What is Thyroidectomy (Thyroid Surgery)?
Thyroidectomy is a surgery where either part or the entire thyroid gland is excised. The thyroid is a tiny gland bearing a butterfly shape, situated in the neck and is very important in controlling the metabolism, body temperature and levels of energy.
This surgery may be recommended for patients with thyroid cancer, large goitres, suspicious nodules, or hyperthyroidism that does not respond to medication. Depending on the severity of the condition, your surgeon may remove a portion of the gland or the entire thyroid.
Types of Thyroidectomy
Types include total thyroidectomy, partial (subtotal) thyroidectomy, and lobectomy, depending on the condition and extent of removal.
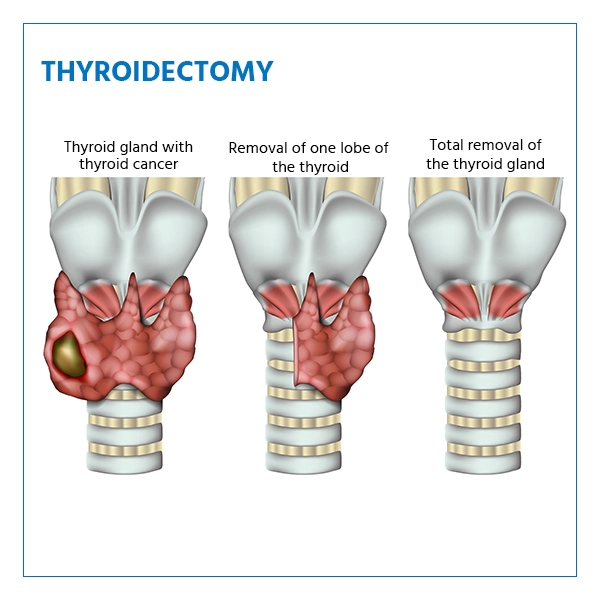
- Total Thyroidectomy: In this surgery, the entire thyroid gland is removed. It is usually recommended for patients with thyroid cancer, large goitres, or severe hyperthyroidism. After this procedure, patients will require lifelong thyroid hormone replacement therapy to maintain normal body functions.
- Subtotal (Partial) Thyroidectomy: In this approach, only a part of the thyroid gland is removed, leaving a small portion behind. It is considered for patients with benign nodules, small goitres, or when only one side of the thyroid is affected. This helps preserve some natural thyroid function, though hormone supplements may still be needed.
- Hemi-Thyroidectomy (Lobectomy): This involves the removal of one lobe (half) of the thyroid gland. It is often performed when a nodule, cyst, or localised tumour is limited to just one side. In many cases, the remaining thyroid lobe can produce enough hormones to keep the body functioning normally.
- Near-Total Thyroidectomy: In this method, almost the entire gland is removed, but a tiny part of thyroid tissue is left to protect nearby structures like the parathyroid glands and recurrent laryngeal nerve. It's often performed in cases where a balance between effective treatment and reduced surgical risk is needed.
1-2 Hours
Surgery Duration
General Anesthesia
Anesthesia Used

When is Thyroidectomy Recommended?
Thyroidectomy is recommended for thyroid cancer, large goiters, overactive thyroid, suspicious nodules, or compression symptoms.
- Thyroid Cancer: Thyroidectomy is often recommended for individuals diagnosed with thyroid cancer. Depending on the type, stage, and extent of cancer, a partial or total thyroidectomy may be performed to remove cancerous tissue and prevent its spread.
- Hyperthyroidism (Overactive Thyroid): When medications and other treatments fail to adequately control hyperthyroidism caused by conditions like Graves' disease or toxic nodular goitre, thyroidectomy may be considered.
- Goitre: A goitre is a thyroid gland growth that can cause discomfort, difficulty swallowing, or breathing problems. If the goitre is large, symptomatic, or causing compression of nearby structures, thyroidectomy may be recommended.
- Thyroid Nodules: Thyroidectomy may be indicated if thyroid nodules are suspicious for cancer or causing significant symptoms including breathing, swallowing, or speech issues.
- Thyroiditis: In certain cases of thyroiditis, especially those associated with severe pain or inflammation, thyroidectomy may be considered to alleviate symptoms and manage the condition.
- Recurrent Thyroid Cysts: If thyroid cysts reoccur despite drainage or other treatments, thyroidectomy might be considered to prevent further complications.
- Cosmetic Concerns: In some instances, thyroidectomy might be performed for cosmetic reasons when a visible goitre or thyroid enlargement affects a person's appearance.
- Genetic Conditions: Inherited genetic conditions such as multiple endocrine neoplasia (MEN) types 2A and 2B, which increase the risk of thyroid cancer, may lead to the recommendation for prophylactic thyroidectomy.
- Non-Cancerous Conditions: Rarely, certain non-cancerous conditions, such as severe thyroid storm or uncontrolled hyperthyroidism, may necessitate thyroidectomy as a last resort.
Preparing for Thyroidectomy Surgery?
Preparation includes blood tests, imaging, medication adjustments, and following your surgeon's instructions for a safe procedure.
- Preparing for Thyroidectomy Surgery: Preparing for your thyroidectomy surgery is an important step to ensure a safe procedure and smooth recovery. Proper planning helps minimise risks, optimise your health before the operation, and make recovery easier.
- Medical Evaluation & Pre-Operative Assessment: Your surgeon will examine your medical history, your current medication, and your past thyroid or neck treatment. It may be needed to do routine tests like blood work, thyroid-function tests, ultrasound, or ECG. These assessments ensure you are fit to operate, and guide the team on how to do so.
- Medication & Lifestyle Adjustments: Some medications, such as blood thinners or herbal supplements, may need to be paused before surgery to reduce bleeding risks. If you are on thyroid medicines, your doctor will adjust the dosage or give special instructions. Smoking should be avoided 4-6 weeks before surgery, and a healthy diet will prepare your body for faster recovery.
- Preparing at Home & Support System: Arrange for a family member or close friend to accompany you on the day of surgery and assist during the first 24-48 hours at home. Soft, easy-to-swallow foods should be kept ready, as your throat may feel sore after surgery. Keeping extra pillows handy will also help you rest in a comfortable, slightly elevated position.
- Day Before & Day of Surgery: Follow fasting instructions, usually no food or drink after midnight before surgery. A shower with antiseptic soap may be advised to minimise infection risk. Avoid lotions, perfumes, nail polish, or jewellery. Dress in loose, comfortable clothing and arrive on time for the surgical team's final checks.
What Happens During Thyroidectomy Surgery?
During thyroidectomy, the surgeon removes part or all of the thyroid gland under general anesthesia, taking care to protect nearby nerves and glands.
- Anesthesia & Preparation: Before the procedure, you'll be placed under general anaesthesia so that you remain fully asleep and pain-free. The surgical area is cleaned and prepped to maintain sterility.
- Incision & Access to Thyroid Gland: The surgeon makes a small incision at the base of the neck, usually along natural skin creases, so that the scar is less visible. Through this incision, the muscles are gently moved aside to provide access to the thyroid gland.
- Removal of Thyroid Tissue: Depending on your condition, the surgeon may remove one lobe (lobectomy), part of the thyroid (subtotal thyroidectomy), or the entire gland (total thyroidectomy). Care is taken to preserve important structures like the parathyroid glands and vocal cord nerves.
- Bleeding Control & Closure: Bleeding is carefully controlled throughout the procedure to minimise complications. Once the thyroid tissue is removed, the incision is closed using sutures, surgical glue, or small strips. A small drain may sometimes be placed to prevent fluid build-up.
- Recovery Room & Monitoring: After surgery, you'll be moved to a recovery area where your vital signs are closely monitored. Most patients are encouraged to walk within hours after the procedure, and many can go home the next day, depending on recovery progress.
Who Will Perform the Thyroidectomy Procedure?
Specialists with expertise in thyroid-related conditions perform thyroidectomy surgery.
Recovery After Thyroidectomy Surgery Procedure:
Recovering from thyroidectomy is usually smooth, with most patients resuming daily activities within a few weeks.
First Few Days After Surgery
Mild neck pain, swelling, or hoarseness is common but improves quickly. Walking and light movement are encouraged. A drain may be placed to remove fluid, but it is usually removed before discharge.
Doctor's Tip: "Don't worry if your voice feels weak, it typically improves within days to weeks."
Weeks 2 to 4
Swelling reduces, and the incision heals steadily. Thyroid hormone replacement begins (if the entire gland is removed) and may need dosage adjustments. Light work and daily routines are usually possible.
Doctor's Tip: "Take your thyroid medication regularly, it helps restore your body's balance."
Weeks 5 to 6
Energy levels improve, and most people return to normal activities. Exercise can be resumed gradually, though avoid heavy lifting or strain on the neck until cleared.
Doctor's Tip: "Follow-up visits are key to ensuring your hormone levels are stable."
3 to 6 Months Post-Surgery
The scar fades, energy stabilises, and long-term hormone monitoring becomes part of routine care.
Doctor's Tip: "Even if you feel fine, regular thyroid check-ups are essential for lasting health."
Lifestyle Changes After Thyroidectomy
- Take thyroid hormone replacement if prescribed to maintain hormone balance.
- Monitor calcium levels and take supplements if advised.
- Avoid strenuous activities until cleared by your surgeon.
- Eat a balanced diet rich in calcium and vitamin D to support recovery.
Benefits of Thyroidectomy
The surgery treats thyroid cancer, relieves compressive symptoms, and helps control hyperthyroidism when medications are ineffective.
- Relief from Symptoms: Surgery to eliminate an enlarged thyroid (goitre) or pathological tissue can help ease the condition of the patient who has difficult swallowing, breathing problems or constant throat pain.
- Treatment of Thyroid Cancer: Thyroidectomy provides the best cure of thyroid cancer, as it guarantees a total elimination of the cancerous cells and minimizing chances of recurrence.
- Control of Hyperthyroidism: For patients with overactive thyroid glands, surgery provides permanent relief when medications or radioactive iodine fail.
- Improved Quality of Life: Many patients experience improved energy, confidence, and comfort after surgery as health issues caused by thyroid dysfunction are resolved.
Risks of Thyroidectomy
Potential risks include bleeding, infection, voice changes due to nerve injury, and low calcium levels if parathyroid glands are affected
- Voice Changes: Rarely, injury to the recurrent laryngeal nerve can cause temporary or permanent hoarseness or voice changes.
- Low Calcium Levels: If parathyroid glands are affected, calcium levels may drop, leading to tingling or muscle cramps, which are usually treatable with supplements.
- Infection or Bleeding: As with any surgery, there is a small risk of infection or post-operative bleeding, though modern techniques make this rare.
- Need for Lifelong Medication: In cases where the entire thyroid gland is removed, patients must take thyroid hormone replacement pills daily to maintain a normal metabolism.
What is the Cost of Thyroidectomy in India?
The cost of thyroidectomy surgery in India generally ranges between Rs. 1,50,000 to Rs. 2,50,000, depending on several factors. The type of surgery plays a major role, as partial thyroidectomy is usually less expensive compared to a total thyroidectomy. The complexity of the case also affects the overall expenses, since advanced procedures require longer operating time, greater surgical expertise, and sometimes additional technology.






















































