What is COPD?
- COPD (chronic obstructive pulmonary disease) is a lung condition that causes shortness of breath and a persistent cough.
- Although this progressive lung disorder has no cure, it may be treated (and its progression slowed) by following appropriate measures and working closely with your doctor.
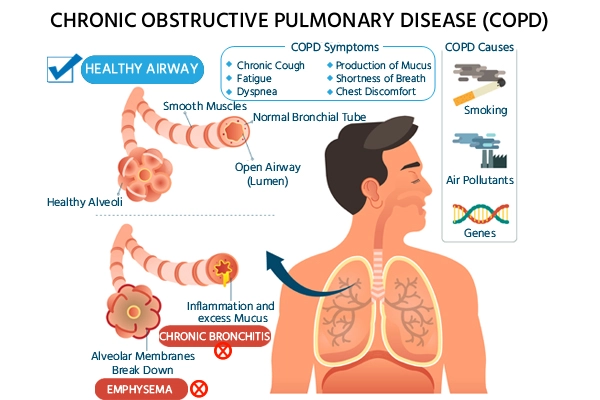
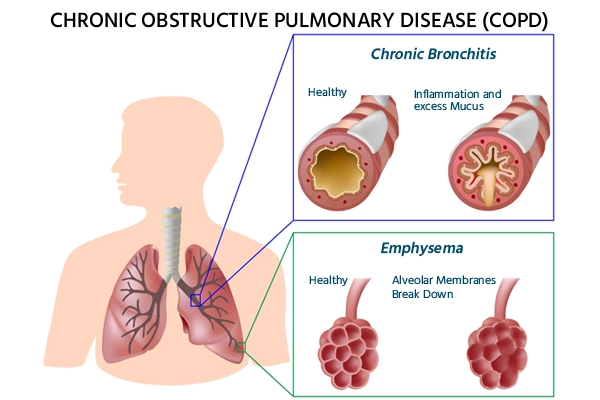
- Emphysema and chronic bronchitis are the two most common conditions found in patients with COPD.Emphysema obstructs airflow by gradually damaging the air sacs in the lungs.
- Bronchitis is characterized by inflammation and constriction of the bronchial passages, allowing mucus to accumulate. COPD, if left untreated, can lead to quicker disease progression, cardiac difficulties, and severe respiratory infections.
Get a second opinion from trusted experts and makeconfident, informed decisions.
 Get Second Opinion
Get Second Opinion
What are the Symptoms of COPD?
It makes breathing difficult. At first, the symptoms may be mild, with occasional coughing and shortness of breath. Symptoms might grow more consistent as time goes on, making breathing extremely difficult.
What are the Early Symptoms of COPD?
COPD symptoms might be quite mild at first. They might be mistaken for a cold. It involves
- Shortness of breath on occasion, especially after exertion.
- Cough that is mild but recurring.
- Frequently clearing your throat, particularly first thing in the morning.
Find Our Specialists
What are the Worsening symptoms of COPD?
Symptoms might become increasingly severe and difficult to ignore. You may have symptoms as your lungs get increasingly damaged.
- Even mild forms of exercise, such as going up a flight of stairs, can cause shortness of breath.
- Wheezing is a form of higher-pitched loud breathing that occurs often during exercise.
- Exhalations
- Tightness in the chest
- Coughing for a long time, with or without mucous
- Need to clear mucus from your lungs every day
- Colds, flu, or other respiratory diseases regularly
- Energy deficiency In later stages of COPD, symptoms may also include:
- Fatigue
- Swelling of the feet, ankles, or legs
- Weight loss
What are the Causes of COPD?
The majority of people with COPD are at least 40 years old or have a history of smoking. The longer people smoke and the more tobacco products people consume, the more likely they develop the condition. In addition to cigarette smoking, It can be caused by cigar smoke, pipe smoke, and secondhand smoke. If you smoke and have asthma, your chances of developing COPD are significantly higher.
- Passive smoking
- Indoor cooking with poor ventilation
- Air pollution
- Exposure to chemicals
- Exposure to industrial dust and fumes
- Intravenous drug abuse
- Infections, such as HIV
- Genetic disorders, such as Marfan syndrome and alpha1-antitrypsin deficiency
What are the Risk factors of Chronic Obstructive Pulmonary Disease?
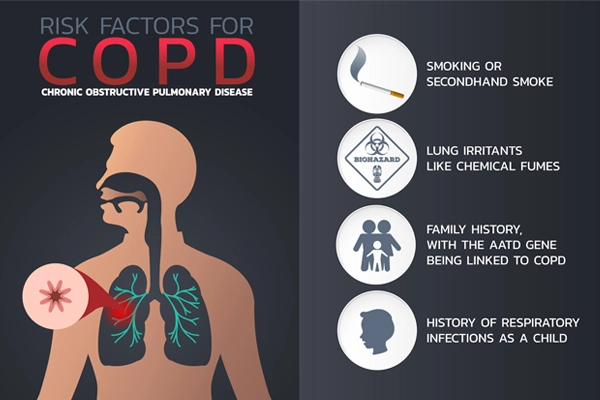
It has several risks, including
- Smoking: This is the most significant risk factor. COPD affects up to 75% of those who smoke or are used to smoking.
- Long-term exposure: To additional lung irritants from the environment or workplace, such as secondhand smoke, air pollution, chemical fumes, and dust.
- Age: When COPD symptoms first appear, most patients are at least 40 years old.
- Genetics: This covers the hereditary disorder alpha-1 antitrypsin deficiency. Smokers who develop COPD are also more prone to do so if they have a family history of the disease.
- Asthma: Asthmatics are more likely to acquire COPD than persons who do not have asthma. However, most asthmatics do not get It.
What are the Diagnosis of Chronic Obstructive Pulmonary Disease?
Your doctor will ask about your COPD signs and symptoms, your medical history, and whether you smoke or have been exposed to chemicals, dust, or smoke at work. They’ll also do a physical exam and breathing tests. Let them know if you have an ongoing cough.
The most common test is called spirometry. You’ll breathe into a large, flexible tube that’s connected to a machine called a spirometer. It’ll measure how much air your lungs can hold and how fast you can blow air out of them.
Your doctor may order other tests to rule out other lung problems, such as asthma or heart failure. These might include.
- More lung function tests
- Chest X-rays that can help rule out emphysema, other lung problems, or heart failure
- CT scan, which uses several X-rays to create a detailed picture of your lungs and can tell the doctor if you need surgery or if you have lung cancer
- Arterial blood gas test, which measures how well your lungs are bringing in oxygen and taking out carbon dioxide
- Laboratory tests to determine the cause of your symptoms or rule out other conditions, like the genetic disorder alpha-1-antitrypsin (AAT) deficiency
What are the Treatments for Obstructive Pulmonary Disease?
Because there is no cure, the purpose of treatment is to alleviate the symptoms and slow the progression of the condition. In addition, the doctor will work to prevent or treat any other complication and improve the overall quality of life. Giving up smoking is one of the best things you can do to keep your COPD from worsening.
Medical treatment for COPD:
The medical treatment includes:
- Bronchodilators: These medications are inhaled. They aid in the opening of your airways.
- Corticosteroids: These medications help to minimise airway inflammation. They might be inhaled or taken as tablets.
- Combination inhalers: Steroids and a bronchodilator are included in these inhalers.
- Antibiotics: These may be prescribed by the doctor to treat bacterial infections.
- Roflumilast(Daliresp): This medication inhibits an enzyme known as PDE4. It prevents flare-ups in persons with COPD who also have chronic bronchitis.
- Flu or pneumonia vaccines: These immunizations reduce the risk of respiratory infections such as COVID-19.
- Pulmonary rehabilitation: To help you stay as healthy and active as possible, this programme combines exercise, illness management, and counselling.
- Oxygen therapy: You may require this to alleviate shortness of breath, protect your organs, and improve your overall quality of life.
In severe cases of COPD, your doctor may suggest
- Bullectomy: Removes bullae, large air spaces that form when air sacs collapse
- Lung volume reduction surgery: Removes diseased lung tissue
- Lung transplant: Replaces a diseased lung with a healthy one