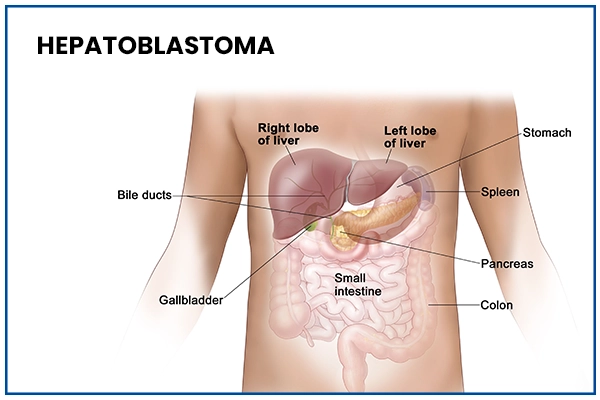
Hepatoblastoma: Overview
Hepatoblastoma is a rare type of paediatric
liver cancer
generally diagnosed in one in a million children aged under three years. The exact cause of hepatoblastoma is not known. But, certain risk factors are associated with the condition, such as having a genetic syndrome or a family history of liver cancer. Usually, hepatoblastoma is a severe condition and requires early diagnosis and immediate treatment. In addition, children with this condition should receive ongoing medical care and monitoring depending on the histology of the tumour to ensure the best positive outcomes.
Treatment for hepatoblastoma typically involves a combination of surgery, chemotherapy, and radiation therapy. The goal of treatment is to remove the tumour and any surrounding tissues that may be affected by cancer. The prognosis for hepatoblastoma varies depending on the tumour stage at diagnosis, but early detection and timely treatment can significantly improve the chances of survival.
Get a second opinion from trusted experts and makeconfident, informed decisions.
 Get Second Opinion
Get Second Opinion
Types
There are two types of hepatoblastoma, each with different characteristics, including:
-
Fetal type: This type accounts for about two-thirds of all hepatoblastomas. It is characterized by cells that resemble fetal liver cells. Fetal-type hepatoblastomas tend to be less aggressive and have a better prognosis.
-
Embryonal type: This type accounts for about one-third of all hepatoblastomas. It is characterized by cells that resemble the embryonal liver cells. Embryonal-type hepatoblastomas tend to be more aggressive and have a poorer prognosis.
Risk factors
Most cases of hepatoblastoma occur in children with no known risk factors. However, there are a few well-known risk factors for hepatoblastoma, which include:
- Rare genetic syndromes: Certain genetic conditions such as Beckwith-Wiedemann syndrome, familial adenomatous polyposis, and hereditary non-polyposis colorectal cancer were associated with an increased risk of developing hepatoblastoma.
- Exposure to infectious agents: Children exposed to the hepatitis B or hepatitis C virus during the early days of life have an increased risk of developing hepatoblastoma.
- Low birth weight: Children who are born with a low birth weight have a slightly higher risk of developing hepatoblastoma.
- Family history: Children with a positive family history of hepatoblastoma have a higher risk of developing the condition.
- Prematurity: Babies born prematurely have an elevated risk of developing hepatoblastoma compared to those born full-term.
Causes
The exact causes of hepatoblastoma are not well understood, but it is believed that a combination of environmental and genetic factors may increase the risk of developing this hepatoblastoma. Some of the potential causes include:
- Genetic mutations: Children with specific genetic mutations, including APC, AXIN1, and CTNNB1, increased risk of hepatoblastoma.
- Environmental toxins: Exposure to environmental toxins like aflatoxins or vinyl chloride could increase the risk of hepatoblastoma.
- Viral infections: Infection with hepatitis B or hepatitis C virus during the prenatal period or after birth may induce hepatoblastoma.
Symptoms
Symptoms of hepatoblastoma can vary depending on the tumour size, the tumour location and whether the cancer cells have metastasized or spread to other body organs. However, some common symptoms of hepatoblastoma include the following:
- Painful abdominal lump
- Persistent nausea and vomiting
- Abdominal pain
- Fever
- Loss of appetite
- Unexplained weight loss
- Jaundice
- Pale or light grey or white stools due to bile flow obstruction by the tumour.
- Dark brown or tea-coloured urine due to excessive bile excretion.
- Fatigue or easy tiredness.
- Itchy skin: Excessive toxin accumulation in the body because of compromised liver function causes skin issues in patients with hepatoblastoma.
- Increased hepatic arterial pressure.
- Enlarged veins on the abdominal skin
Diagnosis
The general diagnostic tests used in the diagnosis of hepatoblastoma include the following:
- Alpha-fetoprotein test: Increased levels of Alpha-fetoprotein levels in the child's blood may indicate the presence of tumours in the liver.
- Comprehensive metabolic panel: Combination of blood tests that estimate the levels of 14 different substances that indicate liver function.
- Vascular ultrasound: To view changes in the blood vessel network that enter and leave the liver.
- Complete blood count: This test analyses the complete blood cell morphology, count, and levels of different essential substances in the blood.
- Liver ultrasound and Doppler ultrasound: To view the abnormalities in the liver.
- MRI: To clearly view the lumps or other structural abnormalities in the liver.
- PET scan: This test helps to examine the whole body for the presence of metastasized tumours.
- Tumour biopsy: A sample tissue of the tumour was taken using a needle and should be examined under the microscope. This test will help to explore the tumour cells and differentiate the type of tumour for better treatment.
Treatment
Treatment for hepatoblastoma depends on various factors like -
- The child's age
- The size of the tumour,
- Number of tumours present,
- Location of the tumour in the liver
- Whether the cancer cells spread from the liver to other organs or not.
Usually, hepatoblastoma can be treated by partial hepatectomy in which some portion of the liver containing tumours is removed. Sometimes partial hepatectomy may combine other treatments, which include:
- Chemotherapy: These are effective medicines that kill cancer cells. They may be administered before or after surgery. They are delivered orally or intravenously or intramuscularly. Some anticancer medication may also be directly delivered to the liver by accessing the liver's main artery through a catheter.
- Transarterial chemoembolization: This procedure involves the injection of anticancer drugs into an artery that supplies blood to the liver, followed by the injection of another substance to block that artery. This process helps to keep the anticancer drugs inside the tumours for a longer duration.
- Radiation therapy: Used to treat tumours that can not be removed by surgery. Radiation therapy can also be done after surgical removal of the tumours to kill the leftover cancer cells.
- Ablation therapy: This treatment is used to treat recurring tumours.
-
Liver transplantation:
This procedure is recommended when the child has large or multiple tumours.
Complications
Some of the complications are as follows:
- Increased risk of infections after surgical treatment.
- Loss of blood and bleeding from surgery
- Skin bruising, bleeding, nausea, vomiting, hair loss, diarrhoea, and tiredness with some chemotherapy medicines.
- Growth and developmental abnormalities
- Problems with liver function
- Spread of cancer to other organs (metastasis)
- Recurrence of tumours
- Growth of new cancers
- Organ rejection reactions after liver transplantation
- Problems with anti-rejection medicines
Precautions to be taken during and after treatment
- A child might feel very tired during treatment. Therefore, parents should ensure that their children get the proper amount of rest and activity.
- Utilise timely hospital visits even after the tumour has been completely cured.
- Provide physical and mental support to the child.
- Call the healthcare provider when a child has worsening symptoms, new symptoms, fever and any side effects from the treatment.
Care at Medicover Hospitals
At Medicover Hospitals, we have the most trusted group of oncologists and healthcare professionals skilled at providing the best medical treatment to patients while showing compassion and care. Our diagnostic department is equipped with state-of-the-art technology and equipment to conduct the necessary investigations for diagnosing hepatoblastoma. Our outstanding team comprises paediatricians, oncologists, and other specialists who use a systematic and multidisciplinary approach to diagnose and treat this condition.