| Do’s | Don’ts |
|---|---|
|
Eat plenty of fruits and vegetables in the diet. |
Include lots of saturated fat in your diet. |
|
Drink plenty of water, |
Smoke. |
|
Take the medicines prescribed by the doctor. |
Discontinue medicines without completing the course. |
|
Keep a positive attitude, strong will and determination. |
Be hard on the circumstances. |
|
Consume hot and cold foods separately, |
Eat too many sugary foods and drinks. |
Multiple Sclerosis: Types, Causes, Prevention and Diagnosis
Multiple Sclerosis (MS) is a chronic illness that affects the central nervous system (CNS), which includes the brain and spinal cord. It happens when the immune system mistakenly attacks the protective covering of nerve fibres, called myelin, leading to inflammation and damage. This disrupts the normal transmission of electrical signals between the brain and the rest of the body, causing a range of neurological symptoms.
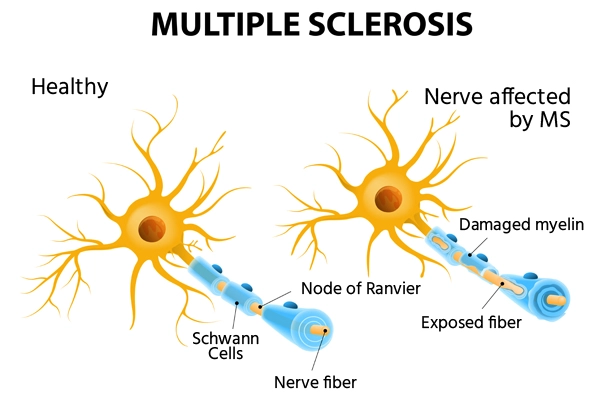
Types of Multiple Sclerosis
Multiple Sclerosis (MS) has several types, each with its own pattern of symptoms and progression. The main types of MS are:
Relapsing-Remitting MS (RRMS)
- Most common type.
- It has periods of new or worsening symptoms (relapses), followed by times of recovery (remissions).
- There is no progression of disability during remission.
Secondary Progressive MS (SPMS)
- Starts as RRMS, but later it progresses steadily with or without occasional relapses.
- Disability keeps increasing, but relapses may still happen in some cases.
Primary Progressive MS (PPMS)
- There is a gradual worsening of symptoms from the beginning, without clear relapses or remissions.
- The disability progresses steadily, though the rate of worsening can vary.
Progressive-Relapsing MS (PRMS)
- This is a rare form of MS.
- It involves a steady worsening of symptoms from the start, with occasional relapses that may cause more damage or disability.
- There are no periods of remission.
Get a second opinion from trusted experts and makeconfident, informed decisions.
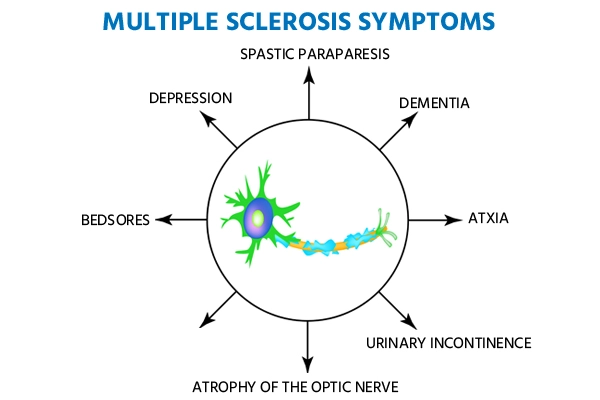
Symptoms of Multiple Sclerosis
The symptoms of Multiple Sclerosis (MS) can vary widely depending on where the nerve damage occurs and how severe it is. They also differ from person to person and can come and go, or gradually worsen over time. Here are the most common multiple sclerosis symptoms:
- Fatigue: Extreme tiredness that affects daily activities.
- Numbness or Weakness: Usually in the limbs, making movement or balance difficult.
- Vision Problems: Blurry or double vision, or even partial loss of vision, often due to inflammation of the optic nerve ( optic neuritis).
- Muscle Spasms or Stiffness: Sudden tightness or rigidity, especially in the legs.
- Walking Difficulties: Problems with coordination and balance, which can make walking hard.
- Cognitive Changes: Difficulty with memory, concentration, and problem-solving.
- Pain: Sensations like burning or stabbing pain, often in the back or legs.
- Bladder and Bowel Problems: Urgent need to urinate, incontinence, or constipation due to nerve damage.
- Dizziness or Vertigo: A feeling of spinning or light-headedness, often linked to balance issues.
Causes of Multiple Sclerosis
Multiple sclerosis causes are unknown to experts. According to research, the following factors may increase the chance of getting MS:
- Immune system dysfunction: Being an autoimmune disease, the immune system in ms attacks on its own instead of attacking pathogens it attacks on protection covering around your nerve fibres in CNS. This leads to inflammation and injury, interfering with normal nerve function.
- Genetic Predisposition: Although not directly inherited, there is a genetic component to MS. If someone has a close relative with multiple sclerosis, the risk is slightly increased, suggesting the possibility of some genetic factors which make the individual more prone to developing it.
- Environmental Influences: Environmental factors can contribute to the onset of MS in genetically predisposed individuals. These include:
- Vitamin D Insufficiency: Low serum levels of 25-hydroxyvitamin D (VDD) have been associated with a significantly increased risk of MS, especially when exposure in childhood.
- Infections: Certain viral infections, primarily the Epstein-Barr virus (the virus that causes mononucleosis), are thought to contribute to MS risk.
- Geography: People living farther from the equator have a higher risk for MS, likely due to lower sunlight exposure and lower vitamin D levels, which indicates an environmental cause.
- Gender: MS is more prevalent in women than in men, with women being two to three times more likely to have the disease.
- Age: MS usually develops in people aged 20-40, although it can present at any age.
When to see a doctor?
If a doctor says you have multiple sclerosis, consider seeing an MS specialist, or neurologist, for a second opinion. People should consider the diagnosis of MS if they have one or more of these symptoms:
- Vision loss in one or both eyes
- Acute paralysis in the legs or along one side of the body
- Acute numbness and tingling in a limb
- Imbalance
- Double vision
Confirming the diagnosis is an important step for a disease that depends on a strong long-term relationship between a patient, family members and a medical team to monitor and manage the disease.
Get the best treatment for Multiple Sclerosis from our Neurologists at Medicover Hospitals.
Complications of Multiple Sclerosis
Multiple Sclerosis (MS) is a chronic disease that life-threatening complications may develop in their stages according to severity and data on clinical progression of disease. Common complications are as follows:
- Mobility Challenges: MS may cause muscle weakness, spasticity (muscle stiffness) and coordination and balance problems, making it difficult to walk or move without assistance.
- Vision Problems: Damage to the optic nerve can cause blurry vision, double vision, or even partial loss of sight. There are some people with MS who may develop permanent vision issues.
- Cognitive Changes: MS can impact memory, focus, problem-solving, and other cognitive functions. It can affect day affairs and work as well.
- Bladder and Bowel Problems: Many patients with MS have urinary urgency, incontinence, or problems emptying the bladder. Constipation and issues with bowel control are also common.
- Sexual Dysfunction: Because MS impacts nerve transmission, it can hinder sexual function, resulting in a decreased libido, erectile dysfunction in men, or difficulty achieving orgasms in both sexes.
- Fear and Stress: Chronic illness and the uncertainty of the disease process can contribute to mental health problems including depression, anxiety, and mood instability.
- Difficulty Speaking or Swallowing: Because MS affects the nervous system, it can sometimes cause a person to have difficulty speaking clearly or swallowing, which can present a choking hazard.
- Breathing Problems: In severe cases, MS may involve the muscles used in breathing, resulting in difficulty breathing.
Prevention of Multiple Sclerosis
Scientists, researchers, and doctors haven’t yet been able to develop a method of curing or preventing MS. One of the main reasons is that MS's cause isn’t fully understood. Experts believe a combination of genetic and environmental factors contributes to the development of MS. Identifying these factors might one day help pinpoint the cause of the disease. This can open the door to developing treatments and prevention options.
Diagnosis of Multiple Sclerosis
Diagnosis of Multiple Sclerosis (MS) requires a detailed medical history, physical exam, and tests to eliminate other causes. The first step in the Multiple Sclerosis diagnosis process is to evaluate symptoms such as numbness, weakness, vision difficulties, balance challenges, and cognitive changes that arise in episodes or relapses. The following are the key steps in diagnosing MS:
- Clinical History and Symptoms: The doctor will ask about symptoms and try to identify patterns that point to MS, like the recurrence of neurological problems.
- Neurological Examination: The physician will test motor skills, coordination, reflexes, and sensory perception to find any irregularities that could indicate MS.
- MRI (Magnetic Resonance Imaging): MRI is a golden advantage for diagnosis of Multiple Sclerosis. It aids in identifying lesions or plaques in the brain and spinal cord, which are typical of MS.
- Lumbar Puncture (Spinal Tap): This process includes taking a sample of your cerebrospinal fluid to look for certain changes, such as the presence of oligoclonal bands, which are often found in multiple sclerosis patients.
- Evoked Potentials test: In this test, the patient's brain electrical activity is measured in response to stimuli, which may indicate nerve damage related to MS.
- Blood Tests: To exclude other conditions that may appear as NS, but not specific blood tests exist for MS.
Treatment for Multiple Sclerosis (MS)
Treatment for Multiple Sclerosis (MS) focuses on managing symptoms, reducing relapse frequency, and slowing down the progression of the disease. While MS doesn't have a cure, there are several treatment options that can help improve the quality of life for those affected. Here are the available Multiple Sclerosis treatment options:
- Disease-Modifying Therapies (DMTs): These medications aim to reduce the frequency and severity of relapses and slow the progression of MS. They work by modulating the immune system and preventing it from attacking the nervous system.
- Steroids (Corticosteroids): These are used during relapses to reduce inflammation and speed up recovery. They help manage flare-ups but don't affect long-term disease progression.
- Symptomatic Treatments: These treatments focus on managing specific symptoms of MS, such as muscle spasticity, pain, fatigue, depression, and bladder or bowel issues. Medications, physical therapy, and lifestyle changes are part of this approach.
- Physical Therapy and Rehabilitation: MS can cause muscle weakness and coordination problems. Physical therapy helps improve mobility, strength, and balance, while rehabilitation services help with issues like speech and swallowing difficulties.
- Plasma Exchange (Plasmapheresis): In severe cases where symptoms don't improve with steroids, plasma exchange may be recommended to remove harmful antibodies from the blood.
Lifestyle Changes and Selfcare
Managing Multiple Sclerosis (MS) also requires lifestyle changes and self-care. These approaches can help alleviate symptoms, enhance overall functioning, and preserve independence. Here are several lifestyle changes and self-care tips for those living with MS:
- Regular Physical Activity: Engaging in fitness activities increase strength, mobility and stability. Gentle activities such as walking, swimming or yoga can also improve flexibility and reduce fatigue. If you want to do some kind of exercise, it's best to talk to a physiotherapist to work out a safe and suitable exercise plan for you.
- Heart-Healthy Nutrition: A heart-healthy diet is rich in fruits and vegetables (whole fruits are preferred over juices), whole grains, lean protein, plant-based protein and healthy fats. Foods such as salmon, which are rich in omega-3 fatty acids, may help reduce inflammation. Staying hydrated and cutting back on salt and processed foods are also important.
- Stress Management: Stress can worsen the symptoms of MS. Employing relaxation strategies, including breathing exercises and meditation, mindfulness practices and certain pastimes like reading and music can also help beat back stress.
- Adequate Rest and Sleep: Fatigue is one of the symptoms of MS, so proper rest and sleep is important. And adopting a sleep schedule and trying to correct sleep issues like insomnia will help raise energy levels.
- Mobility Aids: Canes, walkers, or wheelchairs can assist with mobility and help prevent falls. With your doctor’s advice, you can also work with an occupational therapist, who can recommend everything from home modifications to assistive devices that enhance your activities of daily living.
Your health is everything - prioritize your well-being today.
Do’s And Don’ts With Multiple Sclerosis
Living with multiple sclerosis is a challenge and it requires a set of dos and don’ts to be followed. Take care of yourself, stay informed and seek medical care on time to further manage this condition.
Awareness and self-care will help you fight the condition positively and improve your quality of life.
Multiple Sclerosis Treatment at Medicover
At Medicover, we have the best team of Neurologists and Neurosurgeons who work together to provide Multiple Sclerosis treatment with utmost precision. Our highly skilled team utilises the latest medical equipment, diagnostic procedures and technologies to treat various neurological diseases and ailments. For Multiple Sclerosis, we adopt a multi-disciplinary approach to provide comprehensive care to the patients and attend to all their medical needs at once for faster and sustained recovery.
Frequently Asked Questions
What is the main cause of multiple sclerosis?
The exact cause of MS is unknown, but it's believed to be an autoimmune disorder where the immune system attacks the protective covering of nerve fibers in the central nervous system.
Can you live a normal life with MS?
Yes, many people with MS can live a normal life with proper treatment, lifestyle changes, and symptom management. However, the course of the disease varies from person to person.
What age does MS start?
MS commonly starts between the ages of 20 and 40, but it can develop at any age, including in children or older adults.
Who is at high risk for MS?
Individuals at higher risk for MS include those with a family history of the disease, women, people of Northern European descent, and those with certain genetic factors.
Can stress cause MS?
Stress does not cause MS, but it can trigger or worsen symptoms in people already diagnosed with the condition.
What causes multiple sclerosis in females?
The exact cause is unclear, but hormonal differences, genetic factors, and immune system dysfunction are believed to contribute to a higher prevalence of MS in females.
What are the Multiple sclerosis symptoms in females?
Symptoms in females are similar to those in males and may include fatigue, numbness, vision problems, muscle weakness, difficulty walking, and cognitive changes. Women may also experience more relapses or flare-ups.