What is Colporrhaphy?
Colporrhaphy is a surgical procedure aimed at repairing defects in the vaginal walls caused by weakening of the supporting tissues.
This surgery is performed to restore the normal anatomy of the vagina, improve pelvic organ support, and relieve symptoms such as urinary incontinence, pelvic pressure, or discomfort during sexual activity.
Colporrhaphy can involve the anterior (front) or posterior (back) vaginal wall, depending on the type of prolapse.
What is Anterior Colporrhaphy?
Anterior colporrhaphy specifically targets the anterior (front) vaginal wall, which supports the bladder. It is most commonly performed to correct cystocele, a condition where the bladder bulges into the vaginal canal due to weakened connective tissues or muscles.
The goal of anterior colporrhaphy is to restore bladder support, improve urinary function, and relieve pelvic pressure or discomfort.
Anterior Colporrhaphy Surgery Types
Anterior colporrhaphy can be performed using different approaches based on the severity of prolapse and surgeon preference:
- Traditional Anterior Colporrhaphy: The surgeon makes an incision in the anterior vaginal wall, removes or tightens excess tissue, and repairs the underlying supportive muscles to restore bladder support.
- Mesh-Enhanced Anterior Colporrhaphy: In some cases, a synthetic mesh is used to reinforce weakened tissues and reduce the risk of recurrence.
- Minimally Invasive or Laparoscopic Approach: Rarely, a laparoscopic approach may be used for complex cases, allowing smaller incisions and quicker recovery.
Each type is selected based on the patient's needs, the severity of the prolapse, and the surgeon's recommendation, ensuring optimal comfort and recovery.
1 to 2 Hours
Surgery Duration
General/Regional Anesthesia
Anesthesia Used
8 weeks or more
Full Recovery Timeline
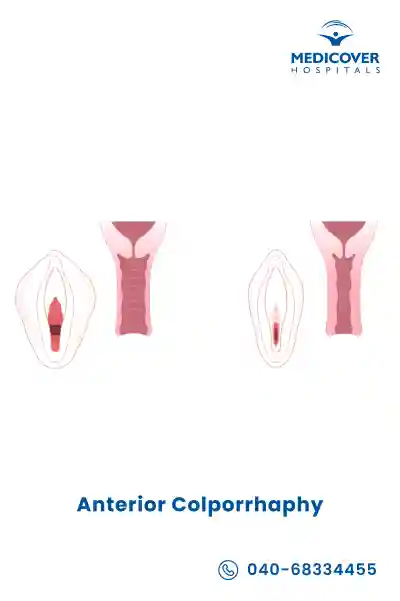
Indications for Anterior Colporrhaphy
Anterior colporrhaphy is recommended for women experiencing symptoms due to anterior vaginal wall prolapse (cystocele) or weakened pelvic support. The main indications include:
- Pelvic Organ Prolapse (POP): When the bladder descends and bulges into the vaginal wall, causing discomfort or functional issues.
- Urinary Incontinence: Weakening of the pelvic floor or bladder support may lead to stress urinary incontinence or difficulty controlling urination.
- Chronic Pelvic Discomfort: Persistent pressure, fullness, or a bulging sensation in the pelvic region affecting daily activities or sexual function.
- Failed Conservative Treatments: Non-surgical options such as pelvic floor exercises, pessaries, or lifestyle modifications have not provided sufficient relief.
- Anatomical Abnormalities: Changes caused by childbirth, aging, or connective tissue weakness that alter bladder or vaginal placement.
Conditions Treated by Anterior Colporrhaphy
- Cystocele (bladder prolapse into the anterior vaginal wall)
- Stress urinary incontinence linked to pelvic floor weakness
- Vaginal bulging or pelvic organ prolapse affects the quality of life
- Recurrent urinary tract symptoms due to bladder displacement
When Would a Doctor Recommend Anterior Colporrhaphy?
A doctor may recommend anterior colporrhaphy when:
- Conservative treatments for pelvic organ prolapse or incontinence fail
- Symptoms interfere with daily life, sexual activity, or bladder function
- The anatomical defect is significant enough to cause persistent discomfort or urinary issues
- There is a risk of progression or complications from untreated prolapse.
How Should I Prepare Before Anterior Colporrhaphy Surgery?
Preparation for anterior colporrhaphy is essential to minimise risks and ensure a smooth recovery. Key steps include:
- Medical Consultation: Meet with your gynaecologist or urogynecologist to review your symptoms, overall health, and suitability for surgery.
- Medication Review: Inform your doctor about all medications, including blood thinners, vitamins, or herbal supplements. Some may need to be paused to reduce surgical risks.
- Lifestyle Adjustments: Stop smoking and limit alcohol intake to promote better healing and reduce surgical complications.
- Personal Preparation: You may be advised to shower with antiseptic soap on the day of surgery to reduce infection risk.
- Support Arrangements: Arrange for someone to drive you home after surgery and assist during the early recovery period.
What Tests Are Done Before Anterior Colporrhaphy Surgery?
Doctors may recommend specific tests to evaluate your condition and overall health before surgery, including:
- Pelvic Examination: To assess the extent of vaginal prolapse (cystocele) and rule out associated prolapse conditions.
- Urinary Tests: To check for infections or bladder dysfunction.
- Blood Tests: To evaluate overall health, blood count, and clotting ability.
- Imaging (if needed): Ultrasound or MRI may be recommended in cases of complex prolapse.
- Cardiac Evaluation (for older patients): ECG or other cardiac tests to ensure fitness for anesthesia.
Should I Stop Eating, Drinking, or Taking Medicines?
- Fasting: You will likely need to fast (avoid food and drinks) for 6-8 hours before surgery to reduce anaesthesia-related risks.
- Medications: Your doctor will provide specific instructions on which medications to stop, such as:
- Blood thinners: Like warfarin, aspirin, clopidogrel. Usually stopped several days before surgery to reduce bleeding risk.
- Diabetes medications: May be adjusted or withheld on the day of surgery.
- Supplements and herbal remedies: Often discontinued due to potential interactions or bleeding risks.
What Happens Before Anterior Colporrhaphy Surgery?
On the day of the procedure, you can expect:
- Hospital Admission: You will be admitted to the hospital and prepared for surgery.
- Anesthesia Consultation: The anesthesiologist will discuss anesthesia options (general or regional).
- IV Line Placement: For fluids and medications.
- Monitoring: Your vital signs (blood pressure, heart rate, oxygen levels) will be checked.
- Final Review: Your surgeon will review the surgical plan, confirm consent, and answer any last-minute questions.
By following these steps and your surgeon's guidance, you ensure a safer and smoother anterior colporrhaphy surgery experience.
Anterior Colporrhaphy Procedure Steps
The anterior colporrhaphy surgery follows a series of carefully planned steps to restore support to the vaginal wall and bladder:
- Anesthesia: The patient receives either general anesthesia, regional anaesthesia, or sedation to minimize discomfort during the procedure.
- Incision: The tissues are cut to allow access to the bladder and the tissue in need of treatment.
- Dissection: The surgeon gently separates the bladder from the vaginal wall and adjacent structures, such as the uterus or rectum.
- Two Key Steps of Bladder Suspension Surgery: Fixing Vaginal Wall, The surgeon tightens the stretched/attenuated vaginal tissues so that the bladder receives the appropriate support again; this tissue will usually be secured with stitches.
- Rehab of the Bladder: The bladder is realigned in its correct anatomical position in case of incomplete bladder rehab to prevent further repletion of the bladder.
- Incision closure: The vaginal incision is closed with absorbable suture, and no stitches on the outside are shown.
- Recovery: The patient is observed in the recovery area after the procedure and may spend a day or two in the hospital.
Anterior colporrhaphy aims to restore normal function of the pelvic structure, reduce symptoms, and improve quality of life.
Who Will Perform the Anterior Colporrhaphy Procedure?
Anterior colporrhaphy is usually performed by gynaecologists, particularly one who specializes in pelvic floor diseases or urogynecology. These professionals are educated to detect and treat pelvic organ prolapse, urine incontinence, and vaginal wall abnormalities.
If urinary problems exist, a urologist may be consulted, particularly if bladder function is impaired. A collaborative approach may be used for comprehensive care, including post-surgery rehabilitation with pelvic floor physical therapists.
Recovery After Anterior Colporrhaphy Surgery
Recovery from anterior colporrhaphy is gradual and requires careful attention to rest, wound care, and activity restrictions.
What should I expect immediately after the procedure?
- Hospital Stay: Most patients remain in the hospital for 1-2 days for monitoring.
- Pain and Swelling: Some pain, swelling, or discomfort in the vaginal area is common. Pain relief medications and ice packs are usually provided.
- Urinary Function: A catheter may be placed temporarily to help with urination.
- Observation: Medical staff will monitor vital signs, incision healing, and urinary output to ensure no immediate complications.
When can I return to normal activities?
- Initial Rest: For the first 2-3 weeks, rest and limited movement are important. Avoid bending, straining, or lifting.
- Activity Restrictions: Heavy lifting, strenuous exercise, and sexual activity should be avoided for at least 6-8 weeks.
- Gradual Return: Light household tasks and walking can typically be resumed within 2-3 weeks, depending on your recovery progress.
- Full Recovery: Most women recover fully within 6-8 weeks, although this may vary depending on age, overall health, and individual healing speed.
Are lifestyle changes required after recovery?
Yes. Certain lifestyle adjustments can help maintain pelvic health and prevent recurrence of prolapse:
- Pelvic Floor Exercises: Regular Kegel exercises strengthen pelvic muscles and provide long-term bladder and vaginal support.
- Weight Management: Maintaining a healthy weight reduces pressure on pelvic structures.
- Dietary Habits: A high-fibre diet and good hydration help prevent constipation and straining.
- Avoid Smoking: Smoking can weaken connective tissues and impair healing.
- Lifting Techniques: Use proper posture and avoid heavy lifting to prevent strain on the pelvic floor.
These changes not only support recovery but also help protect long-term pelvic function and quality of life.
What are the Benefits of Anterior Colporrhaphy Surgery?
- Restores Pelvic Anatomy: The procedure corrects bladder prolapse (cystocele) and strengthens the anterior vaginal wall, restoring normal anatomical structure.
- Improves Urinary Function: Resolves urinary incontinence or difficulty urinating caused by bladder descent or weakness of pelvic support.
- Reduces Pelvic Discomfort: Alleviates symptoms such as pelvic pressure, vaginal bulging, and the sensation of fullness, improving overall comfort.
- Improves Sexual Function: Repair of prolapse often enhances comfort and function during sexual intercourse, improving intimacy and quality of life.
- Minimally Invasive Option: Performed vaginally with dissolvable sutures, which avoids large external incisions and promotes faster recovery compared to abdominal surgeries.
- Long-Term Symptom Relief: Provides a durable solution for pelvic organ prolapse when conservative treatments (pelvic exercises, pessaries) are ineffective.
- Improves Quality of Life: Reduces the psychological and physical burden of prolapse symptoms, helping patients return to daily activities without discomfort or embarrassment.
What are the Risks or Complications of Anterior Colporrhaphy Surgery?
Anterior Colporrhaphy is a surgical procedure performed to repair the anterior (front) vaginal wall, commonly done to correct cystocele (bladder prolapse). While it is generally safe, like any surgery, there are potential risks and complications. Here are the common risks associated with anterior colporrhaphy:
- Infection: Infections at the incision site or in the pelvic area are a potential risk. Post-surgical care, including keeping the area clean and following medical instructions, helps minimize this risk.
- Bleeding: Some bleeding during or after surgery is expected. However, excessive bleeding can lead to complications and may require further medical intervention or a blood transfusion.
- Urinary Issues: Urinary retention (difficulty urinating) or urinary incontinence (leakage of urine) are possible. These issues may resolve over time, but can sometimes require additional treatments.
- Injury to Surrounding Organs: Accidental injury to nearby organs, such as the bladder, urethra, or rectum, is a risk during surgery. Any damage may require additional surgical repair or long-term care.
- Vaginal Stenosis or Scarring: Scarring or narrowing of the vaginal canal (vaginal stenosis) can occur, potentially causing discomfort or difficulty with sexual intercourse. This complication may require further intervention.
- Blood Clots: Deep vein thrombosis (DVT) or blood clots, particularly in the legs, are a potential risk after any surgery. Early mobilization and preventive measures reduce this risk.
- Recurrence of Prolapse: The repaired prolapse may return over time. In some cases, the procedure may need to be repeated if the prolapse recurs.
- Pelvic Pain or Discomfort: Pain and discomfort in the pelvic area after surgery are common but typically resolve over time. Chronic pelvic pain can develop if complications arise.
- Sexual Dysfunction: Post-surgical changes to vaginal anatomy, such as scarring or narrowing of the vaginal wall, may affect sexual function and cause pain during intercourse.
- Anesthesia Risks: As with any procedure involving anesthesia, there is a risk of allergic reactions or complications, though these are rare.
- Bowel or Rectal Injury: Injury to the bowel or rectum, while rare, is a potential risk, especially if the posterior vaginal wall is also involved in surgery or the pelvic area is very distorted.
Anterior Colporrhaphy Surgery Cost
The cost of Anterior Colporrhaphy surgery can vary depending on the hospital, the surgeon's experience, the type of procedure, and your specific medical needs. On average, the surgery in India can range from Rs. 45,000 to Rs. 1,50,000.





















































































