is an overview of the general process:
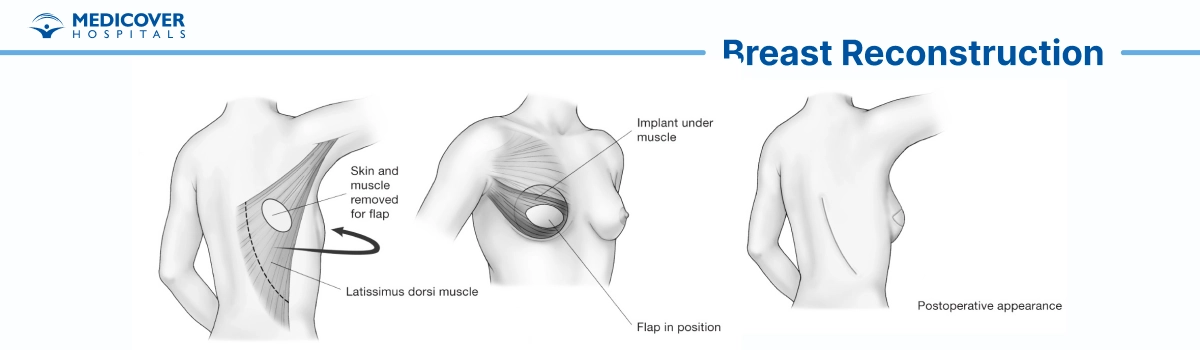
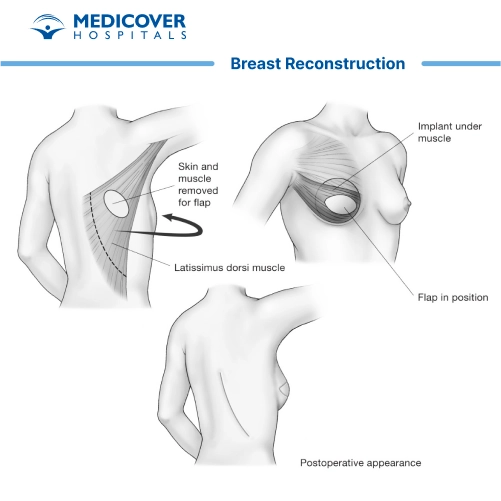
Anesthesia
The surgery begins with anesthesia to keep you comfortable and pain-free. Most often, general anesthesia is used, which means you'll be asleep throughout the procedure.
Incision and Tissue Preparation
The surgeon makes incisions depending on the chosen technique:
- For implant reconstruction, incisions may be placed in the breast crease, around the areola, or under the arm.
- For flap reconstruction, tissue is carefully taken from donor areas like the abdomen, thigh, or buttocks and prepared for transfer.
Implant Placement or Tissue Transfer
- Implant-based reconstruction: The surgeon creates a pocket and inserts a saline or silicone implant.
- Flap reconstruction: Your own tissue is shaped and placed to form a natural-looking breast mound.
Nipple and Areola Reconstruction (Optional)
In some cases, nipple and areola reconstruction is done during the same procedure. This may involve creating a nipple mound and using tattooing or grafting for a natural appearance.
Closing the Incisions
After shaping the breast, the surgeon carefully closes the incisions with sutures. Surgical dressings or tape are applied to protect the wound and promote healing.
Drain Placement (if needed)
Temporary drains may be inserted to remove excess fluid and reduce swelling. These are usually taken out within a few days to a week, depending on your recovery.
Who Conducts Breast Reconstruction Surgery?
Breast reconstruction surgery is a specialised procedure that involves a team of healthcare specialists working together to ensure the best possible outcome for the patient. Breast reconstruction surgery involves a collaborative team of specialists:
- Breast Surgeon
- Plastic Surgeon
- Anesthesiologist
- Nurse Navigator
Recovery After Breast Reconstruction Surgery
Recovery after breast reconstruction surgery is a step-by-step process that requires time, patience, and proper care.
The exact recovery timeline depends on the surgical technique used (implant-based or flap), your overall health, and how your body heals. Here's what you can generally expect:
Immediate Postoperative Period
- Hospital Stay: You may spend a few days in the hospital for observation and initial recovery.
- Pain Management: Pain or soreness is common, and your doctor will prescribe medications to keep you comfortable.
- Monitoring: Medical staff will closely check your vital signs, incision sites, and overall condition during this stage.
Recovery at Home
- Follow Instructions: Carefully follow your surgeon's advice on wound care, dressing changes, and activity levels.
- Rest & Activity: Rest well and gradually return to light activities. Avoid heavy lifting or strenuous movements until cleared.
- Drain Care: If surgical drains are placed, you'll need to monitor fluid output and keep the area clean as instructed.
- Medications: Take antibiotics and pain relievers as prescribed to prevent infection and ease discomfort.
- Compression Garments: Wear a surgical bra or compression garment to minimize swelling and support healing.
- Diet & Hydration: Eat nutrient-rich foods and drink plenty of water to boost recovery.
- Wound Care: Keep incisions clean and dry to avoid infections.
- Follow-Ups: Attend all scheduled check-ups so your surgeon can track your progress.
Long-Term Recovery
- Scar Care: Use recommended scar creams or silicone sheets to help minimize scarring over time.
- Physical Therapy: Some patients may benefit from gentle stretching or therapy sessions to restore strength and mobility.
- Emotional Support: Recovery isn't just physical. Counseling or support groups can help you cope emotionally and regain confidence.
- Returning to Normal Activities: Gradually resume work, exercise, and other routines once your doctor confirms it's safe.
Lifestyle Changes after Breast Reconstruction Surgery
After undergoing breast reconstruction surgery, certain lifestyle adjustments can help promote healing, enhance overall well-being, and ensure the best possible outcomes.
Here are some lifestyle changes and considerations to keep in mind during your recovery and beyond:
- Follow Medical Advice: Stick to your doctor's instructions for wound care, medication, and activity limits.
- Eat and Hydrate Well: Eat a healthy diet to aid healing and avoid dehydration.
- Avoid Smoking & Alcohol: Stop smoking and limit alcohol to help lower complications and aid recovery.
- Stay Active Gradually: Begin light activities as approved by your doctor to boost circulation and prevent clots.
- Wear Supportive Bras: Use bras or garments recommended by your surgeon for comfort and support.
- Care for Scars: Follow scar care guidelines and protect scars from the sun to reduce visibility.
- Emotional Wellness: Focus on mental health with relaxing activities, counselling, or support groups if needed.
- Attend Follow-Ups: Regular appointments help check on the healing progress and correct any problems.
- Choose Comfortable Clothing: Wear outfits that make you feel confident and comfortable.
- Practice Self-Care: Stay positive, accept your body, and engage in activities that make you happy.
Benefits, Side Effects, and Risks of Breast Reconstruction Surgery
Breast reconstruction surgery offers many positive outcomes, but like any major surgery, it also comes with potential side effects and risks. Understanding both helps you make an informed decision about whether the procedure is right for you.
Benefits of Breast Reconstruction Surgery
- Boosts Confidence: Restores self-esteem and body image after mastectomy, trauma, or congenital issues.
- Restores Symmetry: Balances the chest, especially when only one breast is affected.
- Improves Emotional Health: Reduces feelings of loss, anxiety, or self-consciousness.
- Natural Appearance: Creates a breast that looks and feels more natural.
- Comfort in Clothing: Makes it easier to wear fitted outfits, bras, and swimwear.
- Long-Lasting Results: Provides permanent restoration with durable results.
- Nipple & Areola Reconstruction: Option to rebuild the nipple and areola for a more complete appearance.
- Enhanced Quality of Life: Improves overall well-being and restores a sense of normalcy.
Side Effects of Breast Reconstruction Surgery
- Pain & Discomfort: Common in the initial weeks after surgery.
- Swelling & Bruising: Usually temporary but can take weeks to settle.
- Scarring: Inevitable, though scars fade over time with proper care.
- Numbness or Sensation Changes: Loss of feeling in the breast or donor site may occur.
- Fatigue: Common during the early recovery phase.
- Drain Care: Temporary drains may cause some inconvenience.
What are the risks of breast reconstruction surgery?
While generally safe, breast reconstruction carries certain risks:
- Infection: As with any surgery, there is a risk of infection at incision sites.
- Implant Complications: Implants may rupture, leak, or cause capsular contracture (hardening of scar tissue around the implant).
- Flap Complications: For tissue-based reconstruction, the transferred tissue may not survive, leading to partial or complete flap loss.
- Bleeding or Blood Clots: Rare but serious risks associated with surgery.
- Asymmetry: Breasts may not be perfectly symmetrical, requiring revision surgery.
- Delayed Healing: More common in smokers, diabetics, or patients with poor circulation.
- Additional Surgeries: Some patients may need further procedures for adjustments or corrections.
Breast Reconstruction Surgery Cost in India
The cost of breast reconstruction surgery in India typically ranges from Rs. 40,000 to Rs. 5,00,000 per breast. The exact price depends on multiple factors, such as:
- Type of Reconstruction: Implant-based (silicone/saline implants) vs. autologous (using patient's own tissue like DIEP or TRAM flap).
- Timing of Surgery: Whether reconstruction is performed immediately after mastectomy or as a delayed procedure.
- Surgeon's Expertise: Highly experienced and specialized plastic surgeons may charge higher fees.
- Hospital Location & Facilities: Premium hospitals in metro cities generally cost more than smaller clinics.
- Additional Procedures: Use of advanced microsurgery, fat grafting, nipple reconstruction, or revision surgeries can increase the overall cost.
- Room Category & Hospital Stay: Private rooms, ICU facilities, and the duration of hospital stay all affect the final billing.
On average, implant-based breast reconstruction is usually more affordable, while flap-based (autologous tissue) reconstruction tends to be on the higher end of the cost range due to its complexity.








































