Ulcerative Colitis (UC): Symptoms and Treatment
Ulcerative colitis is caused by the alteration in the response of the immune system. Usually, the immune system attacks the intruders in the body like microorganisms causing the common cold. However, in this case, the immune system considers the food, the cells that line the colon, and the gut bacteria as the intruders and attacks them, which are actually needed for the body. It causes inflammation and ulcers in the inner lining of the colon.
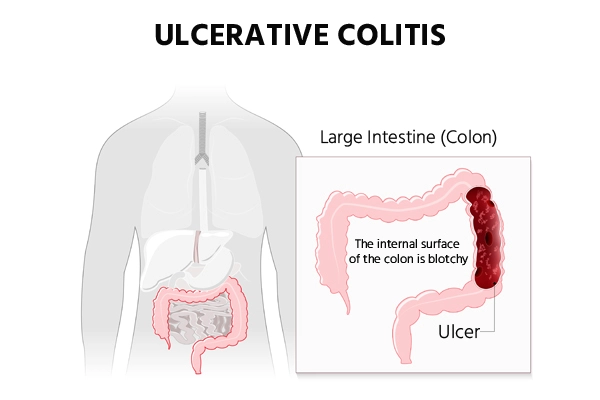
Types of Ulcerative colitis
- Ulcerative proctitis : This is the mildest form, caused only in the rectum. The bleeding in the rectum may be the only sign of this type of ulcerative colitis.
- Proctosigmoiditis : It occurs in the rectum and the lower end of the colon. Blood diarrhea, stomach cramps and the consistent urge to poop are some of its symptoms.
- Left-sided colitis : This condition is caused by the inflammation in the rectum, up to the left side of the colon and it causes severe cramps on that side of the stomach. Bloody diarrhea and losing weight without trying are the symptoms of this condition.
- Pancolitis : It affects the entire colon, causing bloody diarrhea, severe belly cramps, fatigue, and major weight loss.
- Acute severe ulcerative colitis : It is quite rare, but like pancolitis, it affects the entire colon, with heavy diarrhea, severe pain, bleeding, and fever.
Symptoms of Ulcerative colitis
The most common symptom of ulcerative colitis is bloody diarrhea; some may observe pus in their stools too. This disease belongs to a group of conditions called inflammatory bowel disease(IBD). The symptoms include:
- Diarrhea
- Abdominal cramps
- Weight loss
- Anemia
- Nausea
- Sudden urge to poop
- Fever
- Dehydration
- Skin sores
- Loss of fluids and nutrients
- Mucus and pus in the bowels
When to see a doctor?
If you think you may have ulcerative colitis and are experiencing any of the following symptoms, it’s important to see a doctor right away:
- Severe abdominal pain that lasts more than 24 hours. Delaying treatment could be dangerous.
- Thick blood in your stool during a bowel movement.
- Fever along with severe abdominal pain.
- Severe diarrhea with rectal bleeding.
For the best care, visit Medicover Hospitals and get treated by an experienced Gastroenterologist.
Causes of Ulcerative Colitis
The ulcerative colitis causes are not fully understood. While diet and stress were once thought to be causes, we now know they may only make the condition worse, not cause it. IfPossible causes include:
- Immune system issues: Ulcerative colitis may result from a problem with the immune system. When it tries to fight off infections, it may directly attack the cells in the digestive tract instead.
- Genetics: Certain genetic factors have been linked to ulcerative colitis, and it tends to run in families. People with family members who have the condition may be more likely to develop it themselves.
Get a second opinion from trusted experts and makeconfident, informed decisions.
Risk Factors
Ulcerative colitis might also additionally boom the chances of body and mental fitness complications, such as:
- Arthritis
- Pores and skin problems
- Eye inflammation
- Liver and kidney problems
- Bone loss
- Stress
- Depression
Complications
Ulcerative colitis complications may include :
- Severe bleeding
- A hole in the colon
- Dehydration
- Anemia (low red blood cell count)
- Bone loss (osteoporosis)
- Inflammation in the skin, joints, and eyes
- Increased risk of colon cancer
- Toxic megacolon (rapidly swelling colon)
- Higher risk of blood clots
- Delayed growth in children
It's essential to manage the condition properly to reduce the risk of these complications.
Diagnosis of Ulcerative Colitis
To diagnose ulcerative colitis (UC), your doctor will ask about your symptoms and inquire about your family history of inflammatory bowel disease (IBD). They’ll also order some tests and procedures to rule out other conditions that may cause similar symptoms.Here are the tests and procedures that may be used:
- Blood tests: The signs of anemia, which may indicate bleeding in the colon or rectum. Blood tests can also help identify other possible causes of your symptoms, like an infection.
- Stool samples: Your stool may be tested to look for signs of infection, parasites, or inflammation.
- Imaging tests: Doctors may order an X-ray, CT scan and MRI to get a clearer picture of your colon and rectum. These tests help show inflammation and complications like megacolon (a swollen colon) or perforation (a hole in the colon).
- Endoscopic tests: These use a thin, flexible tube with a small camera to look inside your colon. Your doctor may insert the tube through your rectum to take a closer look and collect tissue samples for testing (biopsy).
These tests help your doctor determine if you have UC and rule out other possible conditions.
Treatment for Ulcerative colitis
Ulcerative colitis treatment often involves surgery, depending on the severity of the condition. Different types of medications can be effective, but the right one for you will depend on how severe your symptoms are. Since what works for one person may not work for another, it may take some time to find the right treatment. It's also important to consider the potential benefits and risks of each treatment, as some medications may have significant side effects.
Medications
- Anti-inflammatory drugs: These are usually the first treatment and include corticosteroids, which help reduce inflammation.
- Immune system suppressors: These help lower inflammation by blocking the immune response that causes it. Sometimes a combination of these drugs is more effective.
- Other medications: You may also need medications for specific symptoms, such as anti-diarrheal drugs, pain relievers, antispasmodics, or iron supplements. Always consult your doctor before taking any over medications.
Surgery
If medications don’t work, Ulcerative colitis surgery may be necessary. One option is proctocolectomy, where the colon and rectum are removed. A pouch is formed from the small intestine and attached to the anus for waste elimination. If this isn’t possible, an ileal stoma may be created, with a bag attached to collect waste.
Lifestyle changes and self care
Managing ulcerative colitis can feel challenging, but making some lifestyle changes can help control symptoms and reduce flare-ups. While diet doesn’t cause the condition, certain foods and drinks can trigger symptoms, especially during flare-ups.Here are some tips for better managing your condition:
- Limit dairy: Dairy can cause diarrhea, stomach pain, and gas for many people with IBD. If you’re lactose intolerant, try using Lactaid or other enzyme supplements.
- Eat smaller meals: Eat 5–6 smaller meals throughout the day instead of 2–3 large ones.
- Stay hydrated: Drink plenty of water daily. Avoid drinks, alcohol, and caffeine, as they can irritate your intestines and worsen diarrhea.
Tracking what you eat and how it affects you can help identify triggers and improve your overall management.
Your health is everything - prioritize your well-being today.
Do's and Don’ts
A person with Ulcerative Colitis has to follow sets of do’s and don’ts to manage it and related symptoms and risks:
|
Do’s |
Don’ts |
|---|---|
|
Do’s |
Don’ts |
|
Eat small meals in a day. |
Consume more than 2 cups of milk, cottage cheese, pudding, or yoghurt per day |
|
Drink a lot of water and stay hydrated. |
Consume frozen and processed meats |
|
Take proper rest. |
Consume raw vegetables with high fibre content. |
|
Some regular exercises or yoga. |
Consume spicy sauces, pickles, etc. |
|
Take your medications on time. |
Consume foods and beverages that contain caffeine, cocoa, and alcohol |
Care at Medicover Hospitals
At Medicover Hospitals, we have the most trusted team of doctors and medical experts who provide excellent healthcare services to patients with compassion and care. Our diagnostic department is equipped with modern technology and equipment to conduct all the tests required for Ulcerative Colitis diagnosis, based on which a dedicated treatment plan is designed. We have an excellent team of Gastroenterologists and gastro surgeons who diagnose and treat this condition with utmost precision that brings successful treatment outcomes.
Frequently Asked Questions
Is ulcerative colitis an autoimmune disease?
Ulcerative colitis is like when your body's defence system, called the immune system, gets a bit confused and starts attacking the inside of your colon and rectum. This causes swelling and other problems in your tummy.
What is the ulcerative colitis treatment?
When you have ulcerative colitis, doctors can use medicines to improve the swelling, handle how you feel, and even slow down your immune system. Sometimes, if things are serious, they might even do an operation to take out the part of your colon causing trouble.
Why do ulcerative colitis occur?
We're still figuring out the exact reason why ulcerative colitis happens. It seems like a mix of things, like genes you inherit, stuff in your environment, and how your immune system works. Sometimes, certain things can set off your immune system to attack your tummy, causing problems.
Can ulcerative colitis cause cancer?
Ulcerative colitis patients have a slightly increased risk of developing colon cancer, especially if the disease is long-standing and involves a more significant portion of the colon. Regular monitoring and appropriate medical care can help manage this risk.
What is the meaning of ulcerative colitis?
Ulcerative colitis is a long-lasting problem that makes the inside of your colon and rectum all swollen and sore. It's a sickness where you get ulcers and swelling in these parts of your tummy.
What are the ulcerative colitis symptoms in females?
Girls and boys can both have the same signs of ulcerative colitis. This might mean tummy pain, going to the bathroom a lot, bleeding from the bottom, losing weight, and feeling tired. Sometimes, the symptoms might change a bit when girls have their periods.
What are the Ulcerative colitis foods to avoid?
Some foods can make things worse if you have ulcerative colitis. Spicy stuff, foods with lots of fibre, dairy like milk and cheese, caffeine, and even drinks with alcohol can be tricky. Making a particular eating plan that works just for you is a good idea. Your doctor can help you with that.
Where is the pain located in ulcerative colitis?
Pain in ulcerative colitis can vary, but it's often in the lower abdomen, especially on the left side. Pain might also be accompanied by cramping and discomfort.
What is ulcerative colitis radiology?
Doctors sometimes use unique picture-taking methods, like X-rays, CT scans, and MRIs, to see how bad the swelling and problems are in the colon and rectum of people with ulcerative colitis. These pictures help the doctors decide how to help you feel better.