What is Coronary Angioplasty and Stents?
Coronary angioplasty and stent insertion are minimally invasive cardiac procedures used to open narrowed or blocked coronary arteries. This helps restore blood flow to the heart muscle, relieve chest pain, and reduce the risk of a heart attack.
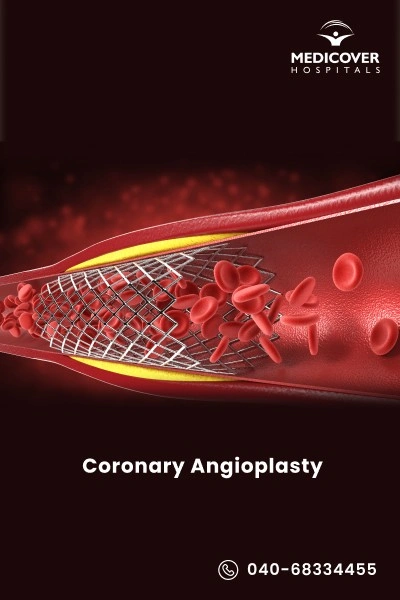
Coronary angioplasty (percutaneous coronary intervention - PCI) is a procedure where a balloon catheter is used to widen narrowed arteries. A stent (small metal mesh tube) is then placed to keep the artery open and ensure continuous blood flow.
Types of Coronary Angioplasty and Stents
There are many types of angioplasty and stents, but based on the condition and complexity, the doctor chooses the one that is best suited for the patient.
- Balloon Angioplasty: A balloon catheter is used to compress plaque and widen the artery.
- Bare-Metal Stents (BMS): A bare stent is placed to keep the artery open. It is an old option and is no longer commonly used today.
- Drug-eluting stents (DES): These release medication to prevent the artery from narrowing over time.
- Primary Angioplasty: Emergency angioplasty is performed during an ongoing heart attack.
- Rotational Atherectomy: A high-speed device used to remove hardened plaque before stent placement in severely calcified arteries.
30 Mins to 2 Hours
Surgery Duration
Local anesthesia with sedation
Anesthesia Used
1 Week
Full Recovery Timeline
When is Coronary Angioplasty Recommended?
Coronary angioplasty is usually recommended for people with blocked or narrowed heart arteries that reduce blood flow and cause chest pain or increase the risk of a heart attack. The main indications of Coronary Angioplasty and Stents include:
- Severe chest pain (angina) that does not improve with medicines or lifestyle changes.
- Narrowing or blockage of coronary arteries found during diagnostic tests.
- Acute heart attack, where immediate angioplasty helps restore blood flow and prevent damage.
- Reduced blood supply to the heart muscle leading to breathlessness or fatigue.
- High-risk cases where bypass surgery is not suitable or needed.
Who is a Candidate for Coronary Angioplasty and Stents?
You may be a suitable candidate if you:
- Have been diagnosed with narrowed or blocked coronary arteries.
- Experience chest discomfort, fatigue or breathing difficulty due to poor cardiac perfusion.
- Shows significant blockage on angiography.
- Candidates who have had a heart attack are at high risk of having another one.
- Those who are physically stable and can tolerate a catheter-based procedure.
Cardiac evaluation, including stress testing, echocardiography, and coronary angiography, helps determine eligibility.
Preparation for Coronary Angioplasty and Stents
Preparation is simple but important for safety and outcomes:
- Your doctor will review your medical history, current medications, and allergies.
- Blood tests, ECG, echocardiogram, or angiography may be done to assess heart health.
- You may be advised to stop eating or drinking a few hours before the procedure.
- Certain medications, especially blood thinners or diabetes medicines, may need to be adjusted.
- Inform your doctor if you are pregnant, have kidney problems, or use any herbal supplements.
- Arrange for someone to drive you home after the hospital stay, as you may not be able to resume normal activities immediately.
Coronary Angioplasty and Stents Procedure
The process includes the following steps:
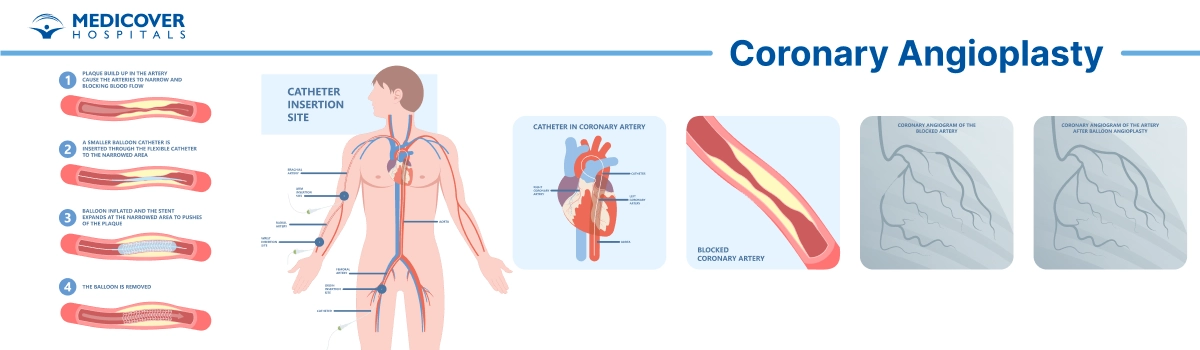

- Anaesthesia: Local anaesthesia may numb only the area of insertion, and mild sedation may be given to promote relaxation.
- Catheter Insertion: A thin tube is inserted through the femoral (groin) or radial (wrist) artery and guided to the coronary arteries.
- Angiography: Contrast dye is injected to locate blockages on X-ray imaging.
- Balloon Inflation: A balloon-tipped catheter is inflated to widen the narrowed artery.
- Stent Placement: A mesh stent is placed and expanded to keep the artery open permanently.
- Deployment of Stent: The stent, which is folded on itself, expands when the balloon gets inflated and fixes in place forever.
- Deflation and Removal: Once the stent is in the right spot, the balloon deflates and the catheter is withdrawn.
- Completion and Monitoring: The catheter is removed and pressure is applied to prevent bleeding. You are monitored in a recovery unit.
This procedure usually takes about 1-2 hours and helps restore proper blood flow to the heart, relieving symptoms like chest pain and reducing the risk of heart attack.
Recovery after Coronary Angioplasty and Stents
Recovery from coronary angioplasty is usually quick, as it is a minimally invasive procedure. Most patients can return to normal activities within a few days, depending on their overall health and the severity of their heart condition.
- Hospital Stay: Typically, patients stay in the hospital for 1-2 days for monitoring.
- Activity Level: Light activities can often be resumed within a week, but strenuous exercise and heavy lifting should be avoided for a few weeks.
- Medication: Doctors usually prescribe blood-thinning medications to prevent clot formation around the stent.
- Lifestyle Changes: Following a heart-healthy diet, exercising regularly, and quitting smoking are essential for long-term recovery.
- Follow-up: Regular check-ups are necessary to monitor stent performance and heart health.
With proper care, most patients experience significant relief from symptoms and improved quality of life after angioplasty.
Lifestyle Changes After Coronary Angioplasty
Adopting healthy lifestyle habits after coronary angioplasty is crucial to maintain stent function, improve heart health, and prevent future blockages. Some important changes include:
- Heart-Healthy Diet: Eat more fruits, vegetables, whole grains, lean proteins, and reduce salt, sugar, and unhealthy fats.
- Regular Exercise: Engage in light to moderate physical activity as advised by your doctor, such as walking, swimming, or cycling.
- Quit Smoking & Alcohol Moderation: Smoking damages blood vessels, and excessive alcohol can strain the heart, so avoiding them is vital.
- Weight Management: Maintain a healthy body weight to reduce strain on the heart.
- Stress Control: Practice relaxation techniques like yoga, meditation, or deep breathing.
- Medication Adherence: Take prescribed medicines, especially blood thinners and cholesterol-lowering drugs, regularly.
- Regular Check-ups: Attend follow-up appointments to monitor heart function and stent health.
These lifestyle changes can significantly enhance recovery and lower the risk of future cardiac issues.
Benefits of Coronary Angioplasty and Stents
- Immediate Symptom Relief: Rapid improvement in chest pain and shortness of breath.
- Prevention of Heart Attacks: Reduces the risk of future cardiac events in many patients.
- Minimally Invasive: No need for open-heart surgery or large incisions.
- Quick Recovery: Short hospital stay and faster return to normal activities.
- Improved Heart Function: Restores blood supply to the heart muscle.
Risks and Complications of Coronary Angioplasty and Stents
Although it is considered safe, some complications include:
- Bleeding or Bruising: At the catheter insertion site.
- Allergic Reaction: To contrast dye used during angiography.
- Restenosis: Re-narrowing of the artery, more common with bare-metal stents.
- Blood Clots: Inside the stent, requiring dual antiplatelet therapy.
- Heart Attack or Stroke: Rare but serious risks during or after the procedure.
- Kidney Impairment: From contrast dye, especially in those with pre-existing kidney disease.
Coronary Angioplasty and Stent Procedure Cost in India
Coronary angioplasty is a common procedure used to open blocked arteries and improve blood flow to the heart. It often involves placing a small mesh tube called a stent to keep the artery open.
What Does the Coronary Angioplasty and Stent Cost Include?
The cost typically covers the hospital charges, surgeon's fees, the angioplasty procedure itself, stent(s), medicines, and post-procedure care.
- Coronary Angioplasty Procedure: Usually costs between Rs. 70,000 and Rs. 2,00,000 depending on the hospital, city, and patient's condition.
- Stent Cost: A single heart stent generally ranges from Rs. 7,000 to Rs. 35,000. Drug-eluting stents (which reduce artery narrowing risk) tend to be on the higher end of this scale.
- For multiple stents, the cost increases depending on the number used.