Lupus: Causes, Symptoms & Treatment Options
Lupus is a condition in which the body's immune system attacks its own tissues and organs (called autoimmune disease). Lupus can cause inflammation in the joints, skin, kidneys, blood cells, brain, heart, and lungs, among other physiological systems.
Lupus is difficult to diagnose since its symptoms and signs are often similar to those of other illnesses. The most distinguishing symptom of lupus is a face rash that looks like butterfly wings unfolding over both cheeks. This rash appears in many but not all cases of lupus.
Types of Lupus
There are several types of lupus, each with unique symptoms and characteristics. Here's an overview:
Systemic Lupus Erythematosus (SLE)
This is the most common type of lupus and can affect multiple organs and systems in the body, including the skin, joints, kidneys, heart, lungs, and brain.
- Symptoms: Fatigue, joint pain, skin rashes (like the butterfly rash), and organ inflammation.
- Severity: Ranges from mild to severe, with flare-ups and periods of remission.
Cutaneous Lupus Erythematosus (CLE)
This form of lupus is limited to the skin and includes three subtypes:
- Acute CLE: Often associated with SLE; includes the butterfly rash on the face.
- Subacute CLE: Red, scaly, or ring-shaped lesions on sun-exposed areas.
- Chronic CLE (Discoid Lupus): Thick, scaly patches that can cause scarring, often on the face and scalp.
Drug-Induced Lupus (DIL)
This type of lupus is triggered by certain medications and mimics symptoms of SLE.
- Symptoms: Joint pain, muscle pain, fever, and fatigue.
- Common Drugs: Hydralazine, procainamide, and isoniazid are known triggers.
- Prognosis: Symptoms usually resolve once the medication is discontinued.
Neonatal Lupus
This rare type occurs in newborns of mothers with certain autoantibodies.
- Symptoms in Babies: Skin rashes, liver problems, and low blood cell counts. In rare cases, it can cause congenital heart block.
- Prognosis: Symptoms typically disappear within a few months after birth.
Lupus in Overlap Syndromes
In some cases, lupus overlaps with other autoimmune diseases, such as:
- Mixed Connective Tissue Disease (MCTD): Features of lupus, scleroderma, and polymyositis.
- Rheumatoid Arthritis or Sjögren’s Syndrome: Where lupus symptoms coexist with these conditions.
Drug-Induced Subacute Cutaneous Lupus
A subtype of CLE caused by medications that leads to sun-sensitive rashes without systemic involvement.
Get a second opinion from trusted experts and makeconfident, informed decisions.
Symptoms of Lupus
There are no two cases of lupus that are the same. Symptoms and signs might appear abruptly or gradually, be moderate or severe, and be transitory or permanent. Most people with lupus have a moderate form of the disease marked by flares, which occur when signs and symptoms worsen for a period of time before improving or perhaps disappearing completely.
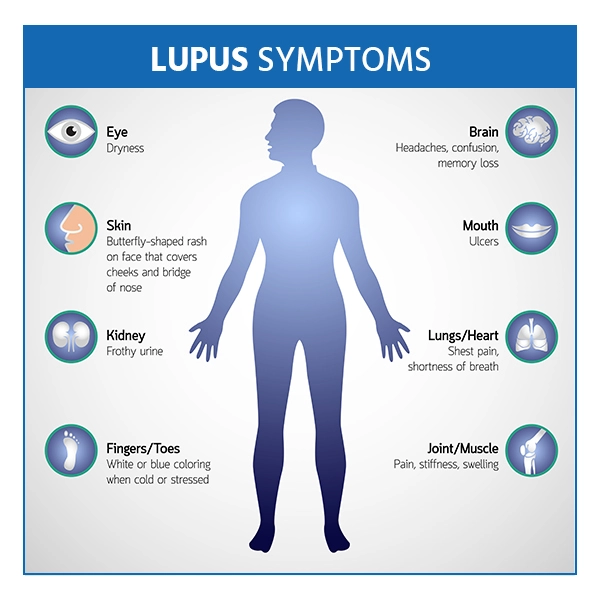
Your lupus signs and symptoms will vary depending on which body systems are affected by the condition. The following are the most common signs and symptoms:
- Fatigue
- Fever
- Joint pain
- Skin lesions
- Fingers and toes turn white or blue when exposed to cold
- Breathlessness
- Chest pain
- Dry eyes
- Headaches
- Memory loss
Nerve damage symptoms
- Peripheral neuropathy deals with tingling, numbness, or weakness in the extremities.
- Cranial neuropathy deals with facial paralysis, double vision, or other problems with eye movement or facial sensation.
- Autonomic neuropathy deals with dizziness, fainting, abnormal sweating, or digestive issues.
- Central nervous system involvement deals with headaches, seizures, cognitive dysfunction, memory problems, mood changes, or psychosis.
Causes of Lupus
Lupus is an autoimmune illness in which the immune system assaults healthy tissue in the body. Lupus is most likely caused by a mix of your genetics and your environment. It indicates that people who have a hereditary susceptibility to lupus may get the disease if they come into contact with a trigger in the environment. However, in the vast majority of instances, the cause of lupus is unknown.
The following are some possible triggers:
- Sunlight: For a person with lupus, exposure to the sun might cause skin lesions.
- Infections: Infections can trigger lupus.
- Medications: Certain blood pressure drugs, anti-seizure medications, and antibiotics can all cause lupus.
Other Problems Can Lupus Cause
Lupus can lead to a variety of other health problems, including:
- Kidney Damage (Lupus Nephritis): Inflammation of the kidneys, which can lead to kidney failure if untreated.
- Heart Disease: Increased risk of heart attacks, strokes, and other cardiovascular issues.
- Lung Issues: Inflammation of the lungs, leading to breathing difficulties, pleuritis, or even pulmonary hypertension.
- Neurological Problems: Seizures, headaches, memory issues, or even strokes.
- Blood Clotting: Increased risk of blood clots, which can lead to deep vein thrombosis (DVT), pulmonary embolism, or strokes.
- Anemia: Lupus can cause a decrease in red blood cells, leading to fatigue and weakness.
- Increased Infections: Due to a weakened immune system from both the disease and medications like steroids.
Risk Factors of Lupus
The following factors may raise your lupus risk:
- Women are more likely to develop lupus.
- Lupus can affect people of any age; however, it is most commonly diagnosed in people between the ages of 15 and 45.
Your health is everything - prioritize your well-being today.
Diagnosis of Lupus
Lupus is difficult to diagnose because indications and symptoms differ greatly from person to person. Lupus symptoms might fluctuate over time and overlap with those of various other illnesses. Lupus cannot be diagnosed with a single test. Instead, it is diagnosed using a combination of blood and urine testing, signs and symptoms, and physical examination findings.
The following tests may be performed on your blood or urine:
- Complete blood count: This test determines the number of red blood cells, white blood cells, and platelets, as well as the amount of hemoglobin, a protein contained in red blood cells. The findings could indicate that you have anemia, which is common in lupus patients. A decreased white blood cell or platelet count is another symptom of lupus.
- Erythrocytes Sedimentation Rate: This blood test determines how quickly red blood cells drop to the bottom of a tube in one hour. A higher-than-normal rate may indicate a systemic disease such as lupus. The rate of sedimentation isn't exclusive to any one condition. It may be elevated if you have lupus, an infection, another inflammatory illness, or cancer.
- Test of the kidneys and liver: Blood tests can be used to determine how well your kidneys and liver are working.
- Urinalysis: A test of a sample of your urine may reveal an elevated protein level or red blood cells in the urine if your kidneys have been damaged by lupus.
- Test for antinuclear antibodies (ANA): A positive test for these antibodies, which your immune system produces, indicates that your immune system is activated. While the majority of people with lupus have a positive ANA test, the majority of those without lupus do not. If you test positive for ANA, your lupus doctor may offer more specific antibody testing.
If your doctor feels that lupus is damaging your lungs or heart, he or she may recommend the following Imaging test:
- X-ray of the chest: Abnormal shadows in your chest picture could indicate fluid or inflammation in your lungs.
- Echocardiogram: Sound waves are used to create real-time photographs of your beating heart in this exam. It can look for abnormalities with your heart's valves and other parts.
- Biopsy: Lupus can damage your kidneys in a variety of ways and therapies vary depending on the severity of the damage. In some circumstances, a small sample of kidney tissue must be tested to establish the best treatment option. A needle or a minor incision might be used to acquire the sample.
Lupus Treatment
Treatment options for lupusaim to manage symptoms, reduce inflammation, and prevent flare-ups. Here are the key treatments:
Medications
- Nonsteroidal Anti-Inflammatory Drugs (NSAIDs): For pain and inflammation relief.
- Antimalarial Drugs: Medications like hydroxychloroquine (Plaquenil) can help control lupus symptoms, especially skin and joint problems.
- Corticosteroids: Prednisone is often prescribed to reduce inflammation and prevent flare-ups.
- Immunosuppressants: Medications like azathioprine and methotrexate are used to suppress the immune system and prevent it from attacking healthy tissues.
- Biologic Drugs: Belimumab (Benlysta) is an FDA-approved biologic drug that helps reduce disease activity by targeting specific immune system components.
Lifestyle Changes of Lupus
By adopting the following lifestyle changes, you can help manage and Prevent the risk of lupus flare-ups.
- Diet: Eating a healthy, well-balanced diet rich in fruits, vegetables, and whole grains can help support overall health.
- Exercise: Regular, low-impact exercises can improve joint health and overall well-being.
- Sun Protection: Using sunscreen and wearing protective clothing can help prevent lupus flare-ups, especially for those with skin symptoms.
- Physical Therapy: Physical therapy can help strengthen muscles and maintain joint mobility, reducing pain and stiffness.
- Psychological Support: Support groups or therapy may be helpful for managing the mental health aspects of lupus, including stress, anxiety, or depression.
- Regular Monitoring: Frequent medical checkups and lab tests to monitor kidney, liver, and heart function, as lupus can affect various organs.
Frequently Asked Questions
Is lupus a dangerous illness?
SLE can range in severity from mild to potentially fatal. A physician or group of physicians with expertise in treating individuals with SLE should be in charge of treating the illness. People who get appropriate medical attention and preventative treatment for lupus
What are the early signs of lupus in females?
Some of the Common symptoms include fatigue, hair loss, sun sensitivity, painful and swollen joints, unexplained fever, skin rashes, and kidney problems.
What are the early signs of lupus in males?
Early signs of lupus in males may include fatigue, joint pain, skin rashes, fever, sensitivity to sunlight, chest pain, and hair loss.
Can lupus disease be treated and cured?
Lupus has no cure, but treatments manage symptoms and prevent flare-ups. Medications like NSAIDs, corticosteroids, and immunosuppressants help. Lifestyle changes, stress management, exercise, and a healthy diet also aid symptom control, enabling many to lead fulfilling lives.
Does lupus cause cancer?
Lupus doesn't directly cause cancer, but long-term use of certain medications and immune system dysfunction can slightly elevate cancer risk. Regular monitoring and discussions with healthcare providers help manage these risks effectively.
What foods make lupus worse?
Foods that potentially worsen lupus include nightshade veggies (tomatoes, potatoes), alfalfa, excessive salt, saturated/trans fats, sugar, alcohol, and processed foods. These can trigger inflammation and exacerbate symptoms like joint pain, swelling, and fatigue.
What is the lupus life expectancy?
With proper treatment and management, individuals with lupus can live a normal or near-normal life expectancy. However, the life expectancy can vary depending on the severity of the disease, organ involvement, and response to treatment.