Advanced Percutaneous Transluminal Coronary Angioplasty (PTCA) with Cardiac Care
At Medicover Hospitals, percutaneous transluminal coronary angioplasty (PTCA) is performed by experienced cardiologists using advanced cath lab technology and modern cardiac care facilities. The procedure helps safely and effectively open blocked arteries, improving blood flow to the heart and supporting a faster recovery through comprehensive patient care.
Expert Surgeons
Successful Surgeries
Success Rate
What Is a Percutaneous Transluminal Coronary Angioplasty?
Percutaneous Transluminal Coronary Angioplasty, or PTCA, is a medical procedure used to open narrowed or blocked arteries in the heart. These blockages are usually caused by plaque buildup, which can reduce blood flow and lead to chest pain or heart attacks.
During the percutaneous transluminal coronary angioplasty procedure, a thin tube called a catheter is inserted into a blood vessel, usually in the arm or leg, and guided to the affected coronary artery. A small balloon at the tip of the catheter is then inflated to widen the artery and improve blood flow. In many cases, a tiny mesh tube called a stent is placed to keep the artery open.
Types of Percutaneous Transluminal Coronary Angioplasty (PTCA)
There are different types of PTCA procedures, depending on the heart condition and the patient's needs:
- Balloon Angioplasty
- Stent Placement
- Drug-Eluting Stent (DES)
- Bare-Metal Stent (BMS)
- Rotational Atherectomy (Rotablation)

Percutaneous Transluminal Coronary Angioplasty (PTCA) Specialists Near You
Find trusted percutaneous transluminal coronary angioplasty (PTCA) specialists at Medicover Hospitals across India in multiple locations. Choose your city to connect with experienced cardiologists for advanced heart artery blockage treatment, high success rates, and comprehensive patient care support.
Why Choose Medicover Hospitals for Percutaneous Transluminal Coronary Angioplasty?
Get a second opinion from trusted experts and makeconfident, informed decisions.
Complete Guide to Percutaneous Transluminal Coronary Angioplasty (PTCA)
Everything you need to know about the procedure, preparation, and recovery
When is Percutaneous Transluminal Coronary Angioplasty Recommended?
Percutaneous transluminal coronary angioplasty is indicated when narrowed or blocked coronary arteries reduce blood flow to the heart. Common situations include:
- Angina (Chest Pain): When lifestyle changes or medications do not relieve persistent chest pain caused by restricted blood flow.
- Heart Attack (Myocardial Infarction): PTCA can be performed urgently to restore blood flow and reduce heart damage during a heart attack.
- Severe Coronary Artery Disease: For patients with significant blockages in major coronary arteries that affect heart function.
- Failed Medication or Other Treatments: When medications, lifestyle changes, or other non-invasive treatments are not effective in controlling symptoms.
- High-Risk Patients: In certain cases, PTCA is chosen to prevent further complications and improve overall heart health.
PTCA helps improve blood flow, relieve symptoms, and lower the risk of future heart problems. Your cardiologist will recommend this procedure based on your heart condition, test results, and overall health.
Preparing for Percutaneous Transluminal Coronary Angioplasty Procedure
Preparing well for Percutaneous Transluminal Coronary Angioplasty (PTCA) helps ensure a safe procedure and smooth recovery. Following your cardiologist's instructions and making simple lifestyle adjustments can improve outcomes and comfort.
Medical Evaluation & Pre-Procedure Visit
- Review your full medical history, current medications, allergies, and heart condition with your cardiologist.
- Complete necessary tests like ECG, blood work, or coronary angiogram to confirm readiness for the procedure.
- Ensure all test results are available at least a few days before the procedure to finalize scheduling and address any concerns.
Health Habits & Lifestyle Adjustments
- Avoid smoking for at least 1-2 weeks before the procedure, as it can affect heart health and recovery.
- Limit alcohol and follow your doctor's instructions regarding medications, especially blood thinners.
- Maintain a balanced diet with adequate protein, vitamins, and minerals to support recovery.
Prepare Your Home and Support System
- Arrange for someone to drive you to and from the hospital and stay with you for the first 24 hours.
- Keep essential items like medications, water, light snacks, comfortable clothing, and reading material within reach.
- Plan simple meals ahead of time so you have nutritious food during recovery without much effort.
The Day Before & Day of Procedure
- Follow fasting instructions provided by your cardiologist, usually no food or drink for a few hours before the procedure.
- Take any prescribed medications exactly as directed and follow any special instructions for heart medications.
- Wear comfortable clothing, avoid jewelry, and remove any makeup or nail polish before arriving at the hospital.
What Happens During Percutaneous Transluminal Coronary Angioplasty Surgery?
Percutaneous Transluminal Coronary Angioplasty (PTCA) is a minimally invasive procedure to open narrowed heart arteries and improve blood flow. It is usually done under local anesthesia with mild sedation, allowing faster recovery compared to open-heart surgery.
- Preparation & Anesthesia: On the day of the procedure, you'll meet the cardiology team to review the process. Local anesthesia is given at the insertion site (wrist or groin), along with mild sedation to keep you relaxed and comfortable.
- Catheter Insertion: A small cut is made in the wrist or groin, and a thin tube (catheter) is gently inserted into the blood vessel. Using X-ray guidance, the catheter is advanced toward the blocked coronary artery.
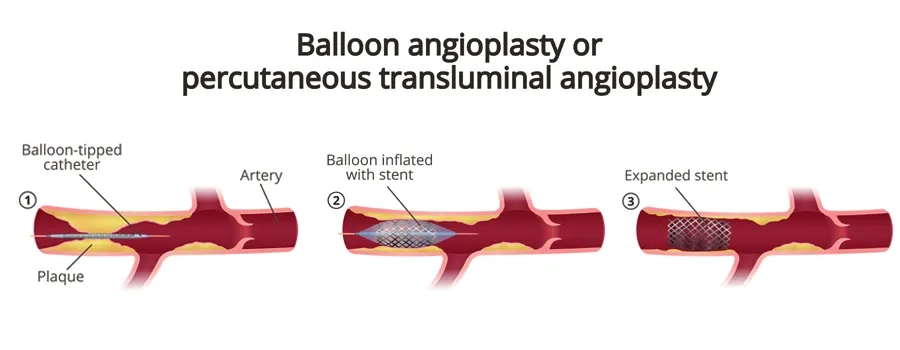
- Balloon Inflation: Once the catheter reaches the blockage, a tiny balloon at its tip is carefully inflated. This pushes the plaque against the artery walls, widening the passage and improving blood flow.
- Stent Placement: In most cases, a stent (small mesh tube) is placed at the site of the blockage. The stent holds the artery open and helps reduce the chance of it narrowing again in the future.
- Completion of the Procedure: After the artery is widened and the stent is placed, the balloon and catheter are removed. The insertion site is then bandaged or sealed to prevent bleeding.
- Recovery Phase: You'll be moved to a recovery area for monitoring of heart rhythm and blood pressure. Most people are encouraged to walk within a few hours and can usually go home the same day or the next, depending on their condition.
Who Will do the Percutaneous Transluminal Coronary Angioplasty Procedure?
Percutaneous Transluminal Coronary Angioplasty (PTCA) is performed by an interventional cardiologist, a heart specialist trained in treating blocked coronary arteries using catheter-based techniques. These doctors are skilled in managing both emergency and planned angioplasty procedures to restore blood flow to the heart.
Your treatment team may also include anesthesiologists, cardiac nurses, and support staff who assist with monitoring, medication, and post-procedure care, ensuring safe recovery and effective results.
Recovery After Percutaneous Transluminal Coronary Angioplasty Surgery Procedure
Recovering from PTCA is usually quicker than traditional surgery, but proper care is essential for long-term heart health.
First 24 Hours After Procedure
- In the first day, you may stay in the hospital for monitoring of heart rhythm, blood pressure, and the catheter site. Mild soreness or bruising at the wrist or groin is common.
- Walking slowly around your room or ward is encouraged, as it helps circulation and reduces the risk of clots.
- Avoid bending, climbing stairs frequently, or lifting heavy items until advised by your doctor.
Days 2 to 7
- Most people feel more comfortable within a few days and can return to light daily activities. Driving and office work are usually possible within 3-5 days, depending on recovery.
- Take prescribed medicines such as blood thinners exactly as directed to prevent further blockages.
Weeks 2 to 4
- By this stage, you should be able to resume regular routines, except strenuous activities. Light walking is encouraged, but avoid running, heavy lifting, or vigorous exercise.
- Follow-up visits are scheduled to monitor healing and check how well your stent or artery is functioning.
1 to 3 Months Post-Procedure
- Most patients regain full strength and energy during this time. Chest discomfort should be gone, and your heart function improves with proper care.
- Long-term recovery depends on healthy lifestyle changes like quitting smoking, eating balanced meals, managing stress, and regular exercise (once approved).
Benefits of Percutaneous Transluminal Coronary Angioplasty Surgery
Percutaneous Transluminal Coronary Angioplasty (PTCA) is a minimally invasive procedure that helps open narrowed or blocked heart arteries. It improves blood flow, eases chest pain and lowers the risk of heart attack, making daily life healthier and more active.
- Restores blood flow to the heart: PTCA opens narrowed or blocked arteries, allowing oxygen-rich blood to reach the heart more effectively and reducing chest pain (angina).
- Reduces risk of heart attack: By clearing blockages, the procedure lowers the chances of future heart attacks and improves long-term heart health.
- Quick recovery and less invasive: Since it's a minimally invasive procedure, recovery is faster compared to open-heart surgery, and hospital stays are usually shorter.
- Improves quality of life: Patients often experience better energy levels, greater ability to perform daily activities, and relief from persistent discomfort.
Risks of Percutaneous Transluminal Coronary Angioplasty Surgery
While angioplasty improves heart health, it also carries some risks. Knowing these helps you prepare and make informed decisions.
- Bleeding or bruising at the catheter site
- Restenosis (artery narrowing again)
- Blood clots in the treated artery
- Heart attack during or after the procedure
- Irregular heart rhythms (arrhythmias)
- Kidney problems from dye used in the procedure
- Artery damage or rupture
- Stroke (rare)
- PTCA complications vary per patient but are usually manageable under medical supervision.
How Much Does Percutaneous Transluminal Coronary Angioplasty (PTCA) Cost?
The cost of Percutaneous Transluminal Coronary Angioplasty (PTCA) in India usually depends on the complexity of the procedure, the hospital facilities, and the cardiologist's experience. On average, the procedure may range from Rs. 75,000 to over Rs. 2,00,000.
Patient Success Stories
Real experiences from patients who regained their mobility and quality of life
""I was very nervous before my angioplasty, but the doctors at Medicover Hospital Hyderabad explained everything clearly. The care I received was excellent, and I felt safe throughout the process.""
""My PTCA surgery at Medicover Hospital went smoothly, and I was able to return to normal life faster than I expected. The team really supported me during recovery.""
""After my procedure at Medicover Hospital Pune, my chest pain reduced, and I feel much more active now. The staff were caring, and the whole experience was reassuring.""



Frequently Asked Questions
1. Can 100% blockage be removed by angioplasty?
Yes, 100% blockage can sometimes be treated with angioplasty using advanced techniques. At Medicover Hospitals, specialists evaluate feasibility based on blockage type and location.
2. What is the recovery time after angioplasty?
Recovery after angioplasty is usually quick, with most patients resuming normal activities within a week. Complete recovery depends on overall heart health and lifestyle changes.
3. Is angioplasty a major surgery?
Angioplasty is a minimally invasive procedure, not a major surgery. It involves inserting a catheter to open blocked arteries and restore blood flow.
4. Which is better, CABG or PTCA?
CABG and PTCA are chosen based on blockage severity. At Medicover Hospitals, doctors recommend the best option depending on patient condition and number of blocked arteries.
5. How much risky is angioplasty?
Angioplasty is generally safe, with low risk of complications like bleeding or restenosis. Experienced cardiologists ensure better outcomes and reduced risks.
6. How many hours is an angioplasty?
Angioplasty typically takes 30 minutes to 2 hours depending on complexity. Patients are usually monitored for a short period after the procedure.
7. How to sleep after angioplasty?
After angioplasty, sleep on your back or as advised by your doctor. Avoid pressure on the catheter site and follow instructions for safe recovery.
8. What foods should I avoid after a stent?
Avoid high-fat, salty, and processed foods after a stent. A heart-healthy diet rich in fruits, vegetables, and whole grains supports recovery and prevents future blockages.
9. What is the immediate care after angioplasty?
Immediate care includes monitoring vital signs, avoiding strenuous activity, and keeping the catheter site clean. At Medicover Hospitals, patients receive complete post-care guidance.
10. Can I live a normal life after angioplasty?
Yes, most patients return to a normal life after angioplasty. Lifestyle changes, medications, and regular check-ups help maintain long-term heart health.
11. Who is a good candidate for angioplasty?
Patients with narrowed or blocked coronary arteries causing chest pain or heart attack are good candidates. Doctors assess condition before recommending the procedure.
12. What is the success rate of angioplasty?
Angioplasty has a high success rate of over 90% in restoring blood flow. Outcomes depend on patient health, blockage severity, and timely treatment.
13. Can you live a normal life after a stent?
Yes, people can live a healthy and active life after stent placement with proper medication, diet, and lifestyle modifications.
14. Can a blockage be cleared without a stent?
Some blockages can be treated with balloon angioplasty alone or medications. However, stents are often used to keep arteries open long-term.
15. How long on blood thinners after stent?
Blood thinners are usually required for 6 to 12 months after stent placement. At Medicover Hospitals, doctors tailor duration based on patient condition.