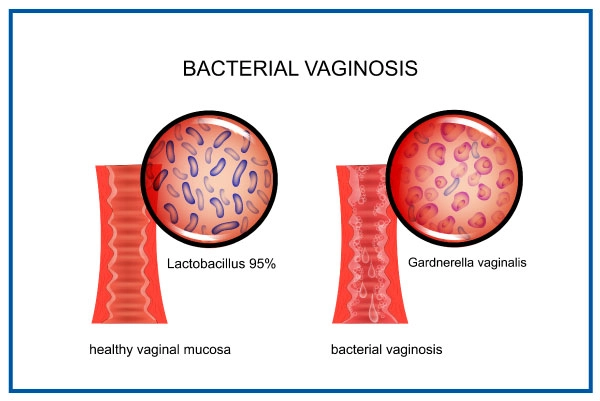
What is Bacterial Vaginosis?
The vagina naturally contains different types of bacteria. Normally, the body maintains a perfect balance between the various bacteria and works to prevent certain types of bacteria from getting out of hand. However, this subtle imbalance can lead to bacterial vaginosis (BV). Bacterial vaginosis (BV) is a vaginal infection caused by bacteria. This is the most common cause of abnormal vaginal discharge in women of childbearing age (women who are not yet menopausal). Bacterial vaginosis can cause a "fishy" odor and vaginal inflammation in some women. Others may have no symptoms. It is associated with poor obstetric and gynecological outcomes, including postoperative infections such as preterm birth and hysterectomy. It can make women more susceptible to sexually transmitted diseases, especially HIV. Let us look into the various symptoms of Bacterial Vaginosis, causes, risk factors, preventions, diagnosis and treatment in detail.
Get a second opinion from trusted experts and makeconfident, informed decisions.
 Get Second Opinion
Get Second Opinion
Symptoms of Bacterial Vaginosis
Symptoms of BV do not usually appear. When it occurs, though, these are some of the possibilities:
- Burning feeling when you pee
- Fishy smell that gets stronger after sex
- Itching
- Thin white, grey, or green discharge.
Causes of Bacterial Vaginosis
Bacterial infections are caused by the transmission (passing) of bacteria. Bacteria can be contracted from other individuals, the environment, or by consuming contaminated food or water. When exposed to microorganisms, anyone can become ill. A weaker immune system, on the other hand, puts you at greater risk of serious bacterial infections. Certain diseases and drugs might weaken your immune system by suppressing it. Even germs that are regularly found in your body might pose a threat to your health.
Risk factors of Bacterial Vaginosis
BV can affect anyone who has a vaginal opening. These factors can increase the chances of getting it:
- Frequent use of vaginal deodorants and douches.
- Using scented soaps and a perfumed bubble bath
- Bathing in water laced with antibacterial substances
- Using a strong detergent to wash undergarments
- Having sex with a new partner and smoking with numerous sex partners
Complications of Bacterial Vaginosis
Bacterial vaginosis has been linked to an increased risk of various health issues, including cancer.
- If one has a hysterectomy or other surgery while having BV, they might get a bacterial infection.
- Risk of developing Herpes, chlamydia, or gonorrhoea.
- Possibility of less success in fertility therapies such as in vitro fertilisation
- Risk of developing the pelvic inflammatory disease (PID), fallopian tube, and ovarian infection.
Diagnosis for Bacterial Vaginosis
Signs, symptoms, and lab testing are used to make a diagnosis. If the doctor detects something unusual during a physical checkup they may:
- Ask about the medical history: Any prior vaginal infections or sexually transmitted illnesses may be brought up by your doctor.
- Examine the pelvis: During a pelvic exam, the doctor visually inspects the vagina for symptoms of infection and inserts two fingers into the vagina while pressing on the belly with the other hand to look for evidence of disease in the pelvic organs.
- Check a sample of vaginal secretions: This can be done to see whether the vaginal flora has an overabundance of anaerobic bacteria. The doctor may use a microscope to analyze the vaginal secretions for "clue cells," bacteria-covered vaginal cells that indicate bacterial vaginosis.
- Test your vaginal pH: By inserting a pH test strip into your vagina, the doctor can determine the acidity of the vagina. Bacterial vaginosis is indicated by a vaginal pH of 4.5 or above.
Treatment for Bacterial Vaginosis
BV can affect anyone who has a vaginal opening. These factors can increase the chances of getting it:
- Antibiotics (metronidazole, clindamycin, and tinidazole) might be prescribed by the doctor to treat BV. This might be a pill that patients swallow or a lotion or gel that patients apply to the vaginal area. Most treatments will take 5 to 7 days to complete. Even if the symptoms go away, finish all of the medication.
- Because BV can be transmitted through sex, avoid sexual contact until you've finished the prescription and the symptoms have subsided. Whether the spouse is a woman, she may wish to consult with her doctor to see if she needs treatment.
- Even when BV has been treated and gone away, it frequently reappears. If this happens, you'll almost certainly need to take antibiotics for a longer period of time.
- If you're using an IUD and the BV keeps returning (recurrent BV), they should chat to the doctor about switching to a different kind of birth control.