Advanced Orthognathic Surgery with Expert Jaw Correction Specialists
At Medicover Hospitals, orthognathic (jaw correction) surgery is performed by experienced dental and maxillofacial specialists using advanced surgical technology and modern facilities. The treatment helps correct jaw alignment, improve facial balance and bite function, and support faster recovery through comprehensive, compassionate patient care.
Expert Surgeons
Successful Surgeries
Success Rate
What is Orthognathic Surgery (Jaw Surgery)?
Jaw surgery, also known as orthognathic surgery, is a corrective surgical procedure performed to fix irregularities in the jaw bones and realign the jaws and teeth. This surgery can improve chewing, speaking, breathing, and overall facial appearance.
It is often recommended when orthodontic treatments alone cannot correct issues related to bite, jaw growth, or facial asymmetry.
Jaw surgery can address functional problems, such as difficulty chewing or swallowing, chronic jaw pain, and sleep apnea, as well as aesthetic concerns like misaligned jaws or disproportionate facial features.
Types of Orthognathic Surgery (Jaw Surgery)
There are three primary types of orthognathic surgery used based on the condition of your jaw.
- Maxillary Osteotomy
- Mandibular Osteotomy
- Bimaxillary Osteotomy
- Genioplasty
- Segmental Jaw Surgery
- Distraction Osteogenesis
- TMJ Surgery
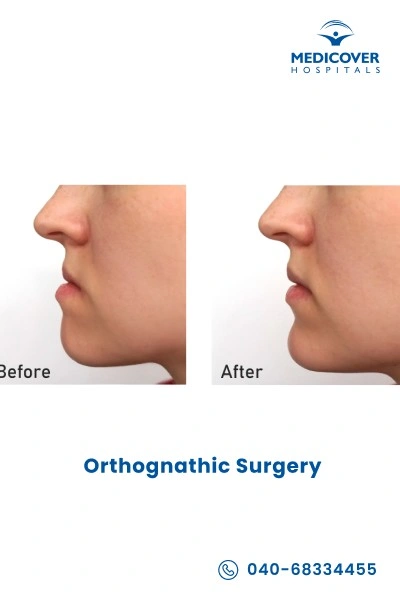
Orthognathic Surgery Specialists Near You
Find trusted orthognathic surgery specialists at Medicover Hospitals across India in multiple locations. Choose your city to connect with experienced Dental surgeons for advanced jaw correction procedures, high success rates,and comprehensive patient care support.
Why Choose Medicover Hospitals for Jaw Surgery (Orthognathic)?
Get a second opinion from trusted experts and makeconfident, informed decisions.
Complete Guide to Orthognathic Surgery
Everything you need to know about the procedure, preparation, and recovery
What Are the Indications for Orthognathic Surgery (Jaw Surgery)?
Jaw surgery, or orthognathic surgery, is indicated for individuals whose jaw alignment or facial structure causes functional problems or aesthetic concerns. Your surgeon may recommend jaw surgery if you have:
- Severe Malocclusions (misaligned bite)
- Facial asymmetry
- Difficulty chewing or speaking
- Breathing difficulties, including obstructive sleep apnea
- Temporomandibular joint (TMJ) disorders
- Open bite, deep bite, overjet, or underjet
- Problems with lip closure
- Chronic jaw pain
- Impaired oral hygiene due to jaw misalignment
- Psychological impact due to appearance or facial imbalance
What Conditions Does Orthognathic Surgery (Jaw Surgery) Treat?
Jaw surgery addresses both functional and aesthetic concerns, including:
- Bite problems (overbite, underbite, open bite, deep bite)
- Misaligned jaws are causing difficulty with chewing, speaking, or swallowing
- Facial asymmetry affecting appearance or confidence
- TMJ disorders leading to jaw pain or restricted movement
- Breathing issues, including sleep apnea
- Lip closure problems affecting oral function
- Impaired oral hygiene due to jaw misalignment
When Would a Doctor Recommend Orthognathic Surgery (Jaw Surgery)?
A surgeon may recommend jaw surgery when:
- Orthodontic treatments alone are insufficient to correct the jaw alignment
- Jaw misalignment causes pain, difficulty chewing, speaking, or breathing
- There are significant aesthetic concerns affecting facial balance
- There is a history of trauma or congenital jaw abnormalities
- Conservative therapies for TMJ disorders or sleep apnea have failed
Who Is Orthognathic Surgery (Jaw Surgery) For?
Jaw surgery is suitable for individuals who:
- Have completed jaw growth (usually late teens or older)
- Experience functional problems due to jaw misalignment
- Have aesthetic concerns affecting self-esteem or social confidence
- Are medically fit to undergo surgery and follow postoperative rehabilitation
How Should I Prepare Before Orthognathic Surgery (Jaw Surgery)?
Preparation for orthognathic jaw surgery involves careful planning to ensure a safe and successful procedure. Key steps include:
- Consultation with Oral Surgeon: Meet with an oral and maxillofacial surgeon who specializes in jaw surgery to discuss your condition, treatment goals, and surgical plan.
- Orthodontic Assessment: If needed, work with an orthodontist for pre-surgical orthodontic treatment to align your teeth correctly before surgery.
- Medical Evaluation: Provide your full medical history, including current medications, allergies, and any chronic health conditions.
- Treatment Planning: Discuss the detailed surgical plan with your oral surgeon and orthodontist, including anticipated outcomes and recovery expectations.
What Tests Are Done Before Orthognathic Surgery (Jaw Surgery)?
Before jaw surgery, you may undergo several tests to ensure you are fit for surgery and to aid in precise surgical planning:
- Imaging Studies: X-rays, CT scans, or 3D scans to evaluate jaw structure and alignment.
- Dental Impressions and Models: To assess teeth positioning and bite.
- Blood Tests: To check overall health and detect any underlying conditions.
- Cardiac or Pulmonary Assessments (if needed): For patients with pre-existing conditions.
Should I Stop Eating, Drinking, or Taking Medicines?
Prior to orthognathic surgery, your surgical team will provide specific instructions:
- Fasting: Avoid eating or drinking for a set period before the procedure, usually 6-8 hours.
- Medications: Some medications, such as blood thinners, may need to be temporarily stopped. Always follow your surgeon's instructions carefully.
- Lifestyle Preparations: Avoid smoking and limit alcohol intake to improve healing and reduce complications.
What Happens Before Jaw Surgery?
Before jaw surgery, the surgical team will ensure everything is ready for a safe procedure:
- Final review of your treatment plan and imaging studies
- Confirmation of anesthesia suitability
- Preoperative instructions for fasting, hygiene, and medications
- Mental preparation and addressing any concerns or questions
Orthognathic or Jaw Surgery Procedure
Orthognathic surgery, or jaw surgery, is designed to correct structural issues in the jaw and face, improving function and appearance. It's a well-coordinated process involving detailed evaluation, orthodontics, and surgical precision.
Here's what the procedure typically involves:
- Comprehensive Evaluation: The process begins with thoroughly assessing the patient's condition. This includes detailed X-rays, scans, photographs, and dental impressions. These images help create a precise three-dimensional model of the patient's facial and jaw structures.
- Collaborative Treatment Planning: Oral and maxillofacial surgeons collaborate closely with orthodontists to develop a comprehensive treatment plan. The plan outlines the movements and adjustments required for the upper and lower jaws to achieve proper alignment.
- Orthodontic Preparation: Before the surgical phase, patients often undergo orthodontic treatment to align their teeth properly. Braces are used to position the teeth to complement the anticipated surgical changes.
- Surgical Procedure: On the day of surgery, the patient is placed under general anaesthesia. The oral and maxillofacial surgeon makes incisions inside the mouth, usually along the gum line, to access the jaw bones. Depending on the patient's specific needs, the surgeon may need to reposition the upper jaw, lower jaw, or both.
Upper Jaw Surgery (Maxillary Osteotomy)
This procedure targets the upper jaw to correct alignment, improve bite, and address facial symmetry issues. It's a key part of jaw surgery for many patients.
- The upper jaw is carefully separated from the skull, allowing the surgeon to reposition it based on the treatment plan.
- The jaw is secured in its new position using specialized surgical plates, screws, or wires that promote stability and healing.
Lower Jaw Surgery (Mandibular Osteotomy)
When the lower jaw is misaligned, mandibular osteotomy helps shift it into a healthier, more functional position. This improves bite and overall jaw harmony.
- Like upper jaw surgery, the lower jaw is cut and repositioned as needed.
- Surgical hardware is used to fix the jaw in its new alignment.
Closure and Healing
After surgery, careful closure and post-operative care are vital for healing. Recovery protocols help prevent complications and ensure the best outcomes.
- After the repositioning, the incisions are closed using dissolvable sutures.
- The surgical wounds are covered with gauze to aid in healing.
Who Performs Orthognathic Surgery (Jaw Surgery)?
Jaw surgery (orthognathic surgery) is performed by an oral and maxillofacial surgeon, a specialist trained in corrective jaw procedures.
Specialist Part of Orthognathic Surgery
Orthognathic surgery, a specialized and comprehensive procedure, involves a multidisciplinary approach that requires the expertise of various healthcare professionals.
Here are the critical specialists who are interested in treating orthognathic surgery:
- Oral and Maxillofacial Surgeon
- Orthodontist
- Dentist
- Prosthodontist
- Medical Anesthesiologist
- Radiologist
- Speech Therapist
- Nutritionist/Dietitian
- Psychologist/Counselor
- Otolaryngologist (ENT Specialist)
Choosing a surgeon experienced in orthognathic procedures is essential for optimal functional and aesthetic outcomes.
What Happens During Jaw Surgery?
The jaw surgery procedure steps typically include:
- Anesthesia: You are placed under general anesthesia so you remain unconscious and pain-free.
- Incisions: The surgeon makes precise incisions, usually inside the mouth to minimize visible scarring.
- Bone Adjustment: The upper jaw, lower jaw, or both are carefully repositioned to correct alignment.
- Stabilization: Plates, screws, or wires are used to hold the jaws in their new position.
- Closure: Incisions are sutured, and the mouth is cleaned to reduce infection risk.
- Post-Surgery Monitoring: You are taken to a recovery area for observation until anesthesia wears off.
The procedure corrects bite issues, improves facial symmetry, and can alleviate functional problems like difficulty chewing, speaking, or breathing.
Post-Surgery Care or Recovery Time After Orthognathic Surgery (Jaw Surgery)
The Jaw surgery recovery period is a crucial phase that requires patience, careful adherence to postoperative instructions, and support from your healthcare team and loved ones.
Here's what you can expect during the Jaw surgery recovery process:
- Hospital Stay: Depending on the complexity of the surgery, you might need to stay overnight in the hospital or surgical centre for observation and initial recovery.
- Swelling and Discomfort: Swelling and discomfort are common after orthognathic Jaw surgery. Cold compresses and prescribed pain medications can help manage these symptoms.
- Diet: Initially, your diet will be limited to soft foods or liquids. As healing progresses, you'll gradually transition to a regular diet.
- Oral Care: Maintaining good oral hygiene is essential. Follow your surgeon's instructions for rinsing and cleaning your mouth to prevent infections.
- Medications: Take prescribed medications as your surgeon directs, including pain relievers and antibiotics.
- Follow-up Appointments: Attend all scheduled follow-up appointments with your oral surgeon and orthodontist to monitor healing and progress.
Lifestyle Changes For Quick Recovery
After undergoing orthognathic surgery, specific lifestyle changes can help facilitate a smoother recovery process and optimize the procedure results. These temporary adjustments support your healing, comfort, and overall well-being.
Here are some lifestyle changes to consider:
- Dietary Adjustments: Start with a soft or liquid-based diet, gradually reintroducing solids as recovery permits.
- Oral Care: Maintain excellent oral hygiene to prevent infections and support healing.
- Medication Management: Adhere to prescribed medications for controlling pain, swelling, and discomfort.
- Equipment: Utilize any necessary equipment while paying attention to the equipment and the individual, such as wheelchairs and prostheses.
- Follow-Up Appointments: When possible, attend all necessary follow-up appointments to monitor progress and make adjustments as needed regularly.
- Physical Activity: Avoid vigorous physical activities initially and gradually incorporate light exercises.
- Sleeping Posture: For the first few weeks, try to sleep with your head elevated to minimize swelling.
- Speech and Communication: Speech may be temporarily affected, but everything will return to normal over time; consider speech therapy if needed.
- Stress Control: Managing stress and emotions can significantly influence health and recovery.
- Protect Incisions: Keep healing wounds from direct sunlight to prevent pigmentation changes.
- Hydration and Nutrition: Hydration and nutrition are also essential for recovery.
- Avoid Smoking and Drinking: Refrain from smoking and drinking, as they can interfere with the healing process.
- Regular Follow-up with the Orthodontist: Continue with orthodontic treatment for proper bite alignment post-surgery.
Benefits and Risks Associated with Orthognathic Surgery
Benefits of Orthognathic Surgery (Jaw Surgery)
- Corrects jaw alignment: Surgery addresses problems that can not be fixed with orthodontics alone.
- Improved function: Proper jaw alignment may make eating, speaking, and breathing easier.
- Enhanced appearance: Jaw surgery can significantly improve facial aesthetics by realigning the jaw.
Risks of Orthognathic Surgery (Jaw Surgery)
- Infection: As with any surgery, there is a risk of infection.
- Bleeding: Some bleeding is normal, but should be managed by the surgical team.
- Nerve damage: Temporary numbness around the jaw area is possible, though it resolves over time.
- Pain and swelling: These are common post-surgery side effects, but they generally subside with proper care.
How much can Orthognathic Surgery (Jaw Surgery) cost?
The jaw surgery cost in India ranges from Rs. 50,000 to Rs. 7,00,000, depending on the procedure and its complexity. A simple jaw implant may cost around Rs.1,00,000, while a double jaw surgery is much more expensive.
The price is influenced by the type of surgery (upper, lower, or double jaw), the complexity of correction needed, the surgeon's expertise, the hospital or clinic facilities, and the city where the surgery is performed.
Patient Success Stories
Real experiences from patients who regained their mobility and quality of life
""I had trouble chewing and speaking because of my jaw alignment. The doctors at Medicover performed corrective jaw surgery, and now my bite and smile feel completely normal.""
""My daughter underwent jaw surgery at Medicover, and the results have been life-changing. The doctors were very professional, and her recovery was smooth with regular follow-ups.""
""I chose Medicover for my jaw surgery, and I'm very happy with the outcome. The procedure went well, and I can eat and talk comfortably again.""
Frequently Asked Questions
1. Who is a candidate for orthognathic surgery?
Candidates include patients with jaw misalignment, bite issues, facial imbalance, or breathing problems. Specialists evaluate dental and skeletal structure before recommending surgery.
2. Is orthognathic surgery painful?
Jaw surgery is performed under general anesthesia, so no pain is felt during the procedure. At Medicover Hospitals, post-surgery discomfort is managed effectively with medications.
3. Will I have visible scars after jaw surgery?
Most orthognathic surgeries are done inside the mouth, so no visible scars are seen externally. Healing is usually smooth with minimal cosmetic concerns.
4. Will I need braces before and after surgery?
Yes, braces are often required before and after surgery to align teeth properly. Orthodontic treatment ensures the best functional and aesthetic results.
5. What type of anaesthesia is used for jaw surgery?
Orthognathic surgery is performed under general anesthesia, ensuring the patient is completely unconscious and comfortable during the procedure.
6. Can orthognathic surgery improve my breathing and speech?
Yes, jaw surgery can improve breathing issues like sleep apnea and correct speech problems by aligning the jaw properly for better airway function.
7. How long will I be in the hospital after orthognathic surgery?
Patients typically stay in the hospital for 1 to 3 days after surgery. At Medicover Hospitals, recovery is closely monitored for safe and smooth healing.
8. Will my appearance change after jaw surgery?
Yes, orthognathic surgery improves facial balance and symmetry. Changes are usually positive, enhancing both appearance and functional alignment.
9. Are there risks associated with orthognathic surgery?
Risks include swelling, infection, numbness, or bleeding. At Medicover Hospitals, experienced surgeons use advanced techniques to minimize complications.
10. Can I resume normal activities after orthognathic surgery?
Most patients resume light activities within 2 weeks, while full recovery may take a few months. Following medical advice helps ensure proper healing.
11. How successful is jaw surgery?
Orthognathic surgery has high success rates in correcting jaw alignment and improving function. Long-term results are stable with proper orthodontic support.
12. Is jaw surgery a serious surgery?
Yes, jaw surgery is a major procedure requiring careful planning and expertise. However, it is commonly performed safely with good outcomes in specialized centers.
13. How long is bed rest after jaw surgery?
Strict bed rest is not usually required. Patients are encouraged to move gently after a few days, while avoiding strenuous activities for several weeks.
14. Does jaw surgery change your voice?
Jaw surgery may slightly affect voice temporarily due to swelling, but it usually returns to normal. In some cases, speech clarity may even improve.
15. What should I avoid after jaw surgery?
Avoid hard foods, smoking, alcohol, and strenuous activities after surgery. Following dietary and care instructions helps ensure faster healing and better results.