Gastroparesis: Causes, Symptoms, and Treatments
Written by Medicover Team and Medically Reviewed by Dr P Abdul Samad , Gastroenterologists Medical
Gastroparesis is a medical condition that impacts passage of food from the stomach to the small intestine. It occurs when the stomach's normally occurring contractions fail to work properly. It is also known as gastric paralysis.
Stomach contractions assist in the passage of partly digested food from the stomach to the small intestine. Further digestion and nutrient absorption takes place here.
For those suffering with gastroparesis, this process does not function properly, affecting the condition of the empty stomach. The condition may include nausea, vomiting, blood sugar fluctuations, and poor nutrition.
What Are the Common Causes and Risk Factors of Gastroparesis?
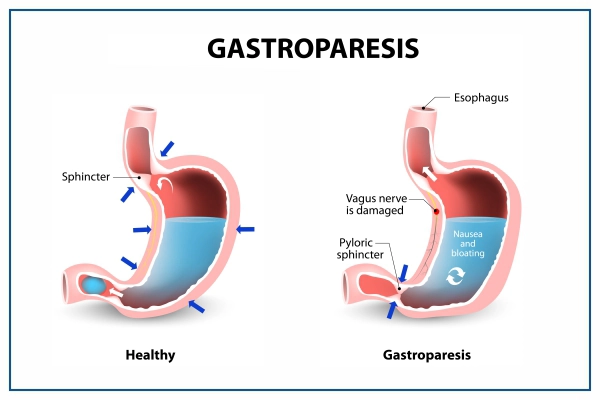
The exact cause of gastroparesis is not fully understood. In many cases, it is linked to damage to the vagus nerve, which controls stomach muscle movement.
The vagus nerve helps regulate complex digestive processes, including signaling the stomach muscles to contract and push food into the small intestine. When this nerve is damaged, food stays in the stomach longer, delaying digestion and nutrient absorption.
Common causes of vagus nerve damage include:
- Diabetes (especially poorly controlled blood sugar)
- Surgery involving the stomach or small intestine
- Infections or inflammation affecting the nervous system
Risk Factors
Risk increases with:
- Hypothyroidism
- Abdominal or oesophagal surgery
- Certain medications, including some antidepressants and narcotics
- Scleroderma
- Nervous system disorders, like MS or Parkinson's.
- Women are more prone than men to develop gastroparesis
Get a second opinion from trusted experts and makeconfident, informed decisions.
Get Second OpinionWhat are the Symptoms of Gastroparesis and Warning Signs?
Gastroparesis often causes many nonspecific symptoms. A gastroenterologist needs to make a diagnosis. Common symptoms of gastroparesis include:
- Bloating
- Nausea
- Abdominal pain
- Feeling full after eating small amounts
- Poor appetite
- Acid reflux
- Weight loss
- Malnutrition
Severe Symptoms
- Vomiting undigested food
- Fluctuations in blood sugar levels
- Severe dehydration
- Persistent nausea and vomiting
- Formation of solid food masses (bezoars)
How is Gastroparesis Diagnosed?
Your doctor will inquire about the symptoms and medical history. They will also conduct a physical examination. They may order tests such as:
- Radioisotope stomach-emptying scan (gastric scintigraphy): You'll be given food containing a small amount of safe radiation. After eating, you'll lie under a scanner. If over 10% of the food remains in your stomach after 4 hours, it may suggest gastroparesis.
- Blood tests: Detect dehydration, malnutrition, infection, and blood sugar issues.
- Barium X-ray: You will be given a liquid (barium) to swallow, which will cover your oesophagus, stomach, and small intestine and appear on an X-ray. This is also part of an upper GI (gastrointestinal) series.
- Gastric manometry: It is a procedure in which the doctor inserts a tiny tube into the mouth and the stomach to measure electrical and muscle activity and the rate at which people digest.
- Electrogastrography: It uses electrodes on the skin to assess the stomach's electrical activity.
- Ultrasound imaging: Employs sound waves to create images of the organs. The doctor may use it to rule out other conditions.
What Are the Treatment Options for Gastroparesis?
The first step in gastroparesis treatment is identifying and addressing the underlying cause. If gastroparesis is caused by diabetes, controlling blood sugar levels is typically the initial step in treating gastroparesis patients.
- Gastroparesis treatment diet: It consists of eating small, nutritious meals, including foods low in fibre and fat, easily digestible food and well-cooked vegetables. You must avoid carbonated beverages and alcohol. Drinking lots of water and liquids such as fruit and vegetable juices will help manage your condition.
- Natural therapy for gastroparesis: It includes consuming probiotics, yoghurt, liquid nutritional supplements, and avoiding constipation. Ginger is a classic natural nausea remedy. Acupuncture and deep relaxation techniques have been known to alleviate the symptoms of gastroparesis.
- Medication for gastroparesis: Promethazine and Metoclopramide are used to relieve nausea and vomiting. Erythromycin, an antibiotic, also helps the stomach muscles to contract and drive food out of the stomach.
- Gastroparesis pain relief: Nonsteroidal anti-inflammatory drugs (NSAIDs) and tricyclic antidepressant medications may help alleviate gastroparesis symptoms.
- Quitting smoking and drinking alcohol: In your daily routine, including modest physical exercises such as walking after eating, and avoiding lying down within three hours of consuming food, may show some improvement.
- Intravenous nutrition: Nutrients are delivered directly into the circulation via a catheter inserted into a vein.
- Jejunostomy tube: Bypassing the stomach, a tube is introduced into the small intestine through the abdomen. This provides nutrition straight to the small intestine.
- Electrical gastric stimulation: This therapy uses electric pulses to stimulate the nerves and soothe stomach muscles to increase contractions.
- Gastroparesis surgery: While partial or total gastrectomy may temporarily relieve certain symptoms of gastroparesis, it has serious long-term consequences.
Home Remedies for Gastroparesis
Dietary changes and home remedies can be managed effectively. Simple adjustments, such as modifying diet and utilizing home remedies for pain, offer practical relief as shown below:
- Consuming cooked vegetables over raw vegetables
- Chewing food thoroughly
- Avoiding high-fiber foods and fruits, such as broccoli and oranges
- Avoiding consumption of greasy meals as these can slow down digestion
- Consuming smaller meals. (Instead of three meals each day, eat five or six smaller meals throughout the day)
- If fluids are easier to swallow, soften the meals or consume soup
- Drinking lots of water on a daily basis (1 to 1.5 liters)
- Walking after consuming meals
- Avoiding alcohol, smoking, and carbonated beverages
- Trying not to sleep after 2 hours of eating
- Taking a multivitamin every day
When Should You See a Doctor for Gastroparesis?
It's important not to ignore the signs your body is giving you. Early treatment can help manage gastroparesis better and avoid unnecessary health problems.
Symptoms That Last Too Long
- If you're having nausea, vomiting, stomach bloating, or feeling full too soon for more than a week, it's better to get it checked.
- Sudden weight loss or loss of appetite is also a strong reason to visit a doctor.
Symptoms Getting Worse
- Vomiting food that was eaten several hours back
- Stomach pain or heavy bloating
- Not able to eat or drink properly
- Feeling weak, tired, or signs of dehydration
These may be signs of severe gastroparesis or other issues like malnutrition.
Who Should Be Extra Careful
- Diabetic patients (especially with Type 1) it can affect sugar levels
- People who had recent stomach or food pipe surgery
- Senior citizens or those with nervous system problems like Parkinson's
- Those already dealing with digestive or autoimmune issues
Your health is everything - prioritize your well-being today.
What Is the Recovery Process After Gastroparesis Treatment?
Recovering from gastroparesis takes time, and it depends a lot on how well you follow the treatment and daily care advised by your doctor. Medicines can help control symptoms, but lifestyle changes play a big role in your long-term comfort.
Follow-Up and Check-Ups
- After starting treatment, regular follow-ups with your gastroenterologist are very important.
- If you are a diabetic, you may need more frequent checks to manage your blood sugar levels better.
- In some cases, tests like gastric emptying scans may be repeated to see how well your stomach is functioning.
Lifestyle & Diet Recommendations
To manage gastroparesis well, small changes in your daily habits can go a long way:
- Eat 5 to 6 small meals a day instead of 2 or 3 large ones.
- Always prefer cooked vegetables over raw ones, they are easier to digest.
- Avoid high-fibre items like broccoli, cabbage, and oranges.
- Stay away from fried or oily foods, as they slow down digestion.
- Drink 1 to 1.5 litres of water daily, mostly between meals.
- If you're finding it hard to eat solids, go for soups or soft foods.
- Chew your food well and eat slowly.
- Take a short walk after meals to help with digestion.
- Don't lie down for at least 2 hours after eating.
- Avoid smoking, alcohol, and carbonated drinks.
- Take a daily multivitamin if your doctor recommends it, especially if you're not getting enough nutrients through food.
Long-Term Outlook
With proper treatment, many patients are able to manage their symptoms and lead a near-normal life. Some may have occasional flare-ups, but regular care and sticking to lifestyle changes can make a big difference.
What Precautions Can Help Prevent Gastroparesis?
Preventing gastroparesis mainly involves lifestyle changes and regular health check-ups, especially if you are at risk.
Prevention
- Control blood sugar levels carefully if you have diabetes.
- Eat small, frequent meals with cooked vegetables; avoid greasy and high-fibre foods.
- Avoid smoking, alcohol, and carbonated drinks.
- Take a short walk after meals and avoid lying down immediately.
- Chew food thoroughly to aid digestion.
- Get regular screenings if you have diabetes or other risk factors.
Complications
Gastroparesis can have a negative impact on your health and decrease the overall quality of life. Complications may include the following:
- Excessive vomiting: This may lead to severe dehydration, which can even be fatal
- Reduced Appetitie: You may have reduced appetite or vomiting that prevents you from receiving adequate nutrients
- Fermation of food in the stomach: Foods that remain in the stomach for too long can ferment, causing germs to develop
- Formation of Bezoars: These are solid masses that may be formed in the stomach due to undigested food
- Nausea: Complications can induce nausea and vomiting, and if they block the passage between the stomach and small intestine, these can be fatal as well
- Abnormal blood sugar levels: This may prevent you from absorbing enough nutrients.
Dos and Don'ts
For those suffering from gastroparesis, the stomach does not drain as fast as it should. The doctor may refer to this as delayed gastric emptying. It can make you feel ill or even vomit. After eating a tiny amount of food, the stomach may ache or appear quite full. This might make it difficult to eat adequate calories, vitamins, and minerals. Following the below mentioned dos and don'ts can help you avoid the negative consequences of gastroparesis:
|
Do's |
Don'ts |
|
Avoid or reduce alcohol and smoking |
Eat high starchy & greasy or fried foods |
|
Engage in regular physical activity |
Drink soda drinks |
|
Keep yourself hydrated |
Drink alcoholic beverages |
|
Eat frequent, small meals that are low in fat and fibre |
Lay down immediately after eating food |
|
Take the medicines as prescribed by the doctor |
Discontinue medicines without completing the dosage |
Precautions and self-care will help you fight this condition positively and improve your quality of life.
Gastroparesis Care at Medicover Hospitals
At Medicover, we have the best team of gastroenterologists and surgeons who work together to provide Gastroparesis disease treatment with utmost precision. Our highly skilled team utilises the latest medical equipment, diagnostic procedures, and technologies to treat various Gastroparesis conditions and ailments.
For treating Gastroparesis, we adopt a multi-disciplinary approach to provide porper care to the patients and attend to all their medical needs for faster and sustained recovery.