Thyroid Cancer: Symptoms, Causes and Treatments
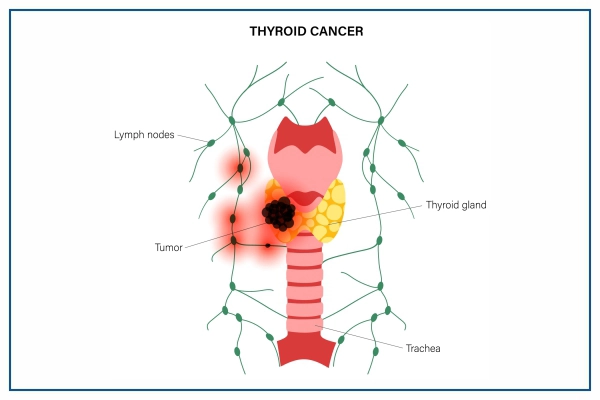
Thyroid cancer is a cancer disease in which abnormal cells grow in the thyroid tissue. Cancer begins in the thyroid gland when the normal cells in the gland multiply abnormally forming a mass called a tumour with capability to metastasize to other parts of the body.
What is Thyroid Gland?
The thyroid gland is a butterfly-shaped endocrine gland present in the front and both sides of the trachea just at the bottom of the larynx. The gland has two lobes, the right, and the left lobes, that are connected with each other by an intermediate structure, called the isthmus.
The thyroid gland is a component of the endocrine system, which is responsible for controlling hormonal levels in the body. This gland takes in iodine from the bloodstream to make thyroid hormones, manage the basal metabolic rate (BMR), calcium metabolism and induce the somatic and psychic growth in the body.
A goitre can be the abnormal swelling of the thyroid gland. The common cause of goitre is iodine deficiency.
There are two types of cells found in the thyroid gland.
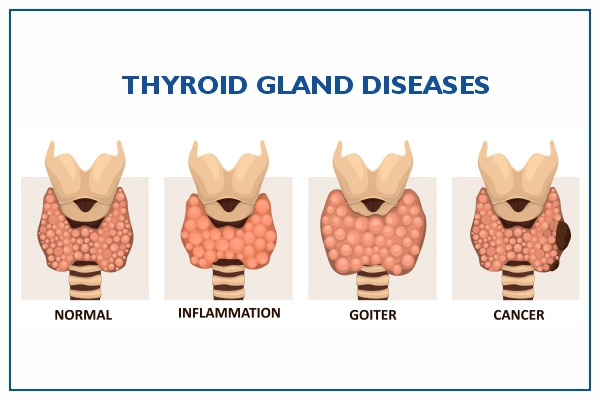
- Follicular cells: These cells produce thyroid hormones. The follicular cells of the thyroid gland constitute the major type of cells. They produce and secrete thyroxine (T4) and triiodothyronine (T3).
- C cells: Parafollicular cells, or C cells, are neuroendocrine cells found in the thyroid gland. These cells secrete the calcitonin hormone that takes part in calcium metabolism.
A thyroid tumour can be malignant or benign. A malignant (cancerous) tumour means it can progress and metastasize to other parts of the body. A benign tumour indicates that it will grow but will not spread. Thyroid gland tumors can also be called thyroid nodules. Nearly 90% of all thyroid nodules are benign lesions.
Get a second opinion from trusted experts and makeconfident, informed decisions.
Types of thyroid cancer
Thyroid cancer is divided into five types. They are:
- Papillary thyroid cancer (PTC): It is the most common form of thyroid cancer. It occurs from follicular thyroid cells and has slow growth. The papillary carcinoma is found in only one thyroid lobe, only 10% to 20% of this cancer appears in both lobes. This cancer can spread to lymph nodes. The tumour cells are very much similar to normal thyroid tissue under a microscope.
- Follicular thyroid cancer (FTC): It is the second most common type of thyroid cancer after papillary thyroid carcinoma. Both follicular and papillary thyroid cancers constitute 95% of thyroid cancer cases. FTC emerges from follicular cells and grows slowly. Both follicular and papillary thyroid cancers are curable if detected at an early stage and in individuals younger than 50 years.
- Hurthle cell cancer (HCC): It is also called Hurthle cell carcinoma, and is a rare thyroid cancer. These tumours can be benign such as Hurthle cell adenomas. Malignant Hurthle cell carcinomas are much more likely to spread to lymph nodes and cause metastasis.
- Medullary thyroid cancer (MTC): Medullary thyroid carcinoma develops when the C cells become malignant and grow abnormally. Rarely, it can result due to a genetic syndrome called multiple endocrine neoplasia type 2 (MEN2).
- Anaplastic thyroid cancer (ATC): Anaplastic thyroid carcinoma is a rare type of thyroid cancer. It is an aggressive type and fast-growing thyroid cancer and carries a very poor prognosis due to its fast uncontrolled growth of cells and resistance to cancer therapy.
Thyroid Cancer symptoms
The early stage of thyroid cancer doesn't exhibit any signs or symptoms. In its advanced stage, it may cause:
- A lump or nodule that can be felt in front of the neck.
- Hoarse voice
- Difficult to swallow
- Difficulty breathing
- Persistent cough
- Swollen lymph nodes in the neck
- Pain sensation in the neck and throat.
When to see a doctor?
If you experience any thyroid cancer symptoms involving discomfort in your neck region, make an appointment with your doctor.
Thyroid cancer Causes
Thyroid cancer occurs when the thyroid cells bring about changes in their DNA. The cell's DNA controls the cell's activities. The DNA mutations cause the cells to grow abnormally in the thyroid tissue. The accumulation of cells together forms a mass called a thyroid tumour.
The malignant tumour can increase and metastasis can take place to the lymph nodes in the neck and also to other body parts.
Risk Factors of Thyroid Cancer
- Female sex : Women are more prone to develop thyroid cancers.
- High radiation exposure : Radiotherapy to the head and neck regions increases the risk of papillary and follicular thyroid cancers.
-
Genetic factors : Inherited genes also play an important role in the development of thyroid cancer.
- A person's likelihood of developing MTC is higher if they have a family history of the disease.
- Individuals having MEN2 syndrome also have a high possibility of developing cancers.
- Occurrence of precancerous polyps in the colon (large intestines) in the family history, increases the risk of developing papillary thyroid cancer.
- Eating less iodine : Less amount of iodine in the diet can cause thyroid problems.
- Race : White and Asian people are more vulnerable to developing thyroid cancer. But this illness can happen to anybody irrespective of race or ethnicity.

Diagnosis of Thyroid Cancer
The diagnosis of thyroid cancer is done by the following test-
- Physical examination The thyroid doctor will perform a physical examination of the neck to detect growths or changes in the thyroid gland, such as a lump or nodes on the thyroid. The doctor will record the medical history such as any radiation exposure or a family hereditary.
- Thyroid profile test There are many blood tests to detect thyroid problems. One of the tests is known as tumour marker tests or cancer markers, in the blood, urine, or body tissues.
- Blood tests include-
- Thyroid hormone levels
- Thyroid-stimulating hormone (TSH)
- Thyroglobulin (Tg) and thyroglobulin antibodies (TgAb)
- Medullary type-specific tests
- Ultrasound scan High-frequency sound waves of ultrasound is used to find out thyroid disorders.
- Biopsy test A biopsy test can make a definite diagnosis. To determine whether a nodule is malignant or benign is done through a biopsy.
- Molecular testing of the nodule sample Genetic testing of the thyroid nodule may help to know the risk of the thyroid nodule being cancerous.
- Radionuclide scanning It involves a whole-body scan. It can be done with a very less quantity and harmless amount of radioactive iodine I-131 or I-123, called a tracer. This test is mostly done to examine a thyroid nodule.
- X-ray A chest X-ray test is done to check if cancer has spread to the lungs.
- Computed tomography (CT or CAT) scan CT scans are used to inspect thyroid cancer to examine parts of the neck that cannot be done with ultrasound.
- Positron emission tomography (PET) or PET-CT scan The PET scan is performed to check whether cancer has metastasized.
Treatments of Thyroid Cancer
The treatment for thyroid cancer depends upon the type, stage of the cancer and the overall health of the person.
Most thyroid cancer patients show an excellent prognosis, as most of the cases can be cured with timely treatment.
The treatment methods include:
- Surgery
- Thyroidectomy: It involves removing all or most of the thyroid gland.
- Thyroid lobectomy: Removing a part of the thyroid gland
- Lymph node dissection: Taking out lymph nodes in the neck
- Thyroid hormone therapy: It is a treatment to replace or supplement the thyroid hormones. This therapy medication is usually taken in pill form.
- Radioactive iodine This treatment uses a form of radioactive iodine to destroy thyroid cells and thyroid cancer cells remaining after the surgery.
- Alcohol ablation or ethanol ablation It uses a needle to inject alcohol into small areas of cancerous thyroid tissues. The alcohol ablation therapy causes the thyroid cancer cells to shrink.
- Advanced thyroid cancer treatment involves:
- Targeted drug therapy
- Radiation therapy
- Chemotherapy
- Killing cancer cells with heat and cold therapy
Your health is everything - prioritize your well-being today.
Prevention and Self Care of Thyroid Cancer
By taking certain precautions and self care it is easy to prevent the development or growth of thyroid cancer. They are as follows:
- Eat iodine rich diet
- Stay away from high radiation exposure
- Take prescribed thyroid medicines on time
- Avoid smoking and alcohol consumption for a fast recovery
- Get regular health check-ups
Thyroid Cancer Care at Medicover Hospitals
At Medicover hospitals, we have the most reliable medical team of oncologists and endocrinologists who design a personalized treatment pathway for each patient. We adopt a multi-faceted approach in managing cancer of the thyroid gland with the active participation of healthcare specialists from different departments to address the disease for holistic recovery and wellness. For the treatment of thyroid cancer, we explore all the avenues as per unique patient requirements and design a personalized treatment pathway keeping the patient and the family informed at every stage of the treatment. Utilizing the latest diagnostic tools and techniques and the most advanced cancer care methodology, we ensure to offer the best possible treatment outcomes.
Frequently Asked Questions
Can thyroid cancer be cured?
Many cases of thyroid cancer can be effectively treated, especially when detected early. The prognosis varies based on factors like the type of thyroid cancer, its stage at diagnosis, and how well it responds to treatment.
What is radioactive iodine therapy?
A frequent therapy is radioactive iodine. certain types of thyroid cancer. It involves swallowing a radioactive iodine pill, which is taken up by thyroid cells, including cancerous ones. The radiation helps destroy the remaining thyroid tissue after surgery.
Is thyroid cancer hereditary?
While most cases of thyroid cancer are not hereditary, some genetic syndromes such as multiple endocrine neoplasia (MEN) and familial medullary thyroid cancer (FMTC) can increase the risk. Individuals with a family history of genetic disorders may benefit from genetic counseling. thyroid cancer.
What is the follow-up care for thyroid cancer survivors?
After treatment, regular follow-up appointments are important to monitor for any recurrence or new developments. These appointments may include physical exams, blood tests, imaging scans, and discussions about ongoing care and surveillance.
What are the symptoms of thyroid cancer in females?
Symptoms include a lump in the neck, changes in voice, trouble swallowing, neck pain, and unexplained weight loss.
Is thyroid cancer a genetic condition?
Thyroid cancer can be inherited in some situations, particularly in people with a family history or who have genetic disorders such as familial medullary thyroid carcinoma.