Pericarditis: Symptoms, Causes & Treatment
Written by Medicover Team and Medically Reviewed by Dr S. Srikar Samir Nandan , Cardiologist
If you are feeling a sudden chest pain in your heart that gets bad and worse when you lie down or breathe in, it could be pericarditis. This happens when the lining around your heart gets inflamed. It often starts after a viral illness or surgery and can make you feel tired, short of breath, or uncomfortable in your chest.
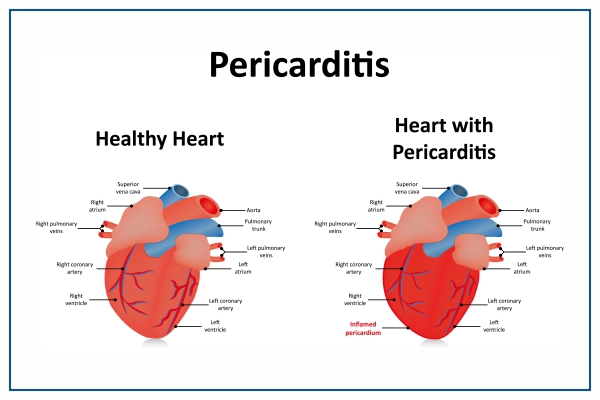
What is Pericarditis?
Pericarditis also known as post-cardiac injury syndrome or post-myocardial infarction syndrome can affect anyone, but it is more common in people who have had recent infections, injuries, or heart procedures.
In some cases, it may come back more than once, which is known as recurrent pericarditis. Though not always serious, ignoring the signs can lead to complications like fluid buildup around the heart.
Along with chest pain, some people may experience a mild fever, a dry cough, or feel generally unwell. The symptoms may vary from person to person and can last for a few days or even weeks. Getting checked by a doctor is important to confirm the condition and start the right treatment early.
What are the Types of Pericarditis?
Pericarditis means swelling of the thin sac that covers the heart. This can happen due to infections, problems with the immune system, or an injury. There are different types of pericarditis, depending on how long it lasts and what causes it:
- Acute Pericarditis: Acute Pericarditis starts suddenly and may be caused by an infection, injury, or immune system problem.
- Chronic Pericarditis: This lasts for more than three months and may be linked to long-term diseases like tuberculosis or immune conditions.
- Recurrent Pericarditis: This means the symptoms go away but then come back again after some time.
- Constrictive Pericarditis: In this type, the sac becomes thick and hard, making it harder for the heart to work normally.
- Uremic Pericarditis: This happens in people with kidney failure. The entire body waste builds up in the body leading to swelling of the body with abnormal smell.
What Causes Pericarditis?
Pericarditis can happen for many reasons. It often starts when the body reacts to an illness, injury, or other health problems. Here are the most common causes and risk factors:
- Heart Attack or Heart Surgery: After damage to the heart, the body's immune system may cause swelling around the heart. This is also called Dressler syndrome.
- Viral Infections: Viruses like COVID-19 and other flu-like infections can lead to pericarditis.
- Injury to the Chest or Heart: A strong hit or injury can irritate the sac around the heart.
- Cancer and Radiation Therapy: Some cancers and cancer treatments like radiation can cause pericarditis.
It is important to treat the cause early to avoid complications and protect heart health.
Get a second opinion from trusted experts and makeconfident, informed decisions.
Get Second OpinionWhat are the Symptoms of Pericarditis?
Pericarditis often begins with chest pain that may feel sharp or stabbing. In some cases, the pain can feel dull or like pressure. It is usually felt behind the breastbone or on the left side of the chest and may spread to the neck, shoulder, or back.
Pericarditis Mild Symptoms
- Sharp or stabbing chest pain
- Feeling tired or weak
- Mild fever
- Dry cough
- Shortness of breath when lying flat
- Pain in the upper belly or under the ribs
- Swelling in the legs or ankles
Severe Symptoms of post-cardiac injury syndrome
- Mild Chest pain that feels like a heart attack
- Difficulty breathing even while sitting
- Fast or irregular heartbeat (palpitations)
- Fainting or dizziness
- Swelling in the abdomen
- Chest pain that does not go away with rest
How Pericarditis is Diagnosed?
To find out if you have pericarditis, the doctor will first talk to you about your symptoms and medical history. A physical examination is done by placing a stethoscope on your chest or back.
To confirm the diagnosis and understand how severe the condition is, your doctor may recommend the following tests:
Common Diagnostic Tests for Pericarditis
- Blood Tests: This test helps detect inflammation, or a heart attack.
- Acute Pericarditis ECG: A quick, painless test that tracks the heart's electrical activity using sticky patches placed on the skin.
- Chest X-ray: This helps identify changes in heart size or shape and may show if the heart is enlarged.
- Echocardiogram: Uses sound waves to create images of the heart. It shows how well the heart is pumping and checks for fluid around the heart.
- CT Scan (Cardiac CT): Gives detailed images of the heart and chest. It helps detect thickening of the heart covering, which may suggest constrictive pericarditis.
- Cardiac MRI: Tested with magnetic field and radio waves to produce detailed heart images. It can detect inflammation, thickening, or other changes in the pericardium.
If you have pericarditis, the doctor may hear a special sound called a pericardial rub, caused by the inflamed layers of the heart sac rubbing against each other.
What are the Treatment Options for Pericarditis?
Treatment for pericarditis depends on what caused it and how severe the symptoms are. In mild cases, especially acute pericarditis, symptoms may go away on their own with rest.
Medications for Pericarditis
- Anti-inflammatory drugs: Medicines like ibuprofen or aspirin are commonly used to reduce pain and swelling.
- Colchicine: This medication helps lower inflammation and reduce the chance of the pericarditis coming back.
- Corticosteroids: These are used in more severe cases or when other medicines do not work well.
- Azathioprine or other immune-suppressing drugs: These may be used for refractory pericarditis, where the condition does not improve with usual treatments.
It is important to avoid heavy physical activity for 1 to 3 weeks to help the body heal and reduce strain on the heart.
Surgical Procedures for Pericarditis
In some cases, fluid builds up around the heart and needs to be drained. Surgery or other medical procedures may be required:
- Pericardiocentesis: A thin, sterile needle or tube is inserted into the chest to remove extra fluid from the pericardial space. This helps relieve pressure on the heart.
- Pericardiectomy: If the pericardium becomes thick and stiff due to constrictive pericarditis, surgery may be needed to remove all or part of the sac to allow the heart to move freely.
When to See a Pericarditis Doctor?
If you are feeling chest pain that lasts more than a few hours or gets worse when lying down or breathing deeply, it is important to see a heart specialist. Pericarditis symptoms, if ignored, can lead to serious heart problems.
You should see a doctor if
- Chest pain lasts for more than 24 hours
- You feel short of breath, especially when lying down
- You have an irregular or fast heartbeat
- You notice swelling in your legs, feet, or stomach
- You feel lightheaded or faint
- You have a fever with chest discomfort
High-Risk Groups Needing Prompt Care
- People with a history of heart disease or recent heart surgery
- Those with chronic kidney problems or undergoing dialysis
- Cancer patients who had radiation therapy near the chest
Getting early care from a pericarditis doctor can prevent complications such as fluid buildup around the heart or chronic pericarditis. Do not wait if you feel something is wrong. Trust your symptoms and consult a specialist at the right time.
Your health is everything - prioritize your well-being today.
What is the Recovery Process After Pericarditis Treatment?
Recovery from pericarditis depends on the type and severity of the condition. Most people with acute pericarditis start to feel better within a few days to weeks, especially with the right medications and rest. However, regular follow-up with a heart specialist is important to make sure the inflammation does not come back.
Follow-Up Care
- Visit your doctor as advised, usually within 1 to 2 weeks after starting treatment.
- Follow-up tests like ECG or echocardiogram may be done to check healing.
- If you have fluid buildup around your heart, more frequent check-ups may be needed.
- Patients with recurrent or chronic pericarditis may need long-term care with regular monitoring.
What Precautions Can Help Prevent Pericarditis?
You may not always be able to stop pericarditis from happening, but some habits can help reduce the risk and support your heart health. Taking care of your body, avoiding infections, and following medical advice are key steps.
Prevention Tips
- Eat Healthy: Choose more fruits, vegetables, and whole grains. Avoid too much salt or oily food.
- Rest After Illness: Give your body time to heal after viral infections or heart problems.
- Avoid Heavy Exercise: Do not do hard workouts or sports if you feel chest pain or are recovering from pericarditis.
- Treat Infections Early: Get treatment if you have a cold, fever, or flu to prevent it from affecting your heart.
- Follow Doctor's Advice: Take medicines exactly as prescribed. Go for regular check-ups, especially if you have kidney disease or immune conditions.
Self-Care During Recovery
- Rest as much as needed
- Take pain relief only after asking your doctor
- Avoid stress and try deep breathing to relax
- Ask your doctor when it's safe to return to normal activities
Pericarditis Complications If Not Treated
If pericarditis is ignored, it can lead to:
- Fluid around the heart (called pericardial effusion)
- Stiff heart lining (called constrictive pericarditis)
- Repeat episodes, making recovery longer
Dos and Don'ts
This condition requires proper treatment along with a clear set of dos and don'ts to manage its symptoms and prevent related infections.
Even after the treatment, it's important to stay alert and follow these guidelines to ensure better management and recovery.
| Do's | Don'ts |
|---|---|
|
|
Follow these precautions and immediately consult your doctor if you notice any new symptoms or worsening of pain.
Our Experience in Treating Pericarditis
Pericarditis can be a painful and scary experience. The chest pain, shortness of breath, and constant discomfort can make everyday activities difficult. It often leaves people worried, especially when symptoms feel like a heart attack.
At Medicover Hospitals, our experienced heart specialists understand how distressing this condition can be. We use advanced tests to diagnose pericarditis early and start the right treatment without delay. Our team follows proven methods, combining medications and care plans that suit your condition and recovery needs.
From the first visit to your complete recovery, Medicover stays with you every step of the way. We offer continuous support, regular follow-ups, and a caring environment to help you heal comfortably. Your heart health is our priority, and we are here to help you feel safe and supported throughout your pericarditis journey.