What Is a Surgical Aortic Valve Replacement (SAVR)?
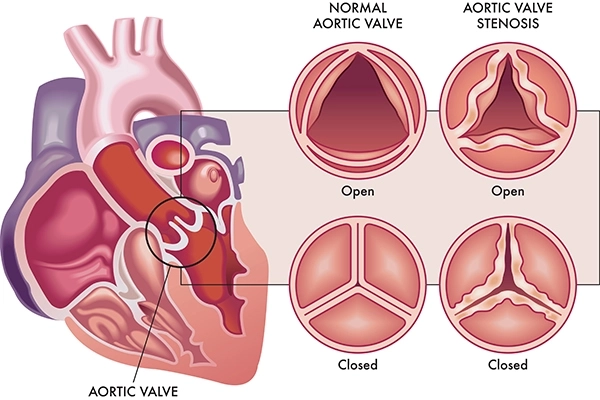
SAVR is a kind of open heart surgery that is carried out to replace a broken or diseased aortic valve. The valve of the aorta is in charge of the regulation of blood flow of the heart to the rest of the body. It becomes hard to dilate (aortic stenosis) or leaky (aortic regurgitation) and pushes the heart to work harder, resulting in such symptoms as chest pain, breathlessness, and fatigue.
In the process of SAVR, the damaged valve is removed and a mechanical valve (comprised of materials that are tough and durable) or a biological valve (comprised of animal tissue) is used. This replenishes the normal blood circulation, eases the load on the heart and also makes the heart work better. SAVR can generally be suggested to patients that are fit to undergo open-heart surgery and require long-term outcomes.
Types of Surgical Aortic Valve Replacement (SAVR)
SAVR can be performed using different valve types and surgical approaches depending on the patient's condition, age, and lifestyle needs:
- Mechanical Valve Replacement: Made from durable materials such as titanium or carbon. Mechanical valves last a lifetime but require lifelong blood-thinning medications to prevent clots. Best suited for younger patients who can safely manage anticoagulation therapy.
- Biological (Tissue) Valve Replacement: Made from animal tissue (bovine or porcine). These valves do not usually require long-term anticoagulation and are ideal for older patients, but they may wear out after 10-20 years and might need replacement.
- Stentless Valve Replacement: A special type of tissue valve that offers better blood flow and may be beneficial for patients with smaller heart anatomy or those needing improved hemodynamics.
- Homograft (Donor Valve) Replacement: Uses a valve from a human donor. These are often used in complex cases or for patients with active valve infections (endocarditis).
- Minimally Invasive SAVR: Instead of a full open-heart approach, smaller incisions are used. This reduces recovery time, scarring, and discomfort while still replacing the valve effectively.
2-4 Hours
Surgery Duration
General Anesthesia
Anesthesia Used
6 to 12 weeks
Full Recovery

When is SAVR Recommended?
Surgical Aortic Valve Replacement (SAVR) is recommended for patients with severe aortic valve disease that significantly affects heart function and quality of life. Some of the main reasons include:
- Severe Aortic Stenosis: Narrowing of the aortic valve that restricts blood flow from the heart, causing chest pain, fainting spells, breathlessness, or fatigue. SAVR is often the definitive treatment.
- Severe Aortic Regurgitation: A leaky aortic valve that allows blood to flow backward into the heart, leading to enlargement of the left ventricle, breathlessness, and reduced exercise tolerance.
- Symptomatic Patients: Individuals with chest pain, fainting, or shortness of breath due to valve dysfunction benefit most from valve replacement.
- Asymptomatic Patients with Heart Dysfunction: Even if no symptoms are present, SAVR is indicated when tests show reduced heart function or enlargement due to aortic valve disease.
- Congenital Aortic Valve Disease: Conditions like a bicuspid aortic valve that progress to severe stenosis or regurgitation, often requiring replacement at a younger age.
- Failed Previous Valve Surgery or Prosthetic Valve Dysfunction: Patients who had a prior valve replacement but now have a failing or infected prosthetic valve.
Preparing for SAVR Surgery Procedure
Preparing for Surgical Aortic Valve Replacement is essential for a safe procedure and smooth recovery. Patients should expect several steps before surgery:
Medical Evaluation & Pre-Op Tests
- A complete medical review including history, medications, and overall fitness.
- Tests such as echocardiogram, cardiac catheterization, chest X-ray, blood work, and ECG to assess heart function and surgical readiness.
- Results are reviewed to finalize the surgical plan and minimize risks.
Health Habits & Lifestyle Adjustments
- Quit smoking at least 4-6 weeks before surgery to improve circulation and healing.
- Avoid alcohol and stop blood-thinning medications (like aspirin or warfarin) under doctor guidance.
- Eat a balanced diet rich in protein, vitamins, and minerals to boost recovery.
Preparing Your Home & Support System
- Arrange for a family member or friend to assist during the hospital stay and early recovery at home.
- Set up a comfortable space at home with essentials (pillows, water, easy clothing) within reach.
- Prepare light meals in advance, as heavy lifting and strenuous activity should be avoided post-surgery.
The Day Before & Day of Surgery
- Follow fasting instructions (usually no food or drink after midnight).
- Bathe using antiseptic soap as advised and avoid lotions or perfumes.
- Wear loose-fitting clothes and remove all jewelry, makeup, or nail polish before arriving at the hospital.
How is Surgical Aortic Valve Replacement (SAVR) Performed?
During SAVR, the diseased aortic valve is surgically removed and replaced with a prosthetic valve under open-heart conditions, sometimes with minimally invasive options.
- Preparation & Anesthesia: On the day of surgery, the cardiac team reviews your case one more time. SAVR is performed under general anesthesia, meaning you'll be fully asleep and pain-free during the procedure.
- Incision & Access to the Heart; A midline incision is made in the chest (sternotomy) to access the heart. In some cases, a smaller incision (minimally invasive approach) may be used. You are connected to a heart-lung machine, which temporarily takes over the function of your heart and lungs.
- Removing the Damaged Valve: The surgeon carefully opens the aorta and removes the diseased or damaged aortic valve, preparing the area for replacement.
- Placing the New Valve: A new mechanical, biological, or donor valve is positioned securely into place. The choice of valve depends on age, lifestyle, and medical condition.
- Closing the Incision: Once the valve is in place and functioning properly, the aorta is closed, and the heart is restarted. The sternum is wired shut, and the incision is closed with sutures or staples.
- Recovery in ICU: Patients are then moved to the intensive care unit (ICU) for close monitoring. Ventilation support may be required for a few hours, and heart function, blood pressure, and oxygen levels are closely watched.
Recovery After SAVR Surgery
Recovering from Surgical Aortic Valve Replacement is a gradual process, and proper care helps ensure the best results.
First Few Days After Surgery
- Expect chest discomfort, swelling, and fatigue, normal signs of healing.
- You'll stay in the ICU for close monitoring before moving to a regular hospital room.
- Breathing exercises and gentle walking are encouraged to improve lung function and circulation.
- Avoid straining or sudden movements; your chest incision needs protection.
Doctor's Tip: "Take pain medications on schedule, don't wait until the pain worsens."
Weeks 2 to 4
- Most patients are discharged within 7-10 days and continue recovery at home.
- Light activities, like walking short distances and simple household tasks, can be resumed.
- Keep the incision clean and dry; monitor for any signs of infection.
- Cardiac rehabilitation programs may be started under your doctor's guidance.
Doctor's Tip: "Follow your activity plan closely, gradual movement is key to building strength safely."
Weeks 5 to 6
- Energy levels improve, and swelling decreases.
- Many patients return to office-based or non-strenuous work around this time.
- Avoid lifting heavy objects, driving (unless cleared), or intense exercise.
Doctor's Tip: "Even if you feel better, your chest bone takes time to heal, don't rush into heavy activity."
3 to 6 Months Post-Surgery
- The sternum is usually fully healed by 3 months.
- Most patients notice improved breathing, reduced fatigue, and overall better heart performance.
- You can gradually return to normal exercise and daily routines with medical approval.
Doctor's Tip: "Stick to your heart-healthy lifestyle, diet, exercise, and medications will protect your new valve."
Lifestyle Changes After SAVR
- Take prescribed medications, including anticoagulants if using a mechanical valve.
- Follow a heart-healthy diet and maintain hydration.
- Avoid heavy lifting or strenuous activity until cleared by your cardiologist.
- Attend all follow-up appointments and echocardiograms to monitor valve function.
Benefits of SAVR Surgery
SAVR restores normal blood flow, relieves symptoms, improves heart function, and reduces the risk of heart failure or other complications.
- Improved Heart Function: Restores normal blood flow through the heart, which reduces stress on the cardiac muscle and helps prevent long-term heart damage.
- Symptom Relief: Eases chest pain, breathlessness, dizziness, and fatigue, allowing patients to return to daily activities with greater comfort.
- Durability of Results: Mechanical valves can last a lifetime, while tissue valves provide many years of reliable performance, reducing the chances of repeat surgery.
- Enhanced Quality of Life: Patients gain better energy levels, improved mobility, and greater independence, which also boosts emotional well-being.
- Prevention of Serious Complications: Timely surgery lowers the risk of life-threatening problems like heart failure, arrhythmias, or sudden cardiac arrest.
Risks of SAVR Surgery
Potential risks include infection, bleeding, arrhythmias, prosthetic valve complications, or issues related to anesthesia.
- Bleeding or Infection: As an open-heart procedure, there is some risk, though modern techniques and antibiotics keep it under control.
- Stroke or Blood Clots: More likely with mechanical valves, requiring lifelong use of blood-thinning medicines to prevent complications.
- Arrhythmias (Irregular Heartbeat): Temporary rhythm problems may occur post-surgery but are usually managed with medicines or pacing.
- Valve-Related Issues: Tissue valves may wear out over time, leading to the need for a second replacement in the future.
- General Surgical Risks: Includes anesthesia side effects, slow healing, or complications in patients with other health conditions, though careful monitoring helps reduce these risks.
How much does a SAVR (Surgical Aortic Valve Replacement) Procedure Cost?
The cost of Surgical Aortic Valve Replacement (SAVR) in India usually ranges between Rs. 3,00,000 to Rs. 7,00,000, depending on factors like the type of replacement valve (mechanical or biological), hospital facilities, surgeon's expertise, and length of hospital stay.












































